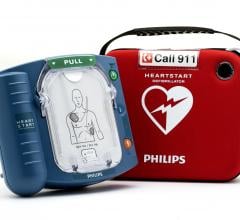
Automatic external defibrillators (AEDs), such as this Physio-Control LifePak CR Plus, are increasingly deployed in hospitals as a first-line response to sudden cardiac arrest. Many times they deliver a shock before the crash cart arrives.
Early defibrillation is often referred to as the “critical link in the chain of survival,” according to the American Heart Association (AHA). But even in a hospital setting, the time from when a person suffers cardiac arrest to when they undergo defibrillation varies widely.
Recently, automated external defibrillators (AEDs) — small, portable defibrillator devices — have experienced a spike in popularity. More hospitals and clinics are deploying the inexpensive, easy-to-use AEDs as a vital first-response measure before crash carts arrive.
Every minute a cardiac arrest victim goes without defibrillation, the odds of survival drop 7 to 10 percent, states the AHA’s Web site. Defibrillators deliver an electric shock to the heart to restore its regular rhythm. In these high-risk scenarios, AEDs can literally mean the difference between life and death, if administered properly.
“It’s been shown repeatedly that the delivery of the first shock is very much associated with the likelihood of survival. I’m a strong advocate of making early defibrillation as rapidly available as possible,” said Roger D. White, M.D., consultant in the departments of anesthesiology and internal medicine/cardiovascular diseases, Mayo Clinic College of Medicine, Rochester, Minn. “I just think we have some unresolved issues to clarify in order to make this a fruitful reality.”
The Mayo Clinic Approach
At the Mayo Clinic, hundreds of AEDs from Zoll Medical Corp. were distributed a couple years ago throughout the institution, including all the nursing stations. Mayo nurses are trained to use AEDs in collaboration with cardiopulmonary resuscitation (CPR) performance, said Dr. White, who works closely with the Olmsted County Early Defibrillation Program for the city of Rochester. AEDs are much more likely to be used, and be more beneficial, in general wards outside of intensive care units, or in clinical facilities, he added.
“Our assumption is that we should be able to improve survival by using a means to make more rapid defibrillation more quickly available before crash carts arrive,” he said. “Having said that, we don’t have data in sufficient numbers to show that we have improved survival rates yet. It’s too early to tell.”
Despite the lack of hard data, anecdotal evidence abounds of patients’ experiencing “return of spontaneous circulation” after being shocked with an AED, before the crash carts arrive. “But these are isolated experiences,” he cautioned.
Findings from a 2009 study published in the Archives of Internal Medicine, “Hospital Variation in
Time to Defibrillation After In-Hospital Cardiac Arrest,” provides some early evidence that rapid defibrillation with these devices in hospital settings will improve survival, said Dr. White. The study shows a link between hospitals in the top-performing quartile for defibrillation time and higher survival rates at discharge.(1) The authors concluded the study with a call for more research to explore potential ramifications: “Given its association with improved survival, future research is needed to better understand best practices in the delivery of defibrillation at top-performing hospitals.”
AEDs play a critical role as adjuncts to critical crash carts, and are not meant to be alternatives, he emphasized. “We will always need the full-fledged crash cart to provide ongoing resuscitative interventions, not everyone is going to benefit from shock,” Dr. White said. The combination of well-trained people and well-maintained devices provides a promising prescription for survival, he added.
Changing Demographics
The demographic of cardiac arrests in hospital settings has changed significantly in the past five to 10 years, said Kenneth Korr, M.D., chief of cardiology and medical director, division of cardiology, The Miriam Hospital in Rhode Island. As the chair of the hospital’s code review subcommittee, Korr has observed an overall shift from primarily ventricular tachycardia and ventricular fibrillation codes to more hypertensive, respiratory-leading-to cardiac arrest types, Dr. Korr said. “I think some of the reason for that is that a lot of our very sick cardiac patients already have defibrillators,” he said. “So that immediately takes a portion of the population out of the possibility of having a [certain] code in the hospital.”
The hospital installed about two dozen Philips Healthcare AEDs throughout the facility several years ago. But, it is seeing less “traditional” arrhythmias in the wards that typically merit AED intervention. Dr. Korr estimates that one or two out of 100 codes require the use of AEDs, typically at night when a nurse is alone. Although few and far in between, in certain cases, “an AED is instrumental in getting them diagnosed and shocked,” he said. “I can remember a few dramatic cases where a nurse runs in with an AED, puts it on, shocks the patient, and by the time the crash cart comes in, the patient is awake and asking what happened.”
