
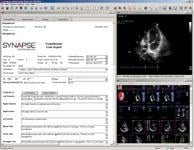
Third-party cardio PACS vendors often partner with other vendors to increase interoperability. An example: Fujifilms Synapse Cardiovascular 4.0.5, which integrates with both GE Healthcares EchoPAC and Philips QLab cardiac ultrasound applications.
Healthcare IT vendors offer a variety of cardiovascular information systems (CVIS), picture archiving and communications systems (PACS), imaging and diagnostic hardware they say will integrate into a seamless electronic medical record. However, end-users still complain this level of interoperability does not exist. Diagnostic & Interventional Cardiology offers the following advice to buyers so they are better prepared to make purchasing decisions.
How Data is Shared
The two most common standardized data formats used in healthcare IT are HL7 (Hospital Health Level Seven International) for data such as measurements, reports, patient monitoring device numeric values, etc. and digital imaging and communications in medicine (DICOM) for medical images, such as angiography, echo, CT, MRI and nuclear.
HL7 is actually a nonprofit standards developing organization that provides a comprehensive framework and related standards for the exchange, integration, sharing and retrieval of electronic health information that supports clinical practice. While HL7 has more than 500 corporate members, representing more than 90 percent of the healthcare information systems vendors, the way each vendor programs or processes specific data fields varies. While the raw HL7 data will transfer easily between devices and systems, data that is modified using proprietary software features or fields does not always transfer. Each vendor’s software will slice and dice information differently, so the modifications made in one system may not transfer correctly into another from a different vendor. A layman’s example of this is similar to the differences in how text (bolding, underlining, etc.) appears (or doesn’t appear) when transferring data between a Mac and a PC.
The National Electrical Manufacturers Association (NEMA) developed the DICOM standard. Raw DICOM images usually transfer without much trouble between imaging devices and various software, PACS and reports. However, most imaging systems come with their own proprietary software specific to the manufacturer of the device. Images modified or manipulated with this software often causes interoperability problems when transferred to PACS, advanced visualization or reporting software made by other manufacturers. For this reason third-party software is frequently used to manipulate, report and store images.
Proprietary vs. Third-Party Systems
Interface issues with DICOM and HL7 generally do not matter if a hospital uses a single vendor’s PACS, reporting systems, patient monitoring devices and various modality imaging systems. Vendors such as Siemens, Philips and GE all test their devices and software for interoperability.
However, many hospitals use best-of-breed devices or have a variety of legacy systems from multiple manufacturers. In this situation, many hospitals opt for third-party, vendor-neutral software systems for their PACS, reporting and advanced visualization. These systems take the raw HL7 and DICOM data and process it using open IT standards so the information will easily flow through various electronic medical records (EMR), hospital information systems (HIS) and between departments.
In most cases, third-party cardiovascular PACS vendors partner with other open-standards, third-party software vendors for components like advanced visualization (such as TeraRecon, Vital Images, TomTec and Emery Toolbox) or electrocardiogram (ECG) storage and reporting components.
Some vendors are working to provide better connectivity between their systems and those of other vendors. At RSNA 2010 in December, GE Healthcare introduced its E-Health Imaging Exchange, which allows images to be exchanged between disparate healthcare providers. The system uses XDS format that enables cross-enterprise image sharing. Many vendors now offer Web-based solutions to share images with referring physicians.
Third-party, vendor-neutral cardiac PACS vendors include McKesson, Infinitt, Fujifilm, Carestream, Agfa, ScImage, Merge, Digisonics, Lumedex, Thinking Systems and DR Systems.
Waveforms, ECGs, Hemodynamics
Saving ECG and hemodynamic waveforms presents a problem with most PACS. “There is no industry standard for waveforms,” said Les Campbell, product manager with ScImage. “Radiology does very well in this space with DICOM worklists, but cardiology, with all its waveforms, does not do so well.”
