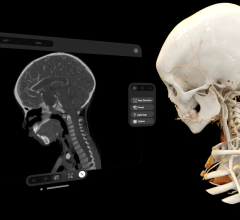
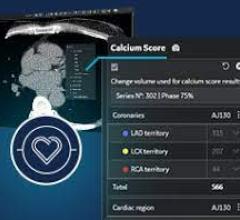
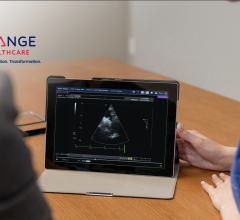
Many CIIMS integrate with cath lab hemodynamic and reporting systems, such as McKessons Horizon Cardiology.
Over the past five years, two major changes have occurred in cardiovascular information systems (CVIS) and cardiovascular picture archiving and communications systems (PACS). There is a migration from disparate reporting and imaging systems toward a single, unified system. The second trend is easier access to patient information using Web-based and cloud technology.
These combined CVIS/PACS are referred to as cardiovascular image and information systems (CIIMS).
“The real advantage of these systems is the integration of various reports,” said PACS consultant Gary Reed of Integration Resources. “It provides easy access to all these reports on one, single system and from one log-in. It allows for seamless integration between images and these reporting systems. It really improves workflow.”
He added these systems also update information automatically as new data or images are saved, giving a more real-time look at a patient’s condition.
Most CIIMS offer access to imaging and reporting templates for computed tomography (CT), magnetic resonance imaging (MRI), nuclear imaging and cardiac ultrasound. Many systems integrate with cath lab hemodynamic and reporting systems. They generally offer an advanced visualization software package, many times in partnership with a third-party vendor. Electrocardiogram (ECG) reporting systems have been integrated with these systems over the past few years as well.
Wider Access to Data
There is a big trend away from single-hospital, server-based systems toward Web-based servers, or third-party, cloud solutions. These Web-based technologies allow easy access to the integrated information and images from any location. This significantly increases workflow between different doctors who are treating the same patient, or as a patient moves through various hospital departments (such as the emergency room, radiology and the cath lab).
This goes hand-in-hand with the rapid adoption of regional health information organizations (RHIOs), also called health information exchanges (HIEs), to share patient information between multiple hospitals, clinics, doctor’s offices and specialists.
“Hospitals want to be able to disseminate patient information over a large area network,” Reed said. “These cloud systems allow unlimited access to patient data between unaffiliated hospitals, healthcare systems and physicians to create a cloud-based HIE.”
There are few, true cloud systems, Reed said, but he expects these systems to proliferate and become the standard PACS platform in the next decade. Most of these cloud solutions will be offered through third-party vendors, which Reed believes will eventually phase out the role of individual hospital information technology (IT) departments in maintaining this ever-increasing amount of data. This offering of “software as a service” has already taken hold in the image archiving and advanced visualization markets.
“The trend definitely has been a move toward thin-clients (Web-based) as opposed to thick-client (dedicated workstations) based systems,” said Michael J. Cannavo, president of PACS consulting firm Image Management Consultants LLP.
Thick-client systems offer slightly better performance and there is no shared bandwidth, he explained. However, Web-based systems are becoming more popular, he said, because they are easier to deploy, cost less and do not require dedicated network connections.
Differences in Systems
Reed said not all vendors are at the same level of integration or may not cover all of the cardiac imaging modalities and reporting systems. While some vendors offer a unified, single database, others can weave together several existing databases so all of a patient’s cardiac images and information appears in one place.
Despite the healthcare industry standardizing on DICOM and HL-7 file formats, Cannavo said most data is still stored in proprietary formats and does not address areas such as gray scale presentation states (GSPS) and image annotation overlays. This also does not allow vendors to share data and create vendor-neutral systems.
Meaningful Use
In July, federal regulations were issued to clarify the definition of meaningful use, enabling federal stimulus money and healthcare IT reforms to move forward. However, the regulations only apply to clinical information systems and exclude PACS. All the large vendors are making commitments to their customers that they will provide whatever is needed to meet any new requirements.
“I would not work with any vendor that cannot include that language in the contract,” Reed said.
Cannavo said the meaningful use definition covers Stage I of the Health Information Technology for Economic and Clinical Health Act of 2009 (HITECH), which is part of the economic stimulus package. It covers general practice electronic medical records (EMRs). Stage II will include meaningful use criteria for specialties, including radiology and cardiology. The meaningful use criteria for these specialties should be effective by 2013.


 December 23, 2025
December 23, 2025