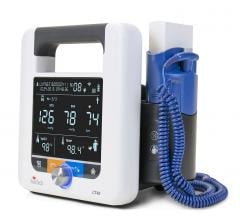
July 28, 2014 — Robert Smith, a cardiologist at Saint Francis Hospital and Medical Center in Hartford, Conn., released the results of his retrospective study designed to compare single in-office automated blood pressure readings to the average of multiple automated blood pressure readings. Blood pressure readings were collected on 187 adult patients using a Welch Allyn Connex Vital Signs Monitor (Model 6300) with Office Profile and automatic base-lining technology enabled. The quantitative analysis shows that blood pressure diagnosis varies over a range of consecutive readings suggesting that it can be important to calculate an average blood pressure in order to obtain the most accurate representation of the true blood pressure in the doctor’s office.
“The purpose of this study was to compare single in-office blood pressure readings to average in-office blood pressure readings and observe the differences in accuracy and potential variation in diagnoses between the two methodologies,” said Smith. “An inaccurate diagnosis of high blood pressure could lead to the overprescribing of blood pressure-lowering medications, which may result in adverse events associated with hypotension, which is the last thing we want for patients. As doctors our mantra is and always will be, ‘first, do no harm.’”
To mimic the true office experience, Smith and his staff started the first blood pressure measurements at varied times after patients entered the exam room one to three minutes into the test. Five subsequent measurements were taken at intervals of one minute, and the monitor automatically calculated a recommended average that included up to six of these measurements. Several factors can affect the accuracy of blood pressure measurements including, but not limited to, talking or active listening, distended bladder, cuff over clothing, smoking within 30 minutes of measurement, back unsupported or an unsupported arm while sitting or standing.
Results showed that with averaged readings half of the patients previously classified as hypertensive using the single reading methodology were reclassified into pre- and normotensive categories. More than half of the patients that would have required the physician to provide hypertensive care did not display the medical need with an averaged reading.
“The study provides observational data that supports the premise that patients may significantly benefit from the use of automated, unattended blood pressure measurement techniques that adopt blood pressure averaging,” said Pooja Sinha, manager, Vital Signs Solutions at Welch Allyn. “Unfortunately, misdiagnosis can lead to unnecessary lifestyle changes for patients, thus decreasing quality of life. Patients that initially would have been categorized as pre-hypertensive based on a single first reading were classified as normal based on the average readings. Finding the average could make for a better outcome for patients.”
For more information: www.welchallyn.com

 February 14, 2022
February 14, 2022