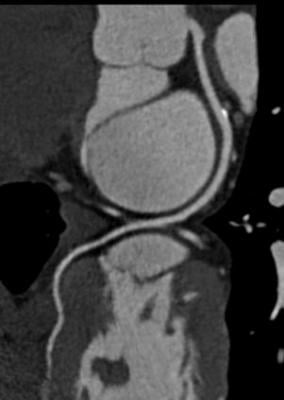
In an era when increasing efficiency, reducing costs and facing an increasing influx in the number of patients is of upmost importance, hospital emergency departments (ED) are looking for more effective ways to triage patients. A large number of ED visits are for chest pain evaluation, and many hospitals are adopting computed tomography angiography (CTA) as a primary test to quickly rule-out coronary disease, which is the case in the majority of these patient presentations.
The current standard of care for patients presenting with chest pain in most EDs is to take a detailed patient history, conduct a physical exam and then perform and electrocardiogram (ECG) and troponin test. Troponin testing actually involves two tests done four to six hours apart, which adds a considerable amount of time to a patient’s stay in the ED.
CTA exams can be used in addition to, or to replace, the standard progression of chest pain evaluations, since the rule-out results of a CTA will be known much faster than waiting for a second troponin test.
“You are not going to harm the patient by sending them for a CT,” Gilbert Raff, M.D., director, advanced cardiovascular imaging, Beaumont Hospital, Royal Oak, Mich. “Chest pain may have several causal reasons that can be determined on a CT.”
In addition, Raff said a CT offers a lot more ancillary information beyond the coronaries. He said the imaging also shows if the patient has pneumonia or can be used for the triple-rule out of coronary disease, pulmonary embolism or an aortic dissection.
Growing Trend of CTA in the ED
Raff said there has been a big increase in interest in CTA in the ED since the positive results were published from three key trials, including the CT-STAT, ROMICAT II and ACRIN PA.[1,2,3] “In each case the trials were comparing CT to the standard of care,” Raff said.
In the CT STAT trial, Raff said CTA was compared to ECG plus a nuclear myocardial perfusion exam to look at speed to diagnosis, costs in the ED and patient safety. The data showed no difference in safety and that CT patients were discharged much faster than the standard of care, which translates into cost savings, Raff explained. One point of interest from the study was that 30 percent of patients received no imaging study, but the patients sent for CTA evaluation were actually discharged faster.
However, Raff said the study also found CTAs showing significant blockages usually translated into sending more patients to the cath lab than the standard of care arm of the study. Since the cath lab increases costs per patients, the question was raised if CTA may drive up additional costs.
“The cath lab rate is likely higher than it needs to be,” Raff said. “Modern evidence shows you do not need to catheterize all patients with chest pain. Patients don’t need a cath unless the blockages are flow limiting. But, if we designate a lesion as 50 percent blocked, it does not mean it is flow limiting.“
This leads to frequent misinterpretations on CTAs, so he feels guidelines need to be established to encourage the person reading the study to call and discuss the findings with ER physicians. He said a patient with a 50-70 percent blockage likely needs some sort of follow up, but patients with a blockage of more than 70 percent need to be admitted.
"Most patients don’t have actionable lesions,” Raff explained. “Only about 14 percent of patients need further testing after a CT.”
Patient Selection is Key
According to the data from the three key trials examining CTA’s use for chest pain evaluation, CT is very good at ruling out cardiovascular disease, but it is not as clear at determining impact of the disease in patients who have coronary atherosclerosis. For this reason, CTA is best used in ED for patients whose risk of coronary disease is unknown or those unlikely to have it.
“One of the issues with CT use in the ED is the over selection of patients,” Raff said. “We are not selecting patients with known prior coronary artery disease. What you want are the patients with no prior history of heart disease.”
He said CTA is best for patients with no history of heart disease. A CTA helps eliminate ECG and other tests, and will speed patient triage and discharge in the majority of cases.
“The vast majority of patients with chest pain do not have any serious problem, and that is what we want to know by using a CT exam,” Raff explained.
He said a Michigan registry of about 50,000 patients accumulated data on how CTA was used for chest pain evaluations. Raff suspected CT would just be added on as another layered test, but was surprised to find that CT was used to eliminate the need for ECG testing by ruling out heart problems.
There currently are no generally accepted CTA guidelines for patient selection in the ED, but that will change in early 2014. The Society of Cardiovascular Computed Tomography (SCCT) is currently in process of preparing guidelines for the use of CT in the ED, and plans to publish them in early 2014. Raff is the co-chair of the writing group for the new ED guidelines.
Lowering Length of State, Costs
Beaumont Hospital, Royal Oak, Mich., began CTA screenings of chest pain patients in the ED about five years ago. At the time of implementation, the average length of stay for these patients was about 22 hours, Raff said.
About 50 percent of patients presenting to the ED have known disease, so that cuts about half of the patients from CT scans. Of the other 50 percent, only about 20 percent are sent for a CTA, and most of these patients are discharged within four hours, Raff said. He explained the hospital receives about 500 chest pain patients a month and has about 155,000 total ED cases per year.
“They can only observe 20 patients at a time in the observation unit, so you can see how fast their beds get filled up,” Raff said. “You also have only so long to diagnose a patient or you need to admit them. We know CT has increased the discharge rate from the ED and it significantly cuts the length of stay.”
