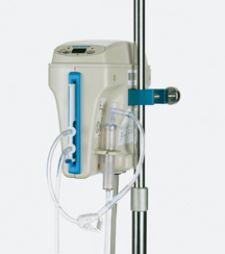
Photo courtesy of Gaymar
Induced hypothermia has traditionally been used perioperatively as a strategy for neurological protection during major vascular surgery or for situations where neurological injury is present or imminent. However, patients cannot deviate off of the normal core body temperature of around 37°C for long without risk of deleterious effects. Studies have shown that hypothermia can lead to a variety of serious complications, including coagulopathy, dysrhythmias, myocardial ischemia and a decreased resistance to surgical-wound infection.
Several factors can contribute to unintentional development of hypothermia during surgical procedures, including a cold surgery room, anesthesia and the infusion of fluids at room temperature. However, a growing body of evidence suggests that the maintenance of perioperative normothermia is associated with improved outcomes, prompting clinicians to take a proactive role in thermal management.
Although a variety of convective methods are available, Joseph Haymore, MS, RN, CNRN, CCRN, ACNP of NeuroCare Associates in Silver Spring, MD, says that intravascular warming continues to be the fastest way to warm patients.
Hitting the temperature bullseye
Haymore, who is responsible for pre- and postoperative management and neurocritical care, says that although most temperature management in neurosurgical procedures involves induced hypothermia, intravascular warming can and does come into play.
“Even during induced hypothermia, you don’t want to go below 30 or 31°C, because then the complication rates go up significantly,” he said. “When you start cooling a body, the body cools at a certain rate. If cooling isn’t slowed as the target temperature is approached, that target can be surpassed and the patient will require warming.”
Although a convective heating device is kept on hand for patients who cannot tolerate additional fluids, Haymore says that intravascular warming is the first choice for patients who need rapid rewarming when desired temperature is overshot.
The devices that Haymore’s practice uses for temperature management are Gaymar products, the Medi-Therm III for conductive cooling and the Medi-Temp III for intravascular warming. A lightweight device that can be mounted to a IV stand, the Medi-Temp III heats infused blood or fluids via sterile disposable, non-pyrogenic, latex-free cassettes that are easily loaded on the side of the device.
“I think the biggest thing the Gaymar products bring to us is that they are straight forward and user friendly,” he said. “There is a lot of work that goes into making the machines intuitive, and they are quite reliable.”
In fact, Haymore notes, the improvements made in the latest models have cut down on the number of cases for which the target hypothermic temperature is surpassed.
“The machines sense temperature, and the newer machines do this much better,” he explained. “So when you get close to whatever you’ve set as your target temperature, the rate of cooling decreases so that when the patient hits the target temperature, heat loss and heat production will be the same and the target temperature is maintained. That’s the perfect scenario.”
Old problem, simple solution
According to Carl Schulman, M.D., M.S.P.H., assistant professor of Surgery at the University of Miami, Miami, FL, there are two reasons a burn surgery is stopped: One, the patient loses too much blood, or two, the patient gets cold.
“Most all of our burn patients who are really badly burned have a multitude of problems, but one of the major ones is temperature regulation,” Dr. Schulman said. “We make that worse by taking patients to the operating room where we have to uncover them completely, from head to toe, to attend to a big burn. And we can only work for as long as the patient can stay warm.”
To provide comfort to the patient and extend the amount of time they are able to operate, Dr. Schulman would set the burn room temperature to over 100?F. Unfortunately, the result was a very uncomfortable medical staff. “The room temperature thing sounds like a small inconvenience,” he commented, “but really, I think most people would agree that when you’re hot, sweaty and uncomfortable, you’re probably not doing your best work.”
Enter a colleague in neurosurgery, who while visiting the burn center one day suggested to Dr. Schulman that he consider a device used in both the neurosurgery and cardiac units for temperature management. The Alsius Thermogard system warms the patient via temperature-controlled saline circulated in a closed-loop balloon sitting within the central venous catheter. An estimated 30 surgeries later, Dr. Schulman has never looked back. He has since been able to operate on an almost completely exposed burn victim for more than four hours, a length of time previously impossible.
“When I discuss this with colleagues, I call it a no-brainer,” he said. “The technology is not complicated; it’s essentially running warm water through balloons in the middle of the catheters we normally use. The catheter is bigger than a normal catheter by a few centimeters, but in every other respect it’s just a central line we use routinely in all of our patients. So from my perspective as a surgeon, there really doesn’t seem to be any added risk to the patient.”
Although use of Thermogard increases the costs associated with surgery, Dr. Schulman suspects that the extended time afforded in surgery may ultimately reduce the number of surgeries patients with large burns have to undergo.
The technological diversity among intravascular temperature management devices reflects in part the variation in requirements of different hospitals, practices and types of patient. Take, for example, trauma or surgical patients who suffer significant blood loss. The rapid, high flow infusion of crystalloid, colloid or blood product may be indicated for volume replacement in these patients, but this can lead to unwanted hypothermia when the fluids are administered at room temperature. Designed to address this problem, the Level 1 H-1200 Fast Flow Fluid Warmer (Smiths Medical), which accommodates standard blood/solution bags and maintains pressure at 300 mmHg, allows rapid infusion of fluids warmed via a counter current 42°C circulating water bath. It also provides protection from air in the line through the use of an integrated air detector/clamp that detects the presence of air, alerts users with audible and visual alarms, and then clamps the line closed to prevent the air from reaching the patient.
Belmont Instrument Corp. produces a compact intravascular warming device, the Buddy Fluid Warmer, which uses dry heat technology to warm fluids. The power module can be placed on an IV pole, but the heating unit — containing dual heater plates and weighing in at a mere 3.5 ounces — is placed next to the patient, shortening the distance traveled to the infusion site to prevent the heated liquid from cooling in the line. The Buddy can warm cold fluids to 38°C at flow rates as low as keep-vein-open (KVO) and as high as 100 ml per minute, automatically self-primes, removes out-gassed air from crystalloid and sounds an alarm when fluid runs out.
“I had never heard of intravascular warming, and when we tried it, we were really surprised at how easy it was and how well it worked,” reported Dr. Schulman. “It has really worked beautifully for us, I have no complaints.” <
Sources are available online at www.AcuityCare.net.
Sources:
http://ccforum.com/content/8/5/R343
http://content.nejm.org/cgi/content/extract/336/24/1730
http://www.anesthesia-analgesia.org/cgi/content/full/90/2/286
http://www.anesthesia-analgesia.org/cgi/reprint/97/4/1064.pdf
http://www.belmontinstrument.com/pdf/BelBuddy_handout4.pdf
http://www.belmontinstrument.com/buddy/specs.html
http://www.aspan.org/PDFfiles/HYPOTHERMIA_GUIDELINE10-02.pdf