Dr. Korr agrees that AEDs, despite advances in technology and effectiveness when used correctly, are not meant to replace crash carts in a hospital setting. “The crash cart always shows up,” he said. “It just shows up second. The AED is the quickest thing a person can grab to get a cardiac rhythm.”
User-Friendly Appeal
Part of the appeal of AEDs, and reason why they have become popular in public arenas, is they are designed to be extremely intuitive and user friendly. Most hospitals train their nurses and other pertinent staff on AEDs as part of their basic life support training. “It’s pretty easy to teach: 1,2,3, put patch on, get rhythm. The AED tells you what to do,” Dr. Korr said. “That’s one of the tremendous advantages of these devices.”
Recent advances in the technology have maintained the device’s core simplicity, while becoming increasingly sophisticated through features such as superior sensor sensibility, voice prompts and video screens. Zoll Medical Corp. recently introduced a new code-ready AED, the R Series, that actually “coaches CPR” by providing users with feedback to help achieve proper compression rate and depth. “This technology is really important for influencing outcome because it’s not just about the shock,” said Annette Z. Fasnacht, senior director of hospital marketing for Zoll.
Another AED line, the R Series Plus, can function as a simple AED or as a full-fledged defibrillator when the code comes alive. “When the first responder walks up, it just has one button on it that says AED. It looks like a regular defibrillator, but doesn’t have all the buttons that make people scared. But when the code comes alive, all the other buttons come up in a backlit way,” she says. “What we’re trying to do is give hospitals the best of both worlds. Give them a very simple AED and hide everything else, and still have a full defibrillator option [when needed].”
Michael Leonard, M.D., national physician leader for patient safety for Kaiser Permanente, was in charge of purchasing AEDs nationally for Kaiser. He is very familiar with the Philip’s Healthcare AED technology. “As someone who was involved with buying them, installing them [at Kaiser clinics] and teaching how to use them, I think the design is great,” he said.
“The beauty of the AED is that all you have to do is push the button and pick up one of the pads, and the device is sophisticated enough that it gives voice prompts,” said Dr. Leonard. “Someone who is a stranger can pick it up and use it quite effectively. They are very thoughtful devices.”
Resistance From Hospitals
Dr. Leonard points to a lingering reluctance on behalf of some hospitals to recognize the need for, and benefits of, installing AEDs. This “fundamental disconnect” stems in part from professional pride, the need to defend their hospital’s cardiac arrest response times, and the feeling that these devices are not truly needed inside hospitals, he said. But even within medical settings, Dr. Leonard argued not all the staff will be effective at using advanced life support defibrillators.
“When you’re in an environment where those things do not happen frequently, they tend to not do it very well because they’re scared or don’t know how to use the equipment or even where it is,” he said. “When you’re stressed and doing something that’s scary, you want it to be simple and predicable.”
Selling Points
In short, AEDs play an important role in simplifying what can be a chaotic and high-stakes situation. “The argument I make is why don’t we make it simple for you. This is a way to do something that’s going to make it real easy for you until the cavalry comes.” Leonard suggests that clinics store the devices behind the front desk, where there is usually a person nearby.
Another selling point in favor of AEDs is their value proposition, he added. “They are certainly substantially cheaper. You can get an AED for around 20 cents on the dollar compared to full-fledged external defibrillators,” he said. Leonard recommends that hospitals and clinics keep their existing crash carts, but consider investing in AEDs when it comes to purchasing new equipment. “No one wants to take the crash cart away. It’s kind of the security blanket.”
Future Expansion
Looking ahead, Dr. White of Mayo predicts an expansion of AEDs in hospital settings — with hopefully hard data providing all the ammunition necessary. “I think a lot of hospitals certainly embrace the understanding that the more rapidly they can defibrillate someone, the greater the likelihood of a favorable outcome. Hospitals are very tuned in to that reality,” he said.
References:
1. Paul S. Chan, M.D., et al., “Hospital Variation in Time to Defibrillation After In-Hospital Cardiac Arrest.” Archives of Internal Medicine. Vol. 169, No. 14. July 27, 2009.
2. Prehospital Emergency Care 14. Suppl. 1. Abstract No. 35. Page 15. January 2010. (Published in abstract form only).



 January 13, 2026
January 13, 2026