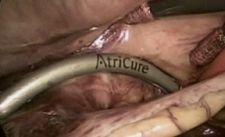
The bipolar clamps from AtriCure build on both the Maze and CA surgeries.
In the past, patients with atrial fibrillation that came to Virginia Commonwealth University Health System (VCU) had several treatment options. There were medications to attack the complex and confusing condition. There were surgical options, involving different intensities and approaches. But according to Vigneshwar Kasirajan, M.D., chair of the Division of Cardiothoracic Surgery, it wasn’t enough.
“We were nowhere near where we should have been, or where we wanted to be,” he said.
With the adoption and implementation of the Mini-Maze procedure, VCU now has a potent weapon in the fight against atrial fibrillation.
While the most commonly used approach to treating atrial fibrillation (AF) has been the open-chest approach of the Cox-Maze procedure, the Mini-Maze techniques use small incisions between the ribs, are performed on the normally beating heart, hence do not require cardiopulmonary bypass, and make few or no true incisions on the heart other than one when removing the left atrial appendage.
There are multiple types of Mini-Maze procedures, including the epicardial bipolar RF ablation with removal of the left atrial appendage and the ligament of Marshall, also known as the “Wolf MiniMaze.” There is also the “microwave minimaze,” which is less invasive, uses microwave energy, makes smaller incisions, yet, unlike the Wolf Minimaze, the microwave method does not evaluate what are the causes of the AF itself.
With innovative technologies that support the minimally invasive procedure entering the surgery room, AF treatment has become more effective. VCU adopted bipolar ablation clamps developed by Atricure. This series of clamps called the Isolator together, with a generator called the AtriCure ASU, deliver radiofrequency current in a bipolar fashion. The Isolator multifunctional pen can pace, sense, stimulate and ablate cardiac tissue, providing feedback to both the surgeon and electrophysiologist that the lesion lines created have electrical isolation.
Through the continued application of the Mini-Maze technique, using state-of-the-art instruments, the physicians at VCU hope to provide an important alternative for patients whose lives have been dominated by the disease. And perhaps, a final cure for its ravages.
Frustrations with A-Fib
The existing situation with AF at VCU and elsewhere left much to be desired. As many cardiologists know intimately, AF is a serious arrhythmia condition that significantly reduces patient’s quality of life. Ultimately, it can lead to dangerous complications like irreversible heart damage and stroke. The latest estimates from the Mayo Clinic indicate that more than 5 million Americans experience the symptoms and compromised health of AF, and that number is expected to increase to 12-15 million by 2050.
AF is a notoriously difficult condition to treat. One problem that VCU physicians and surgeons contended with is the variety of rhythm disturbances that are grouped under the title of “atrial fibrillation.” They saw with their patients the unpredictable nature of the disease: severe symptoms developing without warning and without a specific activity, and lasting for minutes, hours or days. AF can and does take over a patient’s life.
While the knowledge surrounding AF is evolving in the field, treatment at VCU was hindered by the complexities of the disease. Medications have been spotty in their efficacy for AF. Surgical treatment was the traditional add-on during open-heart surgery for other cardiac conditions; the MAZE surgery involved full heart-lung bypass to allow for multiple incisions in the heart’s upper chambers. Big drawbacks, of course, were the significant hospital stay, long recovery and multiple risks. In addition, only a small subset of patients would qualify due to the risks. Patients enlisting this treatment were often quite sick and very symptomatic with their AF, and their vulnerability could introduce even more risks and complications.
Alternatively, surgical treatments just for AF utilize catheter ablation (CA), which is not open-heart surgery, yet is an invasive treatment nonetheless. Electrode catheters are wound from the groin or neck into the heart in order to cauterize or freeze tissue. For single arrthymias, catheter ablation has become the go-to care with high efficacy rates, eliminating damaged tissue and restoring electrical rhythms to normal. But for AF, ablation is more extensive, represents more risks and is less immediately and permanently successful.
Advancement with Mini-Maze
With these surgical treatments limited in their use and expansive in their risk, the Mini-Maze procedure represents an important improvement for VCU and in the greater world of AF. Now patients experiencing the erratic and rapid heartbeats that take over their day-to-day can receive minimally invasive surgery on a stand-alone basis.
“The impact of Mini-Maze procedures is big,” said Kasirajan. “It’s the most comprehensive approach to AF, giving us results that are the closest to what we want. For my first 40 patients, I had a 75-80 percent success rate.”
The Mini-Maze in combination with the bipolar clamps builds on both the Maze and CA surgeries, offering a distinct set of advantages over typical CA procedures:
• Delivers full transmural lesions without damage to nearby healthy heart
tissue and functionality;
• Uses a bipolar energy source to sense complete ablation and alert the surgeon;
• Tests and ablates ganglionic plexi, another area of the heart that can cause arrhythmias
• Removes the left atrial appendage, in which most blood clots form;
• And tests during the surgery to make sure that no further errant electrical activity is present.
Reliability in Results
While multiple Mini-Maze methods exist, VCU is finding sustainable success with Mini-Maze through Atricure.
“In my experience, we’ve found a very high cure rate,” said Kenneth Ellenbogen, M.D., vice chair of Cardiology at VCU. He also serves as director of Clinical Cardiac Electrophysiology and Pacing. “It’s allowing us to treat atrial fibrillation earlier, when patients have shorter or intermittent episodes. We don’t have to wait until something else has failed and risk all the complications of a much more invasive surgery. This gives patients a better chance of successfully treating the condition and controlling it long term or curing it completely.”
According to Kasirajan, the potential to eliminate AF is the key draw for the minimally invasive treatment. By putting the heart back to its normal rhythm, and avoiding other issues or side effects in the process, there is great potential for patients to go off their anti-arrhythmia medications and the standard doses of coumadin. While it doesn’t happen overnight, it can and does happen. In VCU’s treatment experience, approximately 70 percent of patients are able to do just that.
The ability to produce reliable and assessable results is another draw. With previous CA treatments, and with the standard MAZE surgery, one of the biggest challenges is to show that procedures performed are effective. According to Dr. Kasirajan, CA in particular has had many mixed signs in follow up, and many patients are not followed long enough to give accurate information on treatment aftermath, leading to a nebulous atmosphere of uncertainty around the actual results of the therapy. Mini-Maze offers a chance to start anew with a system posting good results thus far.
Besides its potential as a condition cure, one of the most important advantages to Mini-Maze may simply be the option it provides to patients, a group of people who have long had limited options when it comes to treatment.
“We’re seeing patients excited about another viable treatment option,” said Dr. Ellenbogen. “On top of treating AF, the procedure may reduce risk of stroke, a crucial advantage. And anything associated with the long-term treatment of AF, and the subsequent ability to get off heparin, can save energy and costs for patients.”
With the potential to treat and even cure atrial fibrillation, Mini-Maze is allowing VCU to provide improved patient care. As more and more hospitals utilize the technique, patients with atrial fibrillation stand to benefit, and get their lives back.