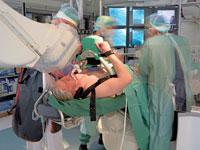
The consistent, effective compressions LUCAS provides help maintain consistent, appropriate coronary perfusion pressure and cerebral circulation. With LUCAS, the cath lab staff at Skane University Hospital-Lund has been able to save more lives in cases requiring prolonged resuscitation during PCI.
In the past, when a patient suffered a prolonged cardiac or circulatory arrest during percutaneous coronary intervention (PCI) in the catheterization laboratory (cath lab) at Skane University Hospital–Lund, it was a catastrophic event. As any interventional cardiologist knows, the mortality rates in these situations are very high because it is essentially impossible to perform effective manual chest compressions while continuing PCI, especially in cases where prolonged resuscitation is required.
“The problem in the cath lab is that you have all these X-ray tubes that are in the way,” says Göran Olivecrona, M.D., Ph.D., associate director of the Coronary Intervention Unit at Skane University Hospital–Lund in Sweden. “It’s difficult to squeeze yourself in and provide good compressions. The other concern is that if you have someone standing under the X-ray tube, they are being exposed to very large amounts of radiation and obstructing fluoroscopic images.” Another challenge is that the cath lab table is often flexible and doesn’t offer a firm base, making chest compressions even more physically demanding and less effective.
As is common practice, one way Olivecrona and his team dealt with this situation in the past was to lower the table out of the way of the X-ray tubes to allow a staff member to perform compressions. Then they would move the table back up and the operator would work on the intervention without compressions. “Many operators have felt the horror of trying to work on coronary arteries on a heart that is arrested in a few seconds before lowering the table again to return to manual compressions,” says Olivecrona. “You’re too rushed.”
In either approach, manual compressions have their limitations. “Even when performed in an ergonomic position, studies have shown – including some of our own – that resuscitator fatigue results in lower quality compressions over time,” says Olivecrona. “That’s why the first time I saw the fantastic blood pressure LUCAS could achieve and maintain consistently, I was amazed and immediately sold on it.”
Better Patient Outcomes
Since they began using the LUCAS 2 Chest Compression System in the cath lab at Skane University Hospital–Lund in 2004, the staff has found they were able to perform lifesaving procedures on patients even while they’re suffering prolonged cardiac or circulatory arrest during PCI. LUCAS is a portable, easy-to-use device that delivers effective, consistent, uninterrupted chest compressions according to current American Heart Association (AHA) guidelines and is mainly radiotranslucent.
“With LUCAS, we can continuously deliver good compressions and at the same time have the X-ray tubes focused over the heart so we can see what we’re doing and continue the PCI,” says Olivecrona. “We’ve had patients on LUCAS for up to 55 minutes who have survived and walked out of the hospital, which would not have been possible without LUCAS.”
Olivecrona and his team have found the consistent, effective compressions LUCAS provides help maintain consistent, appropriate coronary perfusion pressure and cerebral circulation. As a result, the cath lab staff at Skane Univesity Hospital-Lund has not only been able to save more lives with LUCAS in cases requiring prolonged resuscitation during PCI, but they have also been able to achieve more normal functioning neurological outcomes in these cases.
Virtually Unobstructed Fluoroscopic Imaging With Continuous Compressions
Because LUCAS is mainly radiotranslucent – except for the head and the piston – it allows the interventional cardiologists in the cath lab at Skane University Hospital–Lund to capture most fluoroscopy projections while the patient continues to receive consistent, guidelines-quality compressions. The following fluoroscopy projections can be captured in monoplane while LUCAS is attached to the patient: LAO cranial/caudal oblique; RAO cranial/caudal oblique; straight caudal; straight lateral; and straight cranial.
“Fortunately the available views are almost always the preferred angiographic views during PCI,” says Olivecrona. “So I can continue PCI with ongoing compressions from LUCAS and if I need to perform an especially high-precision maneuver, such as positioning a coronary stent, I can stop LUCAS for a few seconds to complete the procedure and I know I will have great circulation again as soon as I give the word to turn LUCAS back on.”
Safer, More Focused Working Environment
In addition to improving safety because staff can stay out of the X-ray field and don’t have to perform manual compressions in non-ergonomic positions for prolonged periods of time, the cath lab team at Skane University Hospital–Lund has also found that using LUCAS results in a much less stressful working environment.
“When people are actively doing manual compressions, it just brings up adrenaline levels in the room and people often make mistakes in these situations,” says Olivecrona. “With LUCAS stabilizing the patient’s circulation, a large burden of stress is relieved, which makes everyone feel more comfortable and the whole staff is more focused.” Olivecrona adds this is especially vital when he’s performing a technically complex PCI because he is better able to concentrate. In addition, staff that would have otherwise been performing manual compressions can focus on supporting his critical next steps.
“It gives us an added confidence to have LUCAS available in the cath lab,” says Olivecrona. “It’s not a complete disaster anymore when someone collapses on the table during a procedure. I would summarize and say the biggest thing is that we can save patients that we would have thought were impossible to save before LUCAS.”


 April 02, 2019
April 02, 2019 



