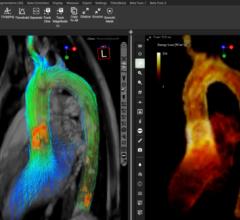
Methodist DeBakey Heart and Vascular Center in Houston, Tex., has leveraged new imaging and interventional technologies to help contain and reduce costs, increase patient volume and revenues and build a reputation as a state-of-the-art heart center.
“Efficient modalities and other technologies that speed patient care and improve outcomes have meant faster outpatient visits, shorter inpatient durations and have also helped us use our resources — including our staff — more efficiently,” said Karla M. Kurrelmeyer, M.D., FACC, FASE medical director, Methodist DeBakey Cardiology Associates Practice Physicians.
These interventional and hybrid technologies include transcatheter aortic valve replacement (TAVR), endovascular aortic aneurysm repair (EVAR), robotic electrophysiology (EP) and interventional procedure navigation systems, and a team approach and use of hybrid operating rooms (ORs). Other innovations include use of the latest cardiac imaging systems, including 3.0T magnetic resonance imaging (MRI), pre-hospital ECG for earlier activation of the cath lab in STEMI cases, and leadership as a top cardiovascular surgical training center.
“These technologies (EVAR and TAVR) have brought less-invasive alternatives to complex and high-risk patient populations,” said Michael Reardon, M.D., FACC, FACS, medical director of the cardiovascular operating rooms.
These unique technology offerings have caught the eye of other facilities in Houston and around the state of Texas, which has increased the number of referrals, Kurrelmeyer said.
TAVR and EVAR in the Hybrid OR
DeBakey has 10 cath labs, 10 surgical ORs and two hybrid ORs. Reardon said he wishes he had more hybrids, because that is where some of the most innovative procedures are performed and where the future of medicine is headed. The hospital is a leading center for EVAR, thoracic endovascular aortic repair (TEVAR) and hybrid approaches to complex thoracic aneurysms. Use of EVAR and TEVAR has helped reduce the cost of treating these patients, Reardon said.
“With EVAR and TEVAR, what’s really innovative to me is that we have done more procedures and have more experience than many other centers,” Reardon said.
He said DeBakey has moved beyond basic stent grafting to much more complex hybrid interventions for TEVAR. “What we do is rebuild the aortic arch,” he explained. This is accomplished using bypass grafts on the ascending aorta to redirect blood flow so the brachiocephalic, left common carotid and the left subclavian arteries can be occluded for easier stent grafting.
“We have certainly seen our endovascular aortic volume going up, but the real growth has been seen in TAVR,” Reardon said. “Everyone who walks though my door now asks to have TAVR.”
Due to the limited indication for the Sapien and CoreValve only for high-risk surgical patients who do not qualify for surgery, most of these patients are told they only qualify for surgical repair. As with centers that participated in the Sapien PARTNER trial, DeBakey has seen a big influx of new patients who want TAVR, but only qualify for open surgical repair, boosting surgical referrals.
“The first year we were in the CoreValve trial we saw a 25 percent increase in our surgical valve repair volume,” he said.
DeBakey is a leading implant center for the CoreValve U.S. pivotal trial for Medtronic’s transcatheter aortic valve. It also offers the Edward’s Sapien transcatheter aortic valve. Both valves are restricted to use in high and extremely high-risk surgical patients. Reardon serves as an investigator for the CoreValve U.S. trial and will be the national principal investigator for the upcoming SURTAVI trial. That trial will investigate the use of CoreValve in intermediate-risk surgical patients and is expected to get underway in the United States by the summer of 2012.
“We are one of the few institutions in the United States that has access to both TAVR devices,” Reardon said. “Soon we will be able to offer TAVR devices to a spectrum of patients, ranging from extremely high-risk to intermediate-risk surgical patients.”
In Europe, where the CoreValve and Sapien have been on the market a couple of years, Reardon said about 30 percent of all tissue valve implants are now performed with the transcatheter valves. At major European heart hospitals experienced with TAVR, he said about 50 percent of valve replacements are now performed with transcatheter devices. That same rapid rate of adoption is expected to take place in the United States.
“I think five years from now, the way we approach valve replacements will be fundamentally different than it is now because of transcatheter valves,” Reardon said.
Robotic Navigation Systems
To increase the accuracy of interventional procedures and decrease the amount of angiography radiation dose required, especially during long electrophysiology (EP) procedures, DeBakey has installed several robotic navigation systems. It has a Stereotaxis magnetic EP navigation system and two Hansen Sensei EP robotic systems. It also received the nation’s first Hansen Magellan peripheral vascular navigation robot for pre-clinical research prior to FDA approval for clinical use.
