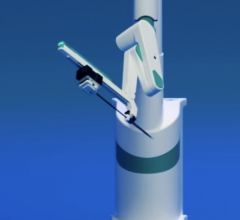
The RP-7 by InTouch Health allows doctors to interact with patients and view charts and monitors remotely.
The healthcare industry has increasingly integrated the use of robots into many areas of medicine. In intensive care units (ICUs) and operating rooms (ORs), doctors are working with robots hand-in-hand— literally. From allowing doctors to see patients anytime from any location, to helping perform minimally invasive surgeries, as well as delivering medications and supplies autonomously, medical robots are becoming a way of life for hospitals worldwide.
24/7 care
ICUs at dozens of hospitals around the country have added new staff members since 2005 in the form of nearly 6-foot tall remote-controlled robots. The Remote Presence Robot System (known as the RP-7) gives doctors the ability to monitor and communicate with patients when physically visiting the patient’s room is not possible, such as during after-hours and on weekends.
The RP-7 is equipped with a large two-way monitor video screen that serves as its face. This monitor allows doctors and patients to see, hear and speak with each other as if they were in the same room. Using a computer and joystick from a remote location — such as a home or office — doctors can guide the RP-7 to a patient’s bedside to communicate with patients and nurses, review medical charts and monitors and determine the appropriate care. Made by InTouch Health, the RP-7 travels up to 2 mph and uses infrared warning sensors to prevent from bumping into people, walls and other obstructions.
Doctors can control the robot’s camera and zoom in to take a closer look at a patient or monitor. The RP-7s are also equipped with digital video cameras, microphones, wireless communications, a printer, stethoscopes and other instruments.
The ability to see patients, communicate with nursing staff and visit the bedside at any time is especially helpful for doctors working in the ICU. For Michael Nelson, M.D., a critical care and pulmonary physician at Shawnee Mission Medical Center in Shawnee Mission, KS, using the RP-7 and its predecessor, the RP-6, has enabled him to increase time caring for patients while relieving some of the inherent stress associated with being on call 24 hours a day to the ICU for a week at a time.
“[Using the robot keeps] me from getting phone calls all night,” Dr. Nelson said. “As a general rule, my practice was to go home around nine or 10 o’clock, call up the ICU, put out as many fires as I could and try to go to bed. Now I drive the RP-7 around… I interact with the patients, I interact with the family and they really like that. It has decreased my calls significantly, which makes me more user-friendly in the morning when the next day comes around and I have to see patients.”
Dr. Nelson estimates using the RP-7 saves him one to three hours a night in traveling to and from the hospital. H. Neal Reynolds, M.D., an internal and critical care physician at Don Secours Hospital of Baltimore, has had a similar experience to Dr. Nelson, estimating he receives 50-75 percent less pages since utilizing the robot.
Dr. Reynolds points out that with the RP-7, it becomes easier to plan nighttime care for ICU patients with nurses and deliver pre-emptive treatments.
“The nurses and I now plan the next six to eight hours,” Dr. Reynolds said. “‘If A happens, here is what I want you to do. If B happens, here’s what to do.’”
The mobile robots may provide potentially life-saving service to smaller ICUs that don’t always have specialists on the premises by allowing intensivists from remote locations to quickly assess a patient’s condition and give the appropriate treatments. A 2002 Johns Hopkins University study reported only 37 percent of ICU patients are treated by an intensivist. There are hospitals in Michigan and California that have placed RP-7s in remote hospitals to allow for intensivists to treat patients. Dr. Nelson indicated his hospital might eventually set up similar agreements with rural Kansas hospitals.
“With the scarcity of critical care resources, a lot of the smaller towns in Kansas do not have a pulmonologist or critical care physician,” said Dr. Nelson. “If I stationed a robot that I had access to in a smaller community hospital that would not otherwise have access to a critical care physician, then the hospital’s medical care, we hope, would be improved.”
So far, patients seem to be pleased with the extra interaction with doctors via the robot.
“The patient acceptance has been remarkable,” said Dr. Reynolds.
Doctors have found few limitations with the RP-7. However, one potential challenge is since the RP-7 is connected to the doctor’s terminal via a wireless network. Occasionally if the network is busy, a moment may occur where the doctor may have difficulty hearing the patient or nurse speak.
Robots and minimally invasive surgery
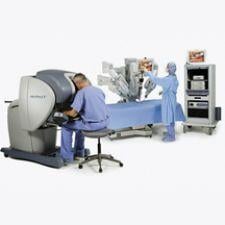
While the RP-7 makes it possible for doctors to help treat patients in other parts of the country, another medical robot might eventually allow surgeons to operate on patients remotely. The da Vinci System has changed the face of minimally invasive surgeries, according to multiple surgeons who spoke with Acuity Care Technology. Essentially, the system allows surgeons to see and access parts of the body using “robot” arms, yielding a more-precise surgery and decreasing a patient’s healing time.
