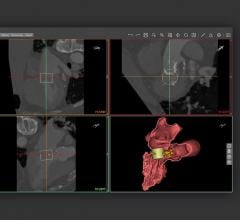
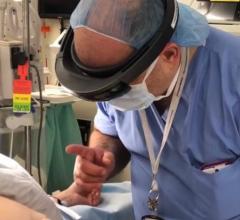
MSCTA helps with CTO, which accounts for 10 to 15 percent of patients undergoing coronary angioplasty.
Delivering vivid and insightful CT images of the coronary vessels directly into the cardiac catheterization laboratories (cath labs) has proven very effective by helping save staff from re-acquiring images of the heart and boosting patient throughput. But CT images are only part of the bigger picture. As cath labs take on more complex and diverse procedures, advanced X-ray equipment and visualization tools are enabling cath labs to go from highly specialized research centers to multipurpose facilities.
Expanding the Mix
The increased adoption of IT solutions to increase workflow efficiency in cardiology has changed the role of the cath lab. Several new, noncoronary angiographic procedures are now taking place in this formerly angio-only room.
“Meanwhile, angio lab procedure volume has grown steadily as the procedure mix has broadened to include a variety of peripheral vascular and other noncoronary angiographic procedures,” indicated Lorna Young, senior director, Market Research, IMV Ltd.
According to a report by IMV, from 1998 to 2004, the proportion of therapeutic applications, including angioplasties, vascular access, stent placements, thrombolytic therapy, IVC filter placements and embolization, has increased from 38 percent of the noncoronary angio procedures to 45 percent.
MSCTA Bursts into Light
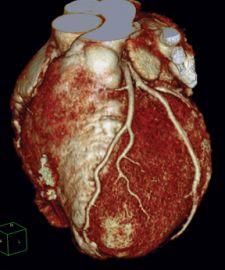
Over the last few years, we have seen multislice-CT for coronary angiography (MSCTA) gain wide acceptance thanks to its minimally invasive nature and ability to visualize both the coronary artery lumen and coronary plaque.
While CTA has been achieved on 64-slice and dual-source CT systems, it has been limited by lower temporal resolution. With the introduction of the AquilionONE 320-slice CT system by Toshiba America Medical Systems and with Phillips’ new Brilliance iCT 256-slice CT scanner, the ability to capture dynamic images of entire organs is extremely promising for noninvasively visualizing disease development and vulnerable plaque. One procedure where MSCTA can be especially helpful is with chronic total occlusions (CTO), which account for 10–15 percent of patients undergoing coronary angioplasty. The challenge for interventional cardiologists is the assessment of CTOs and guidance for the interventional approach
According to Robert S. Schwartz, M.D., FACC, medical director, Minnesota Cardiovascular Research Institute, Minneapolis Heart Institute Foundation, MSCTA performed prior to a CTO procedure permits the interventionalist to ascertain the location, length and tortuosity of the lesion with location and type of plaque, for example, calcification versus soft plaque. To assist clinicians in answering these questions prior to CTO procedures, several manufacturers are developing software specifically for cath lab and interventional procedures to fuse images on stored data in real time.
MSCTA also has applications for the determination of stent patency, as it can visualize the contrast-containing lumen within stents to determine the presence of stent restenosis. According to Dr. Schwartz, the future will allow interventional coronary, cardiac and valvular procedures to be performed in real or near-real time in three dimensions. This is prompting interventional cardiologists to become trained on MSCTA and learn how to manipulate 3D images.
Broadening the Cath Lab’s Scope
Many patients seeking treatment for coronary problems also have systemic vascular diseases, requiring interventionalists to also treat noncardiac vascular organs and perform interventions in other parts of the body’s vascular system.
The diversification of procedures performed in the cath lab is driving demand for cardiac X-ray equipment and digital processing capabilities, according to analysts at Frost and Sullivan (F&S). Subsequently, cath labs have experienced double-digit growth, and the 3D/4D visualization market, which has become more pervasive in the radiology and cardiology fields, grew by 14 percent in 2006. Manufacturers have responded by developing technologies designed to offer greater flexibility, improve image quality and aid in streamlining workflow.
Philips recently introduced its Live 3D transesophageal echocardiogram (TEE) probe, the X7-2t. Live 3D TEE technology is the result of combining and miniaturizing the 3D power of xMATRIX and the outstanding image clarity of PureWave crystal technology in one transducer. New views of cardiac structure, pathology and function can be realized.
John Carroll, M.D., chief of Cardiology and director of Cardiac and Vascular Center, University of Colorado Hospital, uses Philips’ Live 3D TEE. He explained, “The cardiac cath lab is really evolving from a mixture of diagnostic and therapeutic procedures to a greater percentage of therapeutic procedures. Now we see the emergence of vascular interventions, including cardiovascular stenting. But even more significant is the change to structural heart disease interventions to either close holes in the heart and the treatment of heart disease, which is emerging from the investigative arena to clinical care. We expect that impact to play out in the next five years.”
