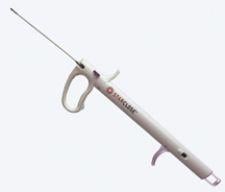
The StarClose from Abbott Vascular is the first extravascular clip-based closure device.
In the cardiac cath lab, success is measured in part by how quickly the patient can ambulate and go home.
With the volume of diagnostic procedures on the rise, hospitals need to get patients through the lab and out the door in a timely manner, according to Paul Buckman, president of St. Jude Medical’s cardiology division. Vascular closure devices are key because, in addition to being more convenient for staff and comfortable for the patient, they allow patients to ambulate sooner than standard manual compression.
Buckman adds that due to advancements in technology and medical care, many formerly invasive procedures have migrated to less invasive or percutaneous options. As a result, manufacturers are responding with newer, more refined vascular closure alternatives for both diagnostic and interventional procedures.
“It has become a very competitive market and the ongoing need and search for the ideal closure device has inspired new methods and closure platforms,” explained Nancy Werfel, senior product manager with Datascope Interventional. And because no single device is advocated for all situations, she points out, there will always be a need for a variety of effective devices.
Out with the Old
When deployment of bare metal stents in the U.S. first began in the mid- 1990s, aggressive anticoagulation was being used to prevent stent thrombosis, which led to a marked increase in vascular access complications, particularly at the femoral artery, explains Tony M. Chou, M.D., general manager, Vessel Closure Technologies, Abbott Vascular Devices.
“That spawned the need for vascular closure devices to provide a secure closure and improve patient safety,” he said.
Over the years the drivers for vascular closure methods have evolved and, to a large degree, now center on patient comfort and decreased time to ambulation. Noninvasive methods, most commonly used with diagnostic procedures, provide topical hemostasis at the puncture site, whereas invasive devices penetrate the skin to close the wound — often with a plug or suture — within or on top of the tissue tract.
Today’s closure devices are easier to use, more effective and reliable, and not surprisingly, very popular with physicians and cath lab staff.
In fact, in the cardiac cath lab at University Hospital, San Antonio, TX, the teaching hospital for the University of Texas Health Science Center, closure devices are preferred almost exclusively over manual compression.
The hospital’s 22-member cath lab staff performs roughly 210 procedures monthly, serving patients from 23 Texas counties. The lab was one of the original clinical investigation sites for Abbott Vascular’s StarClose device; however, its continued use of the product is based on more practical considerations.
“We like the StarClose because (1.) it is easy to use and (2.) it is predictable,” said Steven Bailey, M.D., director of the Cardiac Cath Lab and distinguished professor of Cardiovascular Research. “In our environment we have a lot of cardiology fellows; we want them to have a device that we are certain they can use and use correctly,” he added.
The StarClose introduces — with a series of four clicks — a tiny metal clip onto the surface of the femoral artery to securely close the artery in a matter of seconds. Since its release, it has become University Hospital cath lab’s favored closure modality for diagnostic and 6Fr interventional procedures.
Many cath lab patients at the San Antonio hospital are repeat visitors — following an initial catheterization they return for one or more interventions. According to Dr. Bailey, StarClose is ideal for repeat procedures because it reduces inflammation and improves healing. In addition, an artery that was originally sealed with the StarClose is easy to repuncture, a benefit for both the physician and the patient.
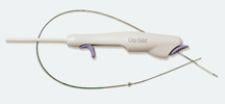
Another facility enjoying the latest in cutting-edge technology is Palmetto Baptist Hospital in Easley, S.C. Since April the Palmetto cath lab has been using Datascope’s newest percutaneous arterial closure device, the On-Site.
Deployed by a single operator, the On-Site precisely delivers collagen on top of the arteriotomy, where it rapidly expands to form a mechanical barrier. The primary benefit, according to the company, is that the device is extravascular and doesn’t require intra-arterial components, which can potentially cause trauma to the artery.
Brian Finley, RT, director of Cardiopulmonary Services at Palmetto, agrees.