“The robots we are using and testing in advance of FDA approval make difficult surgical procedures easier,” Kurrelmeyer said. “They also allow our surgeons to achieve superhuman maneuverability and stability during ablative and other intravascular procedures, which equates to reductions in surgery time, less risk and, studies are showing, better patient outcomes.”
“One of our operators started using the Hansen system, and as with anything, there is a learning curve. At first it took longer for procedures. But today, he has the lowest time for ablations,” said Miguel A. Quinones, M.D., MACC, chairman, department of cardiology.
He said an example of the increased accuracy the Hansen system offers occurred after repeated attempts to place an Amplatzer patent ductus arteriosus (PDA) occluder at a difficult angle to seal a mitral paravalvular leak. The robot was brought in and was able to make the small precise movements necessary to accurately deploy the occluder and seal the leak.
Advanced Imaging Technology
DeBakey possesses several advanced cardiac imaging systems. It uses 1.5T and 3.0T cardiac MRIs, 3-D echocardiography, CT scans and a hybrid OR with an angiography system capable of advanced visualization overlays and rotation angiography 3-D, CT-like scans. The facility also uses the latest in gamma camera technology, which only requires about five minutes to image patients. Extensive use of 3-D echo transesophageal echo (TEE) is used to better guide mitral valve prolapse and regurgitation repairs, atrial septal defects (ASDs) and TAVR.
“Cardiac MRIs and 3-D echocardiography take a lot of guesswork out of imaging, leading to better diagnoses and, ultimately, better outcomes for our patients who require these imaging modalities,” Kurrelmeyer said.
DeBakey uses MRI in place of CT whenever possible to cut both iodine contrast and radiation. The center now performs more than 200 cardiac and vascular MRIs each month. Kurrelmeyer said this has made a significant increase in income, and many Houston-area residents who have cardiovascular devices are now directed to DeBakey for MRIs.
“The acquisition of our cardiac MRI has certainly led to an increase in new patients at Methodist DeBakey Heart and Vascular Center, as well as serving as a resource for our existing heart and vascular patients,” Kurrelmeyer said.
The facility also uses Plato’s Cave, a room with a touch-screen table to rotate and slice through CT, MRI or echo datasets that are projected in true 3-D on the wall. “We have used our 3-D cave with patients whose vascular architecture is unusual and potentially confounding for open-heart surgery, finding safer surgical routes to points of intervention and making surgery less dangerous for these patients,” Kurrelmeyer said.
“Generally, we strive to use specific modalities to answer specific clinical questions, rather than simply ordering batteries of tests, many of them unnecessary, which can subject patients to extra stress and discomfort. These also run up extra costs for the hospital and American healthcare in general. We can do this because we have the diversity of modalities needed to address any clinical question with great specificity,” Kurrelmeyer said.
“We are one of only a small number of centers where all the imaging modalities are located in the heart center,” Quinones said. “This allows, under one roof, side-by-side imaging studies at one time.”
A Leader in Surgical Training
The 35,000-square-foot Methodist Institute for Technology, Innovation, and Education (MITIE) offers one of the most advanced educational and surgical training facilities in the United States. It has simulators for both endovascular and cardiovascular thrombo-embolic events. MITIE trains surgeons to do procedures with greater accuracy and more quickly, shortening surgery time and improving outcomes, which reduce costs. It has trained more than 1,000 surgeons from hospitals around the world to do new or tricky procedures, either at our facility or distally via live, interactive audiovisual feeds.
“MITIE is a unique resource that has improved surgeons’ skills and their skill sets, and patients benefit directly from that, whether they live in the Houston area, New York, or Dubai,” Kurrelmeyer said. “We don’t only train surgeons, however, we train surgical teams, including nurses, technicians, and anesthesiologists, using our simulators of complete surgical suites.”
The team approach is essential for the successful operation of hybrid ORs, which DeBakey also was a pioneered. Early experience with its hybrid room translated into a need for better teamwork training and coordination between specialists.
Our hybrid OR allows immediate imaging during surgical procedures, which numerous studies have shown improves outcomes for patients whose cases present special difficulties, and also provides the backup of open procedures if minimally invasive procedures prove inadequate.
MITIE and DeBakey’s clinical research program have presented an alternative revenue stream to the heart center.
Other Unique Services
DeBakey’s Aortic Network of cardiologists and cardiovascular surgeons ensures that patients throughout the Houston metro area, who are experiencing acute aortic problems, can get same-day care or consultations with the center’s doctors. The network allows access even if the patient lives far from the main hospital in the heart of Houston. The network also provides a way for unaffiliated doctors to refer their patients.
To speed door-to-balloon times and earlier diagnosis of ST-elevated myocardial infarction (STEMI), the facility uses LifeNet. The system allows emergency medical services (EMS) personnel to send pre-hospital ECGs to the emergency department while the patient is en-route.


 January 21, 2026
January 21, 2026