We are at an inflection point with many aspects of medicine, not the least of which concerns choosing the correct tool to discover and manage coronary artery disease. The American landscape of clinical and imaging service providers is going through a major reshuffle. Coronary computed tomography angiography (CTA) is growing in utilization, taking its place as an established modality with AHA, ACC and ACR society-derived appropriate use standards. However, this growth in CT utilization and the resultant growth in per capita radiation exposure have elevated a public debate about the risk of causing cancer versus the value of its information.
Is this just a lot of radiation to get a pretty picture that adds nothing? Or is it the fruit of the computer age and a terrific new test that will diagnose and risk stratify patients with trivial risk of anything, cancer included? Advocates and critics abound in this dialogue, as does the uncertainty about radiation.
But if you, the reader, inwardly feel this is confusing and you don’t know where you actually stand on radiation risk, you are amongst a club of 99 percent of the radiology and cardiology community today. This is a murky area with confusing terminology. The answers regarding risk depend on what the patient characteristics are and how the scan is performed. And if you, the reader, think that CTA is a sideline test and not about to become a major diagnostic modality, then the meaning of phrases like “gatekeeper to catheterization,” “pre-certification” and “justification of medical necessity” have not soaked in yet. This is an attempt at a balanced discussion, looking at several key questions.
Where Are We Now With Retail CTA?
Excellent workhorse CTA scanners (64-slice) are now nearly ubiquitous in the metropolitan United States. That is to say, noninvasive CTA for suitably selected patients is readily available.
Additionally, fresh iterations of scanners that provide improved images at lower radiation dose to a wider swath of patients have arrived, including scanners with two sources of radiation, high-pitch performance and detector arrays of 256 to 320 channels. Of course, these newer scanners are costly. Also, standards for scan performance and reporting have been implemented, as have policies for radiation safety, appropriate use and lab accreditation. More ominously, we are seeing more pressure from payers to shift decision-making away from providers to ACO organizations and payer surrogates, like radiology benefit managers (RBMs).
What is the Issue of Radiation?
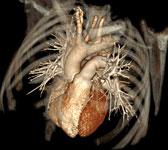
It is the balance of risk of cancer and downstream testing of purported “positive” tests, versus the benefit of an accurate image of the coronary arteries. This is at a time when researchers and practitioners do not agree on what is risk and, in fact, what is clinical benefit?
Why is Low Dose Important?
First, the dose estimate is a calculation from the scanner metrics derived from CT protocols and patient physical characteristics. Most medical researchers studying and comparing different radiation-based modalities have settled on “equivalent dose.” It is readily derived after a scan is complete (dose length product times a weighting factor), but it is at best a rough approximation of the scan exposure pointing toward a five- to 20-year risk of consequential cancer. There may be up to a 40 percent underestimation of the true equivalent dose, so there may be a significant underestimation of the risk this number is meant to convey. Yet, it is the best we can practically do.
Second, if we accept dose uncertainty, we also have to accept that at CT scan doses, there is no direct epidemiological data that supports the risk of developing a new cancer. Plus, we have background radiation from a myriad of sources, and we have a “natural causes” cancer mortality of 25 percent.
Let us accept the idea that any radiation is theoretically bad (this is called the linear no-threshold theory), but we must also accept the reality that the health risk of missing coronary artery disease is probably worse than the low likelihood of developing a cancer as a result of a CTA. This premise is less certain in younger, particularly female, patients.
Hence, we use “effective dose” to get a very “soft” approximation of an X-ray exposure risk that may or may not even be a risk. Small wonder we are perplexed. Hopefully now with this public debate, CT scan technologists will configure the machine variables and protocols to minimize dose without compromising scan value: A low dose scan may be unreadable if not planned correctly. The initial 25-35 mSv scans of the early CTA days are now typically down 60 percent in a broad sampling registry (PROTECTION 1).
For 64-Slice Scanners, How Can Dose be Reduced?
Most of us associate 64-slice scanners for CTA work with early criticism of unacceptably high radiation exposure. In 2009, Gilbert Raff, M.D., and others published a study of 5,000 patients undergoing cardiac CTA on 64-slice scanners, utilizing spiral technique and retrospective gating. They assessed the impact of a dose reduction planning strategy on patients and their images and demonstrated radiation exposure could be halved by:
• tightly limiting scan coverage to the coronary arteries;
• pulsing the tube current to be “on” during a brief diastolic window, and
• reducing the tube potential from 120 to 100 kV when patient size allowed.
They reported no degradation in image value and brought dosages down to the 10 mSv range. The message is clear that with careful attention to scanner setup, spiral CTA can be offered at dose levels comparable to direct angiography and well below nuclear perfusion functional imaging.
This study is important because it does not lean on newer and more expensive technology for dose reduction. Furthermore, in cases with heart rate regularity at or below 60 beats per minute, software upgrades to these systems can enable prospective electrocardiogram (ECG)-triggered scans to be performed. Dosages well below 5 msV (a 70 percent drop) are the norm with this scan technique (PROTECTION 3 study).
How is Dose Meaningfully Reduced on New Scanners?
In scanners with wider detector arrays (256 to 320 channels), the entire heart can be sliced into high-resolution cuts in one or two heartbeats. Gantry rotation is slower and, therefore, ideal heart rates are still 65 or less. But with heart rate suppression via beta blockade, diastolic ECG-triggered pure axial scanning is routine. There is no need for continuous table travel and continuous radiation delivery, current-pulsed or not. For thinner patients, the tube voltage can also be reduced to drop radiation further. These scanners regularly deliver effective doses of 3 mSv or less.
Dual-source scanners, available since 2009, capable of high pitch acquisition, have enabled very quick Z-axis coverage without information gaps, resulting in very low radiation exposure (typically 1 mSv). Single heartbeat acquisition of scan data is possible, but the slow heartbeat caveat remains. Lower tube voltage potential at 100 kV yields sub 1 mSv CTA.
Both of these scan situations gather a single image volume and, therefore, regional or global chamber motion is not available. Since other imaging modalities can capture this information, however, it is not out of the providers’ easy reach if needed.
Regardless of the scanner used, tailoring the scan protocol for the question asked can allow lower tube current settings and provide dose reduction regardless of the scanner generation used. For example, when maximum spatial resolution is not required, as in left ventricular functional display, complex congenital heart disease, or atrial and pulmonary venous anatomy, thicker slices at lower tube current settings should be chosen. And, as yet clinically unvalidated but on the horizon, a new image processing technique called iterative reconstruction is being tested. This is signal processing to allow diminution of image noise and, therefore, the opportunity to scan at lower tube voltage and current settings.
It is clear that in 2012, coronary CTA can be performed at or below radiation levels considered significant for cancer risk. This is true on upgraded 64-slice scanners and all new-generation scanners. When routine 1 mSv or less scan exposure is more widely available the breadth of clinical indications for in-depth knowledge of the presence, location, severity and bulk of atherosclerosis, even in patient risk cohorts for screening, will grow substantially. Regardless of the view of radiation and cancer risk, not much radiation (one-third of individual annual exposures from all external sources) is simply that: not much radiation.
Editor’s note: Carter Newton, M.D., FACC, is assistant professor of radiology and assistant clinical professor of cardiology at the University of Arizona, Tucson. He also serves as a member of the DAIC Editorial Advisory Board.

 February 02, 2026
February 02, 2026