“The No. 1 benefit of the On-Site is that there is no way the collagen can get inside the artery,” he said. “We are very pleased with the device; it is user-friendly, safe for the patients and yields good results. Patients are up and ambulating in about two hours,” Finley added.
Palmetto performs approximately 860 cath lab procedures per year and plans to continue using the On-Site for both diagnostic catheterizations and interventions with 5, 6 and 7Fr sheath sizes, regardless of clot time, according to Finley.
When completing a diagnostic procedure at Somerset Medical Center in Somerville, NJ, members of the cath lab team, including Kenneth S. Sternberg, D.O., director of Interventional Cardiology, reach for the Angio-Seal closure device from St. Jude Medical.
Now in its seventh generation, the Angio-Seal is an intravascular device that “sandwiches” the arteriotomy between a bio-absorbable anchor and collagen sponge. Because a mechanical seal is created, hemostasis does not depend on clot formation.
At Robert Wood Johnson University Hospital, the large tertiary referral center where Dr. Sternberg performs his interventional procedures — and where over 4,000 interventions are performed a year — the majority of the procedures are closed using the Angio-Seal.
“The reason we like the Angio-Seal better than some of the other devices is that it gives us a much higher comfort level of closure because of the little foot inside the artery and the collagen plug that sits on top of the artery,” Dr. Sternberg explained.
Over the last three to four years, Dr. Sternberg admits to using other closure devices, many of which have since come and gone in his labs. During that time, the Angio-Seal has become their top choice for vascular closure.
The Angio-Seal is also favored by Dr. Sternberg for another reason. About a year and a half ago, he began performing same-day angioplasties in highly selected cases. He attributes the success of these procedures to the combined use of anticoagulation with the drug Angiomax and new closure devices, specifically, the Angio-Seal. As a result, rather than staying overnight in the hospital, patients are returning home after six hours.
On Top of the Situation
Given the variety and increasing number of procedures being performed, it’s clear that when it comes to vascular closure, one size does not fit all.
Just ask Marcie Gruchevsky, RN, of the Florida Cath Lab LLC in Orlando.
“We are a freestanding cath lab that uses rather small sheaths, primarily 4 or 5Fr, to perform our diagnostic cardiac and peripheral procedures,” Gruchevsky said. As a result, she explains, use of invasive devices that are more appropriate for sealing access sites created by larger sheaths is simply not necessary.
The Florida Cath Lab consists of six beds and performs between 12 and 14 cases per day. The facility’s method of choice for hemostasis management is manual digital pressure performed in conjunction with a topical hemostat. For nearly three years Gruchevsky and her colleagues have been using the D-Stat Dry thrombin-coated hemostatic bandage from Vascular Solutions with great success.
“My primary goal is patient satisfaction,” Gruchevsky explained. “With the D-Stat Dry, blood starts to clot instantly, and so we only have to hold from five to seven minutes, which makes our patients incredibly happy.”
Another patient-pleasing aspect of the D-Stat Dry is that the head of the bed can be elevated to 30 degrees immediately following a procedure. With manual compression only, staff would have to hold for 15 to 20 minutes to allow the clotting cascade to begin, and the patient would need to lie completely flat for at least one hour. Providing there are no other concerns, such as blood pressure, hematoma or bleeding, patients can now ambulate completely in an hour and a half and go home, according to Gruchevsky.
Cath Lab of the Future
Despite their popularity, a wide variety of opinions on vascular closure device use still exists. Closure devices are essentially an option in the cath lab, reminds Chou, that physicians — for a number of reasons — may or may not choose to employ.
“Manual compression is still very popular,” Chou explained. Even when using a mechanical device, some physicians like to be able to control any residual bleeding with extra compression.
But industry experts, including Chou, agree that acceptance of vascular closure devices is steadily rising, as evidenced by the more than four million procedures closed annually with a mechanical closure device.
“While current practices are about evenly divided between manual compression and [vascular closure] devices, the future trend is toward increasing use of some type of closure device,” Werfel said.
“In the cath lab of the future you’ll see the ability of these devices to cover all ranges of patient anatomy and disease,” added Buckman. “I would like to think at some point that every patient would be a candidate for a closure device.”