The emergence of diverse and complex procedures requires innovative tools to perform these vascular and structural interventions. According to Dr. Carroll, this need is exactly where real-time TEE technology is playing a significant role, and it “is likely to evolve to be the predominant image-guided modality for structural heart disease interventions.” He added, “It is noteworthy because it is the first time ever that real-time three-dimensional imaging has been used to perform interventions.” In the past, X-ray and 2D ultrasound were predominantly used.
This new development has profound implications on how the cath lab needs to be restructured. Firstly, interventionalists and healthcare providers must become familiar with the technology.
“I think for the procedure room there is a need for training on these technologies because technology is only as good as the skills you have in using them,” indicated Dr. Carroll. However, he added, “I also think that it will be easier for new people to the field to be trained. Much of the learning curve is the time needed to learn how to interpret and navigate in 3D images, being shadow or projection images, where you really have to move the gantry around to get the various perspectives of the coronary tree. Two-dimensional ultrasound images are slice images that need to be interpreted in the context of the whole 3D structure.” Obtaining 3D images automatically instead of having to interpret 2D images may shorten this learning curve and shortens the time needed for more experienced physicians to interpret images.
Given the more complex procedures, the cath lab also needs to be reconfigurable to allow multiple access points to the patient. The X-ray system requires the flexibility of
moving the gantry to different positions since the echocardiogram machine needs access to the patient’s left side. If a procedure requires anesthesia, the patient’s head end will also need to be accessed. In addition, more monitors are needed since a variety of imaging techniques are displayed including, X-ray, fluoroscopy, human dynamics, ultrasound and 3D coronary images.
Although technology prompts changes in training and restructuring the layout of the cath lab, the benefits of Live 3D transesophageal echocardiogram outweigh these inconveniences. Clinicians will gain from enhanced visualization, reduction in cardiologists’ dependency on the expensive use of fluoroscopy and improvement of patient safety by reducing X-ray dose, according to Dr. Carroll. “The advantages are first of all improvement in image guidance in the interventions in that there is more realism to the visualization. Three-dimensional imaging fits better into the inherent visual processing in the human mind. It reduces the dependency on the physician of having to put together the 2D images and reconstruct in their head what the 3D target really looks like.”
The benefit on patient outcome is yet to be fully understood, according to Dr. Carroll. More time is needed in order to determine how to effectively use the image guidance in order to improve the outcome of interventions. However, he noted, “Ultimately, what it would bring to the patient is the very simple bottom line: If the doctor can see what they are working on, they’ll do a better job. Hopefully, improving success rates, reducing procedure time and doing a better job at fitting devices in the heart.”
He went on to address the future implications of TEE, which could involve automated navigation systems in performing interventions, including robotic systems. “[Robotic systems] need the 3D imaging technologies to get off of the ground so the improvements in image-guided interventions by different modalities and different tools open opportunities for other advances in therapeutic procedures and other advances in technologies to assist the performance of interventions,” said Dr. Carroll.
Robotics on the Move
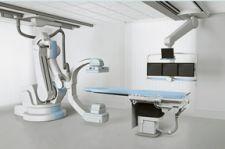
Perhaps one such robotic system may be here sooner than you think. Already in the first stages of development is Siemens’ Artis zeego. J. Fritz Angle, M.D., associate professor of Radiology and director of Interventional Radiology at University of Virginia Health Systems, is currently using the Artis zeego on an investigational basis. The revolutionary new Artis zeego features a multi-axis C-arm that employs robotic technology to extend imaging capabilities through virtually unrestricted C-arm positioning.
“The first clinical advantage we discovered was that the C-arm, the image detector device, can move up and down, side to side, and that allows us to reposition the fluoro image more quickly and more accurately and speeds up the process,” said Dr. Angle. Other advantages include its cone-beam syngo DynaCT capability, which shows a larger field of view with the click of a button. “The software allows the arm to click the whole chest or abdomen in one view. That’s quite a big plus for us,” he noted.
Dr. Angle also emphasized on the improved image quality. “We’ve found a stepping C-arm so we’re getting very nice image quality. There’s no vibration since there’s no stepping table. We have less equipment on the ceiling so the operating room lights are not obstructed. The lighting is more favorable to basic procedures.” He added, “What’s exciting to me is this robot arm platform allows the C-arm to move in a very precise, reproducible way, and I think it’s going to make it possible to do imaging in new ways that we haven’t seen before. The platform is there; all we need is the software development.”
Greater diversification in procedures done in the cath lab is accompanied by an extended portfolio of 3D imaging tools used perform them with. Another reason why, according to Dr. Schwartz, “interventionalists would be well served to become familiar with cross-sectional anatomy and the tools to manipulate cardiac 3D image sets.”

 May 12, 2020
May 12, 2020