Various vendors use different formats, including HL7 and their own proprietary formats. Campbell said the only DICOM-based ECG system on the market is from Mortara. Some vendors, such as Philips, use an extensible markup language (XML) format to transfer their ECG waveforms into PACS systems. Agfa converts old ECGs into an optical character recognition (OCR) format, which can then be translated into an HL7 format. Most Holter monitoring systems and stress test systems data can be saved as PDFs.
Several PACS and CVIS vendors, including ScImage, standardize on PDFs to collect sample waveforms to include in patient records. However, Campbell said the Adobe program used to create PDFs adds a border and squeezes the image, making it difficult to discern some details, such as tiny P-waves. ScImage’s Web-based PicomECG software modifies the PDFs to prevent the border from appearing and squeezing the image. Due to its vendor-neutrality, PicomECG is used as a third-party software by other vendors, including Siemens cardiovascular IT solutions.
McKesson converts ECGs into XML files, since DICOM can be converted into XML. However, XML files cannot be converted into DICOM. McKesson’s CVIS also saves waveforms as a PDF so they can be uploaded into a patient’s EMR.
Hemodynamic waveforms present a similar problem, as some vendors still use propriety data formats. Merge Healthcare deals with this issue by converting the hemo system data into an XML file so it can be transferred into the Merge EMR.
Failed Integrations, Seeking New Solutions
When a CVIS or PACS fails to integrate with critical parts of the electronic medical record, hospitals will look for a replacement. Elmhurst Memorial Healthcare in Elmhurst, Ill., is building a new cath lab and is rewiring its cardiac image and information systems due to ongoing connectivity issues with its existing system. The hospital plans to switch to the Merge Heartsuite CVIS in 2011 in hopes of correcting numerous connectivity issues that interrupt workflow.
Renee Bianchetta, RN, quality analyst and project manager for the CVIS conversion at Elmhurst Memorial Healthcare, said its current CVIS cannot integrate with the cath lab’s hemodynamics system due to proprietary coding. As a result, she said hemodynamic data must be manually entered into the CVIS.
The system also does not integrate well with the hospital’s EMR system. Bianchetta said the EMR strips out coding for text styles like bolding and underlining used to differentiate sections of reports, making the reports very difficult to read. In addition, American College of Cardiology (ACC) and other registry data must be transferred and entered manually.
“Organizations are challenged with trying to find how to streamline this process so you don’t have a lot of full-time employees manually entering data,” Bianchetta said.
She said another point CVIS buyers should consider is if the CVIS they plan to buy includes all the reporting tools they need. While CVIS vendors all offer reports for the cath lab and imaging, some do not have modules for electrophysiology (EP) or interventional radiology (IR), which are often rolled into combined cath lab operations, such as at Elmhurst Hospital. If other vendor’s PACS or reporting systems were added to accommodate EP and IR, Bianchetta said it would create additional compatibility issues.
Web- and Cloud-Based Systems
Instead of each computer in a department, hospital or healthcare system needing to be hardwired through network connections, the big trend in health IT is to eliminate dedicated wiring and connect users to software and patient records through the Internet. Cloud computing also allows health systems to maintain their data, images and computer processing power off-site, but easily accessible through an Internet connection using thin-client computers.
“Doctors want access at multiple locations and they don’t want to maintain or license thick clients,” said Lisa Braunreuther, global business manager, Cardiology IT, Agfa Healthcare. “Web-based applications offer better accessibility and lower maintenance costs.”
She said Web-based systems also help with consolidation of practices and health systems by providing an easy way to connect various offices and facilities. These systems also allow a lower ownership cost and greater functionality and flexibility than a hard-wired network.
Cloud-based computing takes the large amount of computer processing needed to run some programs and places it on a remote server. Smaller, thin-client computers, including iPads, can then access that computing power and vast amount of file data via the Internet, rather than being networked or needing large processing or storage capability.


 January 15, 2026
January 15, 2026 