“There are more than 5 million chest pain patients evaluated in the U.S. each year, so when you discuss 20 percent of these patients, it is a lot of patients,” Raff said.[4]
He said CTA has could offer a significant cost and time savings in the long haul for hospitals.
CT Scanner Technology
Raff said standard 64-slice CT systems are more than adequate for CTA exams. While the higher cost might be a limiting factor when considering higher-slice systems, there are some advantages of using 256, 320 or 640 slice scanners.
“Temporal resolution is faster with more slices, so it saves time and removes motion artifacts.” Raff said. “The higher slice systems are also better for patients with higher heart rates.”
North Shore University Hospital in Manhasset, N.Y., installed a 640-slice Aquilion One Vision CT system in April 2013 and uses it as a dedicated cardiac scanner. The scanner is also used to evaluate chest pain patients from the ED. The new system replaced a 64-slice scanner. The 640-slice system was chosen because of its faster scan speed, ability to greatly reduce radiation dose, and due to its 16 cm scanning area, elimination of motion and stitching artifacts by capturing a cardiac study in one heart beat and without stitching multiple images, said Biana Trost, M.D., director of cardiac CT of the department of cardiology
“The major advantages of this 640-slice scanner is its very fast scan speed and excellent 3-D imaging delivered at a very low dose, which are ideal for use in the ED,” she explained. “CT has 99 percent accuracy in its negative predictive value in determining if a patient has serious coronary disease, and that is better than any other imaging modality I can think of. To evaluate if a patient does or does not have coronary disease, CT is definitely the way to go.”
Trost compared the radiation dose from all cardiac CT scans performed in March with the old 64-slice scanner and compared them to the month of scans on the new scanner the month after implementation of the 640-slice scanner. She found there was a major 78 percent reduction in dose. She attributes this to the larger scan area, use of prospective gating and eliminating the image overlap required for helical scans on the 64-slice system. In addition, since motion and stitching artifacts were basically eliminated with the new system, there were fewer repeat exams required. Trost said the average dose for a CTA scan is now about 3 mSv. For triple-rule out studies that require a larger scanning area, the average dose is about 6-8 mSv.
North Shore assesses the use of CT on a case by case basis. "Although we don't have a strict criteria for excluding patients for CTA, we only did a few patients who presented to the ED with chest pain and had a history of a prior stent. Their troponin was negative and ECG was normal. The ED attending usually discusses it with us prior to ordering the scan on a patient like that."
“I think it should be the first choice test for evaluating chest pain. It helps eliminate other tests downstream and it helps us discharge patients from the ED more quickly,” Trost said.
Reading CTAs
Raff said training physicians to read CTA scans is not difficult, but it is important to read a lot of cases to quickly pick out which ones are real emergencies. He suggests the need to read at least 300 cases per year to hone the emergency response skills needed.
“The real barrier is the experience of the reader and the ability of the hospital to designate staff to properly prepare patients for a CTA exam,” Raff explained.
Another issue is the need for hospitals to develop a protocol for patient selection. Raff said the selection systems needs to be sophisticated, and there is a need for a STAT responder to be able to read these exams quickly and accurately. If not, the program will not be successful, he said.
Driving Down Caths Via Virtual FFR
A promising new technology on the horizon is the used of CTA to accurately and noninvasively measure fractional flow reserve (FFR). Currently, FFR is only measurable via invasive catheters inserted into the patient in the cath lab, and guided to lesions in question under angiography. The CT-FFR system uses complex supercomputing software that analyzes the fluid dynamics of iodine contrast in the blood as it flows past coronary lesions. In addition to the lesion in question, the technology also offers overall FFR scores for segments of vessels with long diffuse disease and the total FFR per region of the heart, including all blockages and their cumulative impact on ischemia.
Raff said the virtual FFR technology offered by HeartFlow Inc. is exciting, but its current form being tested in the DeFACTO Trial is not practical. The issues include the expense and the need to send the CT datasets to the vendor in California and then wait about 24 hours before the computer can complete the analysis. The time required is the biggest barrier to wide adoption, but as computing speeds continue to become faster, this technology will become more viable.
“The data is too new, but I am pretty optimistic that in the next few years this can be used,” Raff said.
References:
1. Goldstein, Chinnaiyan, Raff, et al. “CT-STAT (Coronary Computed Tomographic Angiography for Systematic Triage of Acute Chest Pain Patients to Treatment)”
J Am Coll Cardiol. 2011 Sep 27;58(14):1414-22. doi: 10.1016/j.jacc.2011.03.068.
2. Hoffmann, Truong, Schoenfeld, et al. “Coronary CT Angiography versus Standard Evaluation in Acute Chest Pain.” N Engl J Med 2012; 367:299-308July 26, 2012DOI: 10.1056/NEJMoa1201161 (ROMICAT II Trial)
3. Litt, Gatsonis, Snyder, et al “CT angiography for safe discharge of patients with possible acute coronary syndromes.” N Engl J Med. 2012 Apr 12;366(15):1393-403. Epub 2012 Mar 26. (ACRIN PA Trial)
4. F. Bhuiya, S. Pitts, L. McCaig. “Emergency Department Visits for Chest Pain and Abdominal Pain: United States, 1999-2008.” NCHS Data Brief Number 43, September 2010.