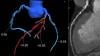
An interview with Ehtisham Mahmud, M.D., FSCAI, chief, Division of Cardiovascular Medicine, executive director of medicine, Cardiovascular Institute, director of interventional cardiology and cardiac cath lab at UC San Diego Medical Center, and president of the Society for Cardiovascular Angiography and Interventions (SCAI). He explains the how cardiology departments in the U.S. are now postponing cardiovascular procedures due to novel coronavirus (COVID-19, SARS-CoV-2) containment efforts and new guidelines from Medicare calling for delay of all elective procedures in the country.
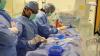
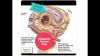
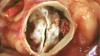
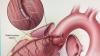
Mahmud explains how patients are being prioritized, with acute myocardial infarction patients or others with acute, life-threatening conditions, or at high risk for a near term hospital admission, will still receive cardiac catheterizations, cardiovascular surgery or structural heart procedures for MitraClip and transcatheter aortic replacement (TAVR) under certain circumstances. All other procedures are being postponed until further notice based in the spread and infection rates of COVID-19. He said most hospitals, including his own, are moving to telehealth visits via phone or online to continue clinic work with patients, including those with chronic conditions such as heart failure.
The Centers for Medicare and Medicaid Services (CMS) announced March 18, 2020, that all elective surgeries, and non-essential medical, surgical and dental procedures should be delayed during the coronavirus outbreak. This move is three-fold.
1. It is to help with containment efforts by reducing patient and family travel to hospitals, which are at the center of the COVID-19 outbreak.
2. Delaying procedures will help preserve and inventory of personal protective equipment (PPE), hospital beds and ventilators and other medical supplies.
3. With the start of social distancing and the shut down of all large gatherings, this has severely impacted blood drives and other blood donations, so the nation's blood banks have severely limited supplies.
“The reality is clear and the stakes are high — we need to preserve personal protective equipment for those on the front lines of this fight,” said CMS Administrator Seema Verma.
This will not only preserve equipment but also free up the healthcare workforce to care for the patients who are most in need. Additionally, as states and the nation as a whole work toward limiting the spread of COVID-19, healthcare providers should encourage patients to remain home, unless there is an emergency, to protect others while also limiting their exposure to the virus.
Read Mahmud's SCAI President's letter The Evolving Pandemic of COVID-19 and Interventional Cardiology
Related Cardiology Related COVID-19 Content:
ACC COVID-19 recommendations for the cardiovascular care team
VIDEO: What Cardiologists Need to Know about COVID-19 — Interview with Thomas Maddox, M.D.
The Cardiac Implications of Novel Coronavirus
ESC Council on Hypertension Says ACE-I and ARBs Do Not Increase COVID-19 Mortality
VIDEO: Imaging COVID-19 With Point-of-Care Ultrasound (POCUS)
CT Provides Best Diagnosis for Novel Coronavirus (COVID-19)
Radiology Lessons for Coronavirus From the SARS and MERS Epidemics
Deployment of Health IT in China’s Fight Against the COVID-19 Epidemic
Emerging Technologies Proving Value in Chinese Coronavirus Fight
Radiologists Describe Coronavirus CT Imaging Features
Coronavirus Update from the FDA
CT Imaging of the 2019 Novel Coronavirus (2019-nCoV) Pneumonia
CT Imaging Features of 2019 Novel Coronavirus (2019-nCoV)
Chest CT Findings of Patients Infected With Novel Coronavirus 2019-nCoV Pneumonia
Additional COVID-19 Resources for Clinicians:
ACC COVID-19 Hub page
Johns Hopkins Coronavirus Resource Center with inteavtive map of cases in U.S. and worldwide
World Health Organization (WHO) COVID-19 situation reports
World Health Organization (WHO) coronavirus information page
U.S. Food and Drug Administration (FDA) COVID-19 information page
Centers for Disease Control (CDC) COVID-19 information page
Centers for Medicare and Medicaid Services (CMS) frequently asked questions and answers (FAQs) for healthcare providers regarding COVID-19 related payments