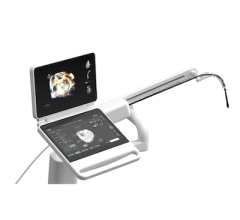
GE recently released its Vivid E9 BT11 (breakthrough 2011) version echo system, offering several workflow improvements.
The biggest trend in cardiovascular ultrasound is the adoption of 3-D/4-D echo systems for better images, more data, better measurement quantification and faster workflow. Other key trends include software to speed workflow with fewer keystrokes and to enhance quantification, miniaturization, increased use of tissue strain imaging and expanded use for operating room and cath lab procedures.
Increasing Speed, Workflow, Accuracy
Workflow improvements are badly needed to help reduce the time studies take to perform. “Twenty years ago, an echo exam took about 45 minutes and today it still takes about 45 minutes,” said Benita Graul, Siemens marketing manager for cardiac ultrasound. “But, with 3-D echo, we may be able to help lower the time it takes. I think this is the future, along with all the automation.”
3-D/4-D volume imaging allows a set of data to be captured for an entire 3-D area of the heart in motion, similar to computed tomography (CT) or magnetic resonance imaging (MRI) datasets. The data can then be sliced through, rotated and manipulated to gain views of the specific areas of heart anatomy in motion along any axis. The advantage of 3-D acquisition is that three standard echo exam views can be extracted from the single volume, saving imaging time. Conventional 2-D echo slices can also foreshorten images based on the angle of the transducer and the position of the anatomy. The use of a 3-D volume can eliminate foreshortening by making is easier to identify and correct.
“If I give you a slice of bread, you can make an assumption about what the entire loaf of bread looks like,” Herbert Dyal, BHS, RDCS, RDMS, clinical sales specialists, GE Healthcare, said, explaining 2-D versus 3-D echo. “If you are given several slices of bread, it is a lot easier to visualize the entire loaf.”
At ACC 2011 in April, Siemens released the SC2000 6.1 version of its 3-D volume cardiac echo system. The newest version automates measurements to help speed workflow. Instead of placing dots to delineate the left ventricle, the system uses a database of clinical images to automatically determine the borders of the left ventricle in the three standard echo views. It then highlights the ventricle and automatically figures the ejection fraction without user intervention. Siemens coined the term “GPS for the heart” for this new feature. Once a volume is acquired, the sonographer can “clip” the optimal image in a cycle to make measurements, and one click will enable the software to automatically capture measurements based on three heartbeats.
GE Healthcare recently released its Vivid E9 BT11 (breakthrough 2011) version echo system, which offers several workflow improvements. These include fewer keystrokes to get a specific view. It also uses an algorithm to automatically extract specific views and to automatically define left ventricular borders and determine ejection fractions with very little user interface.
“There is always a drive for better image quality and there have been some major improvements in the past five to 10 years,” said L.J. Gage, director of marketing and general imaging, ultrasound division, Philips Healthcare, explaining better images lead to better quantification and improved diagnosis and treatment. While software algorithms have helped produce clearer images, some processing is now being done in the transducer (as in the case of Philips’ latest generation X51 transducer). This helps reduce image-processing time by eliminating the need to first send large amounts of raw data to the console to process.
Tissue Strain/Speckle Tracking
Using software to track the individual speckles that make up echo images, systems can measure time and distance involved during movement. This allows measurement of strain to show contractibility of cardiac tissue.
“Over the past five years what I have seen in cardiology is a definite increased interest in tissue strain Doppler,” Gage said. It allows assessment of ischemia, aids placement of biventricular pacing leads and valuation of heart function. Speckle tracking echo also can determine lead positioning for cardiac resynchronization therapy (CRT) devices.
Trends into the Future
“There has been an emergence of interventional ultrasound in the cath lab and in the hybrid operating room,” Gage said. “Interventional use is definitely a growing area to aid in device placement and because of concerns over patient radiation exposure.”
Over the next five years, fusing ultrasound images with MRI or CT datasets will help improve diagnosis and procedural navigation. Evidence-based clinical decision support software will be introduced to act as a second set of eyes. It can red flag values that are out of range and offer suggested diagnoses. It could also help guide less experienced sonographers to acquire better images.
There will likely be a linkage with intracardiac echo (ICE) and transesophageal echo (TEE), especially for better visualization of valve disease, predicts Al Lojewski, vice president and general manager, cardiovascular ultrasound, GE Healthcare. This will become more important as TEE is used to image transcatheter valve implantation to assess placement and positioning.
Comparison Chart
This article served as an introduction to the cardiac ultrasound comparison chart in the May-June 2011 issue of DAIC. The chart included ultrasound systems used in cardiovascular evaluation. It includes systems designed for in-office evaluation, high-end systems for echo labs and systems used to help guide interventional and surgical procedures. To access this chart, visit www.dicardiology.net/comparison-charts?t=57.
Companies that participated include:
Hitachi Aloka Medical
www.aloka.com
Esaote North America
(formerly Biosound Esaote)
www.esaoteusa.com
GE Healthcare
www.gehealthcare.com
Philips Healthcare
www.philips.com/iE33
Siemens Medical Solutions
www.medical.siemens.com
SonoScape
www.sonoscape.net
Toshiba America Medical Systems
www.medical.toshiba.com
Zonare Medical Systems
www.zonare.com


 January 28, 2026
January 28, 2026