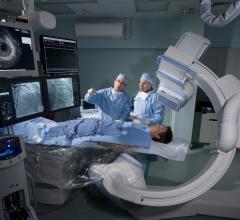
The GE Innova 3100 with FPD boasts up to 10 times the dynamic range of image intensifier-based systems.
When it comes to diagnosing disease, image is everything. It is difficult to treat what you can’t see. That’s especially true in the cardiac cath lab where cardiologists performing procedures ranging from simple diagnostic tests to more complex interventional maneuvers rely on imaging technology to guide their course. To ensure patients get the best treatment possible — and to remain competitive — cardiologists more and more are demanding state-of-art equipment in the cath lab.
One method of obtaining clearer images of complex vascular and cardiac anatomy is with flat panel digital angiography systems. Angiography systems have been a diagnostic mainstay in cardiac cath labs for over 50 years, playing a pivotal role in the diagnosis and treatment of heart and vascular diseases. The introduction of flat panel detectors (FPD) — replacing image intensifiers — for angiography has broadened digital imaging’s role in the cath lab. Now cardiologists can see, immediately and with greater clarity, the intricacies of the heart, the vascular system and how well they are functioning.
“With the image intensifier there are approximately nine steps involved in creating an image, and each step brings with it about 10-15 percent noise,” explained Stephen Green, M.D., associate director, Cardiac Catheterization Lab, North Shore University Hospital, Manhasset, NY. North Shore currently has eight cath labs — all flat panel — which performed 10,000 diagnostic studies, 3,800 coronary interventions and 200 peripheral interventions in 2006. The facility employs several GE Innova systems, including the Innova 3100.
In contrast, “flat panel systems can produce an image in two steps, which dramatically reduces the possible number of sources for error and chances for image degradation,” Dr. Green said.
“Image intensifiers are bulkier and limit the movement of the cameras,” added Katrina Dunn, RN, director of Methodist Hospital’s DeBakey Cardiac Cath Lab, Houston, TX. For the past seven years, Methodist Hospital has used the Siemens AXIOM Artis. “Flat panel detector systems give a more discrete image of the anatomy. More acute angles separate out vessels that have a tendency to overlap, opening up the coronary tree for optimal visualization.”
North Shore, says Dr. Green, has also experienced better visualization of the vessels in obese patients with the flat panel systems, and they make it easier and quicker to do peripherals on all patients.
For the most part, Jon R. Resar, M.D., agrees. Dr. Resar is associate professor of Medicine/Cardiology, director, Adult Cardiac Catheterization Laboratory and director, Interventional Cardiology at Johns Hopkins Hospital in Baltimore, MD.
“Image quality is clearly what sets flat panel detector systems apart from image intensifiers. In my experience, flat panel technology allows better visualization of stents and may be better for procedures such as digital subtraction angiography (DSA) for myocardial perfusion, image stabilization and 3D reconstructions,” said Dr. Resar. “But it does not have a huge impact on the day-to-day functioning in the coronary arena.”
Reducing Radiation’s Punch
Since their introduction seven years ago, flat panel systems have done more than produce clearer images.
“A major advantage of flat panel systems over image intensifiers has been the reduction of X-ray dose to the patient and the people in the room,” said Dr. Green.
Published studies prove, according to Dr. Green, that in 2000 when North Shore switched from an image intensifier system to a FPD system, they experienced a 30-50 percent reduction in X-ray dose both on cine and flouro procedures.
FPD technology, says Dr. Resar, has brought about increased consciousness regarding radiation exposure and dosing. In fact, the electrophysiology (EP) group at Johns Hopkins, he says, has published articles in conjunction with the hospital’s radiation safety officer examining radiation dosing administration during complex, long flouro exposure EP studies.
“However, I am not convinced that flat panel detector technology actually reduces radiation exposure,” Dr. Resar said.
He cites a recent ACC abstract where Australian researchers examined radiation exposure pre- and post-FPD technology. Interestingly, he says, according to the study, radiation exposure was actually greater with FPD technology than with conventional image intensifier technology.
So what’s a cath lab to do?
“I believe hospital radiation safety personnel need to perform very thorough measurements of radiation exposure for the equipment when it is first sited, rather than relying on vendor claims alone,” advised Dr. Resar.
Two-in-One Solution
With the newer dual–plane angiography systems, many integrate two C-arms into one system. Such a set-up can be useful for hospitals that require one room for both coronary and peripheral applications. Johns Hopkins installed Toshiba’s Infinix I Series dual-plane system about eight months ago for just that purpose. One C-arm is dedicated to cardiac work, while the other is optimized for peripheral studies outside the heart.
Dual-plane systems, like Philips’ Allura Xper FD10/10, reportedly simplify complex EP procedures, while improving workflow and productivity, by providing instant visualization of catheter positions from two directions.
One of Methodist Hospitals’ seven cath labs contains a bi-plane system, used primarily says Dunn, for imaging more complex cardiac anatomy.
“By providing an additional dimension to your imaging, bi-plane systems are useful for studies of patients with renal disease because you can see both planes at the same time with reduced contrast to the patient. The additional point of reference is also beneficial when going across the atrial septum (transseptal),” said Dunn.
While a two-in-one solution may be ideal for some users, others may not require the additional functionality.
“Different groups of physicians have different need requirements. In general, for interventional cardiology, I don’t feel there is a significant need for bi-plane flat panel or image intensifier systems at this point. However, I do think there are certain groups of physicians who do better with them: electrophysiologists for their ablations, for example, and neuroradiologists,” said Dr. Green.
Reshaping the Catheterization Suite
With flat panel detector technology already a standard of care, what’s next for the cath lab?
One trend that Dr. Resar foresees is multimodality imaging.
“We have a plethora of imaging equipment in our adult and pediatric cardiac cath labs,” said Dr. Resar. “We replace equipment in rooms as needed with the most up-to-date technology available.”
Now that Johns Hopkins is building a new Heart Institute, they are deciding on what complementary technology to include, considering, for example, intracoronary ultrasound, virtual histology, stereotaxis and even MR imaging.
But the cath lab is not simply the imaging train anymore, there are a lot of inter-related technologies being utilized in the catheterization suite, says Dr. Resar. Procedures such as structural valve replacement and heart disease valve modification are turning the cath lab into a surgical suite as well. Enhanced flat panel technology has brought vascular specialists into the cardiac suite, adds Dunn. “Now we have cardiologists, interventional radiologists and vascular surgeons sharing the same space,” said Dunn.
More than just technology that produces clearer images, FPD systems are the catalyst behind the transformation of the cath lab from a pure cardiology center to one where physicians from across different specialties can practice.

 October 24, 2025
October 24, 2025