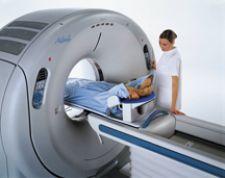
CIS utilizes Toshiba's Aquilion 64-Slice CT because of its speed, and it uses less radiation and contrast.
The only safe assumption to make about today’s current gold standard imaging modality used to identify and evaluate atheromatous plaque in the peripheral arteries is that there is not one gold standard. To locate and evaluate these plaques that cause peripheral vascular disease (PVD), physicians have multiple tried-and-true imaging tests at their disposal.
In keeping with the general trend of modern cardiology and radiology, invasive imaging techniques — though still useful and necessary in certain instances — have largely given way to noninvasive scans. Yet, even among the noninvasive modalities, it’s difficult to assert that one scan is totally superior to another.
And while certain modalities are popular, emerging modalities and techniques seem to have the potential to change the imaging of the peripheral arteries in the future.
What is the Gold Standard?
“Invasive angiography has a spatial resolution that the other [imaging] techniques can’t match practically,” said Eric Williamson, M.D., assistant professor of radiology at Mayo Medical School, Mayo Clinic, Rochester, MN. “You can argue that with MRI you can make the voxels as small as you want to, or intravascular ultrasounds where the spatial resolution is incredible. But, on a practical basis, there isn’t any other technique that can image the entire vascular tree with the spatial resolution of invasive angiography. I don’t ever see that failing to be the gold standard.”
However, according to Dr. Williamson, noninvasive computer tomography angiography (CTA) and magnetic resonance angiography (MRA) are now the preferred modalities for diagnosis. Dr. Williamson favors CTA, using CT systems by Siemens and GE Healthcare.
“[CT] represents a big paradigm shift over the past five years,” Dr. Williamson said. “CT angiography has essentially replaced catheter angiography as a first line imaging test of the diagnosis of peripheral vascular disease at our institution.”
CTA is the preferred modality at the Cardiovascular Institute of the South (CIS), a group of cardiovascular care centers in south Louisiana, according to Peter S. Fail, M.D., CT medical director for CIS. That is not to say that there aren’t inherent problems with the CT. Perhaps the CT’s biggest nemesis in producing clear images of peripheral arteries is presence of heavy calcium, according to the physicians who spoke with Diagnostic and Invasive Cardiology.
“As you get into the peripheral vascularature, they tend to be much more calcified than the coronaries,” Dr. Fail said. “It’s difficult to ascertain good luminal flow or is it just a completely occluded artery with calcium? That’s where it becomes difficult to really separate.”
Dr. Williamson is hopeful that newer CT systems, such as Siemens’ SOMATOM Definition with Dual Source technology, will one day be able to solve the calcification problem, though no CT system has solved the problem yet.
“[Dual Source technology] allows you to characterize plaque in a way we haven’t been able to do previously,” Dr. Williamson said. “That sounds really cool…that you can remove all the calcification and look at the artery underneath and differentiate soft plaque versus calcified plaque. Theoretically, this is extremely helpful, but we haven’t proven that its clinically important yet.”
There are other challenges with CT.
“One of the downsides of CT is it doesn’t give you hemodynamic information that you can get from an invasive angiography,” said Dr. Fail. “But, a lot of times if you are looking for clinical or subclinical disease, the CT is definitely superior.”
According to Christopher Kramer, M.D., professor of radiology and medicine, director of the Cardiovascular Imaging Center of the University of Virginia Health System, MRA is the gold standard for imaging the peripheral arteries.
“People have really moved to the noninvasive imaging for making a diagnosis,” Dr. Kramer said. “[Doctors] may only go to invasive angiography when an intervention is needed.”
“Generally, MRA is preferred. There’s some artifacts on CTA, there’s a lot of radiation and it uses nefrotoxic contrast material,” he added.
Dr. Kramer also prefers MRA because calcium is easier to identify and doesn’t interfere with imaging the peripheral arteries.
The doctors who spoke with Diagnostic and Invasive Cardiology concede that different institutions may favor the CTA or MRA over the other for a variety of reasons, not the least of which is a physician’s or institution’s preference.
“You can find a lot of proponents for both [CTA and MRA],” Dr. Fail said. “When you [examine the reasons] why they are a proponent of one modality or another, it might be because they are really good at what they do in that particular modality. I think realistically if you have someone who is a good MR person, they’re going to get fantastic images and great diagnosis with MR. If you have someone who is a good CT person, they are going to do the same.
“I don’t think there’s truly one benefit over the other. I think MR has got some hemodynamic issues or some flow issues that are maybe a little bit better than CT, but I think realistically, the time, expenditure, cost of the machine, etc., probably puts the PVD diagnosis into the CT ballpark.”
Challenges with Contrast
Both CT and MR have experienced problems using contrasting agents with certain patients. According to Dr. Williamson, referring physicians and radiologists have been leery of giving patients with renal insufficiencies iodine-based contrast used for the CTA, instead ordering an MRA for those patients. Dr. Fail roughly estimates that 5-7 percent of PVD patients don’t get a CTA because of a renal condition, although there are other factors involved in the decision.
For the MRA, using the contract Gadolinium has proved problematic.
There is strong evidence that Gadolinium has caused Nephrogenic Systemic Fibrosis (NSF) in patients with kidney failure, prompting the FDA to issue a warning in 2006. For patients needing an angiography for PVA who have stage four or five Chronic Kidney Disease (with creatinine clearance a less than 30 mL/min), CIS avoids using the MRA, said Dr. Kramer. He hopes that newer generations of MR will not require Gadolinium.
“[The number of patients affected] is not insignificant, that’s for sure,” Dr. Kramer said.
New Invasive Techniques
While noninvasive imaging seems to be the trend relating to PVD, there are new invasive technologies with both diagnostic and interventional applications, which may be available to U.S. doctors in the not-too-distant future.
One such technology is TopSpin Medical’s IntraVascular MRI (IVMRI). Recent clinical trials were performed to determine if IVMRI could better locate vulnerable plaques prior to plaque instability. While the trials were focused primarily on the coronary arteries, they did look at the peripheral arteries, specifically the superficial femoral artery (SFA), according to a clinical review of these trials published last year titled “Intravascular MRI for the Evaluation of Lipid-Rich Vulnerable Plaques in Coronary and Peripheral Vessels” by Robert Wilensky, M.D., and Jacob Schneiderman, M.D. Dr. Wilensky, director, experimental interventional cardiology, professor of medicine at the Hospital of the University of Pennsylvania, said the IVMRI may not yield the beautiful pictures like the MR, but it has yielded some “good results” on the presence of lipids within the arterial wall. Dr. Wilensky’s report noted that IVMIR analysis of atherosclerotic plaques is expected to produce a better understanding of the disease process and more appropriate therapy.
The IVMRI received European approval in 2006 and has submitted its application for FDA 510(k) clearance, according to the company.
Another potential modality is Volcano Corp.’s OCT imaging catheter, which uses optical coherence tomography (OCT), which is designed to enhance the diagnosis and treatment of coronary and peripheral vascular disease by providing high-resolution images in the 10-15 micron range. The first human procedure using the OCT imaging catheter was performed in May 2008 in The Netherlands.


 January 11, 2024
January 11, 2024