The da Vinci System consists of two main components: the surgeon console and the patient-side cart. Seated at the surgeon console, which is located a few feet away from the operating table, the surgeon views a 3D image of the surgical field. The viewing field is up to 15 times the magnification of the naked eye. Just below the field screen, the surgeon’s fingers grasp the master controls inside the console. Next to the patient sits the patient-side cart. From the cart, supporting surgical staff insert two or three instrument arms and one endoscope arm into the body through 1-2 centimeter incisions. These arms perform the surgery by precisely mimicking the surgeon’s movements from the console in real-time.
Since the instrument arms were designed with seven degrees of motion, they mimic and surpass the dexterity of the human hand and wrist. Each instrument has a specific surgical purpose such as clamping, suturing, dissection and tissue manipulation.
The da Vinci has been used for heart and prostate surgeries, hysterectomies and other procedures according to da Vinci manufacturer Intuitive Surgical. Surgeons worldwide are continuously developing and refining surgeries using the system.
“Prostatectomy is the signature case of the da Vinci robot,” said James C. Jensen, M.D., surgeon with The Edwards Comprehensive Cancer Center in Huntington, WV, who has performed nearly 500 prostatectomies. “We’re expanding the horizon of what we do robotically for every potential operation for urology.”
Myriam J. Curet, M.D., FACS, professor of surgery and director of minimally invasive surgery at Stanford Hospitals and Clinics, has developed with her students a robotic gastric bypass surgery. Dr. Curet believes using the da Vinci for minimally invasive surgeries provides many advantages over laparoscopic procedures.
“In my practice, laparoscopic gastric bypass in the hardest thing that we do,” said Dr. Curet. “It required suturing, and laparoscopic suturing is really difficult to do. Unlike open surgery, when you do it laparoscopically, you only have 2D visualization, you are working very far away from your instrument tips and you’re instruments move differently than for open surgery. What the robot does is offset those limitations. Now, you have 3D visualization. You’re operating right at your fingertips and you’re instrument tips move in the direction you’re hand moves and you have the wristed instruments, so it’s like open surgery.”
Dr. Curet also noted that robotic gastric bypass surgeries take 30-40 minutes less time than a laparoscopic procedure and leaves the surgeon physically feeling better and more able to perform more surgeries a day.
According to surgeons who have utilized da Vinci, patients have experienced significantly less post-operative pain, less blood loss, fewer complications, shorter hospital stays and faster returns to daily activities.
The learning curve can be steep. While surgeons who spoke with Acuity Care Technology said learning the basics of operating the da Vinci isn’t a major challenge, but developing specific surgeries the da Vinic hasn’t performed can take time.
Dr. Jensen said the first robotic prostatectomies he performed took several hours longer than conventional prostatectomies. He notes that while it took 150 robotic prostatectomies for him to complete the procedure in the same time as a conventional prostatectomy, he now performs the surgery in 40 percent less time than ever before.
Delivering supplies
Another robot gaining traction in hospitals is utilized for logistical purposes. The TUG automated courier system is designed to deliver medications and various supplies to departments around a hospital with minimal supervision. The TUG, which bears resemblance to the base of a standard vacuum, sits low to the ground. Various carts filled with up to 500 pounds of supplies may be attached on top of the TUG for delivery.
Kimberly Ellis Krakowski, RN BSN, a pharmacy nurse liaison clinical specialist with Washington Hospital Center in Washington D.C., helped coordinate the integration of the TUG into the hospital’s workflow in 2007 in an effort to use staff more efficiently. Currently, three TUG units deliver medications from the central pharmacy, as well as other medical materials, to specific nursing units and other designated areas.
Krakowski indicated the hospital plans to expand the TUG’s role to serve nearly every nursing unit, including high-acuity departments, later this year with the addition of four TUG units.
So far, Krakowski has found the TUG to be a reliable tool in decreasing the burden of manually distributing supplies across the hospital. She cited a 14 percent increase in the nursing staff’s satisfaction level on whether medications are available to them when they need it, a question Krakowski asked nurses as a part of a survey conducted before and after TUG implementation. Those results are similar to a survey conducted at The University of Maryland Medical Center’s R. Adam’s Crowley Shock Trauma Unit. According to TUG manufacturer Aethon, the TUG decreased the cycle time for first doses delivered to the trauma unit by 44 minutes and increased nursing satisfaction by 23 percent.
Krakowski has been impressed with the TUG’s reliability and said there have been very few problems with the robot traveling around the hospital without unescorted. Since Washington uses several automated fire-safety doors throughout the building, the TUG sends an electronic signal to those doors to open. For doors that aren’t automated, the TUG emits an electronic noise, sounding similar to a doorbell, alerting staff on the other side to open them. The robot can also enter and exit an elevator independently, said Krakowski.
One of the only limitations, according to Krakowski, is that the TUG doesn’t work best traveling to locations with tight corners. Another challenge may arise if the TUG is traveling down a path, which becomes obstructed by a large object or people, however the robot typically handles obstructions well, Krakowski said.
“The technology is smart enough to where it can speak, and if it meets a road block it will say ‘waiting to proceed’ and it will repeat itself until the obstacle has moved or it will navigate around it,” Krakowski said. “If a trip normally took five minutes down a hallway, if it were to approach a group of people having a conversation, it might take it six minutes.”



 January 27, 2026
January 27, 2026