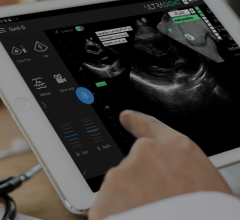
Toshibas 3D wall motion tracking is able to show dyssynchrony in this cardiomyopathy patient. A 3D LV display with bulls eye plot (top left) shows the late yellow color coded posterior area, and the corresponding time to strain curves.
Echocardiography has played an integral role in the diagnosis and treatment of millions of patients with cardiac diseases. Recent advances in echocardiographic technology have improved patient care and created novel ways to diagnose disease, which have had an immediate impact on patient management. Three-dimensional (3D) wall motion tracking is an exciting new development in quantitative echocardiography technology that can provide a more complete assessment of global and regional left ventricular function and has great promise for the clinical application of cardiac resynchronization therapy (CRT).
Improving Diagnosis for Cardiac Patients
The American Heart Association states that more than half a million patients undergo pacemaker implantation or CRT, each year. Approximately 30 percent of these patients (1) do not respond to the treatment, at an average cost of at least $30,000 (2) per patient case.
The clinical pathway for CRT has the potential to improve as advanced cardiac ultrasound technologies are improving. The ability to identify patients who will respond to CRT could also reduce costs to the healthcare system and may increase diagnostic accuracy.
Patients who present with heart failure often have abnormal electrical pathways that are associated with abnormal mechanical activation, known as dyssynchrony. Echocardiography can be used to evaluate their candidacy for CRT by first accurately assessing left ventricular (LV) ejection fraction, and potentially mechanical dyssynchrony. Current clinical guidelines use an electrocardiogram (ECG) to detect a delay in electrical activity through the heart. This is an imperfect marker of mechanical delays, and there is intense interest in measuring the mechanical delay or dyssynchrony using imaging. Although 2D ultrasound imaging has shown some initial promise, there are doubts that 2D imaging alone or in combination with the ECG can accurately and reproducibly determine dyssynchrony in everyday clinical practice.
It is a practical and important goal to define the mechanical activation of the heart more completely. This will help potentially guide the implanting doctor as to where to put the pacemaker lead wire to give the patient the best benefit from the therapy. Secondly, it may help identify the subgroup of patients who do not have enough mechanical dyssynchrony to respond to the therapy. In other words, it can be used to determine which patients do not have a chance to respond to CRT prospectively. Both ECG exams and 2D ultrasound imaging serve important clinical purposes, but are currently limited. Ideally, evaluating quantitative data using volumetric 3D voxels will provide us with a complete evaluation of the properties of the heart in three-dimensional space, which will directly translate to increased accuracy for evaluation of the CRT patients.
3D Wall Motion Tracking
Three-dimensional wall motion tracking, a new development in ultrasound technology, has the potential to revolutionize the way patients are evaluated for pacemakers. It allows us, for the first time, to see regional and global events of mechanical and electrical events in one cardiac cycle. It also provides quantitative information about myocardial contraction, displaying a complete picture of the heart and its motion in a three-dimensional aspect.
Since the motion of the heart is highly complex, many parameters are possible only by 3D wall motion tracking, which include longitudinal, radial, circumferential and transverse strain. With these calculations, the true motion of the heart can be tracked to provide a comprehensive analysis of left ventricular function and timing. This 3D information is crucial for a comprehensive diagnosis of global and regional cardiac function.
Quantitative wall motion tracking data, provided by 3D wall motion tracking, takes the subjectivity out of diagnosis by enabling us to detect wall motion abnormalities and timing events not visible to the naked eye. Now we can see not only a 3D visual depiction of the heart, but also graphical information showing the timing and movement of the heart’s walls. This ability to see the wall motion abnormalities in visual and graphical data from 3D wall motion tracking shows promise in mapping the site of latest activation causing the dyssynchrony. This is not achievable by 2D imaging.
Three-dimensional wall motion tracking is capable of displaying a 3D image quantifying LV function, which is also critical in evaluating patients for CRT. LV volume and ejection fraction, which are important predictors for CRT, are also calculated from the 3D data in a way that is superior to 2D imaging. LV function is exceedingly complex and 3D wall motion tracking helps give a more complete evaluation of viable tissue. Wall motion tracking also detects myocardial motion in all three dimensions and real-time motion data is produced. This data allows for the assessment of LV function and relations between segments such as displaying twist and torsion. These parameters give us a more complete and powerful assessment of the heart function. This can provide information that can determine where the pacemaker lead wire will have the optimal location, or even if a patient is going to respond to CRT. Thus, 3D wall motion tracking shows promise in optimizing device placement and reducing nonresponders.
Furthermore, 3D wall motion tracking can be very useful to demonstrate the patient’s response to CRT by showing the degree of improvements that result from CRT and quantify the degree of resynchronization. This can be reassuring to the patient and clinician caring for the patient as they have achieved a favorable resynchronization result. The ability of 3D wall motion tracking to document this response is truly remarkable. Additionally, physicians can use this new data to evaluate and adjust pacemaker settings after implantation to maximize pacemaker efficiency and its effects on cardiac function.
3D Wall Motion Tracking is Changing Cardiac Echo
Our group has had the opportunity to apply this new technology to the evaluation of approximately 55 patients before CRT. We found the 3D wall motion tracking to provide insight that was not possible before, and the ability to image and display the heart in this new way exceeded our expectations. We are very excited about the possibility to improve our capability to evaluate patients who are candidates for CRT. We believe that 3D wall motion tracking has the ability to capture unique and superior quantitative data that can translate into improvements in the care of heart failure patients who are being treated with CRT.
References:
1. Abraham W. T., Fisher W. G., Smith A. L., et al., “MIRACLE Study Group. Multicenter InSync Randomized Clinical Evaluation. Cardiac resynchronization in chronic heart failure.” New England Journal of Medicine, 2002;346: 1845–53.
2. Adrienne Heerey, Michael Lauer, Firas AlSolaiman, Jennifer Czerr and Karen James. Original Research Article. “Cost Effectiveness of Biventricular Pacemakers in Heart Failure Patients.” American Journal of Cardiovascular Drugs 2006.


 October 09, 2025
October 09, 2025