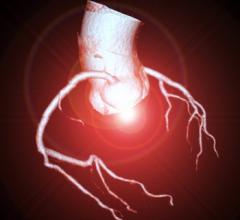
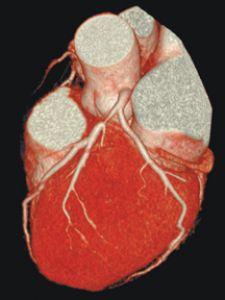
This patient's axial femoral bypass graft is clearly seen in this 3D view. Long term patient follow-up post intervention is an important advantage for MDCT.
More than ever before, cardiologists are adopting CT as the new standard for cardiac care. In the last five years, CT’s popularity as a diagnostic tool has exploded. Its ability to produce slices as thin as 0.5 mm creates a platform for evaluating patients, detecting disease at early stages and designing treatment roadmaps. Today’s advanced 64-slice CT has dramatic advantages over previous imaging technologies for accurate diagnosis of cardiovascular, peripheral vascular and other diseases affecting millions of Americans.
Despite CT’s clinical value in cardiology, there are challenges associated with it as a diagnostic tool, including the fundamental thinking behind traditional cardiac interventional diagnostic approaches, such as catheterization angiograms or cath lab. More importantly, there is a need to convince third-party payers that CT is more clinically accurate than other tests and will ultimately reduce healthcare costs by detecting disease earlier with only one test.
A Brief History of Cardiac Diagnosis
To understand CT’s advantages as a diagnostic tool, one must examine the traditional interventional diagnostic approaches, such as cath lab angiograms, which have been used for years and are common in many hospitals today.
Five years ago, when a patient arrived at my office with symptoms, a series of physiological tests, including an EKG and a treadmill stress test, were conducted. If these physiological tests were inconclusive, which was often the case, the patient would undergo an invasive cath lab angiogram for diagnosis.
Without the ability to see a patient’s anatomy by working with only physiological test results, a large number of healthy patients underwent invasive angiograms, a procedure not worth the risk unless absolutely necessary. Risk of serious complications resulting from catheterization range from one in 1,000 to one in 500. Complications can include bleeding and infection, damaged blood vessels and blood clots. Additionally, physiological diagnostic methods often result in false negatives, in other words, test results appear normal when the patient is actually ill.
How CT Created Another Path to Diagnosis
CT allowed physicians to examine the cause of a patient’s symptoms by detecting disease at the earliest stages. With a high accuracy rate, CT drastically improved diagnostic ability, ensuring that healthy patients went home and sick patients received proper, timely treatment.
64-slice CT changed interventional cardiology by allowing cardiologists to review virtually every aspect of the heart through 0.5 mm slices. Today, CT as a diagnostic tool is beginning to transcend cardiology into other medical specialties to detect all forms of disease.
CT as a Planning Tool
Beyond its benefits as a diagnostic tool, CT can play an integral role as a planning tool in managing disease. Today, patients may endure a series of tests, each accompanied by various degrees of radiation. Often these tests yield inconclusive results only for the patient to later undergo a CT exam.
Using CT as the first test considerably decreases diagnostic time, offers anatomical images superior to those seen in the cath lab and exposes patients to less overall radiation dose than a series of tests. This makes CT an ideal planning tool, first to detect disease (diabetics often have multiple diseased areas), assess the level of severity, identify the greatest risk areas and develop a roadmap for treatment.
Post-surgery, CT images can be used to reevaluate patients by comparing the pre- and post-surgical images to ensure good clinical outcomes. With long-term patient follow-up, CT provides the capability to check for signs of new disease over time.
Reimbursement Challenges
One of the fundamental challenges of diagnostic CT is the ability to convince third-party payers that CT is more clinically accurate than physiological tests and cath lab angiograms for diagnosis and will ultimately reduce healthcare costs by detecting disease, particularly cardiovascular and peripheral vascular diseases, at the earliest stages using a single test. Diagnostic CT spares patients unnecessary radiation, fatigue, time and money associated with undergoing a series of less-effective tests that often end with a CT scan anyway.
Third-party payers typically base reimbursement on the “gold standards” used in the field such as the cath lab angiogram for cardiovascular disease diagnosis. The amount of reimbursement is greater for interventional procedures than diagnostic procedures. Although diagnostic CT offers advantages over these traditional interventional diagnostic methods, it is considered a new technology and is less common, so reimbursement is limited.
Ideally, the CT suite and cath lab would work closely together to improve patient care and offer better patient outcomes by using CT for diagnosis and cath lab for intervention.
Reducing the Risk of CT
Although CT has inherent clinical value for diagnosing and managing disease, the use of radiation and contrast dye are still risk factors. The risk of radiation decreases for patients as they age. There is less concern for senior patients (60 years) than for younger patients whose lifetime radiation exposure is still unknown. Using CT as the first test should reduce the amount of radiation and contrast dye a patient would receive if subjected to other, less-effective diagnostic tests.
CT Studies Show Promise for Validation
There are many studies evaluating CT, but the CorE 64trial is the largest and only multi-center, international trial evaluating 64-slice CT as a diagnostic tool as compared to cath lab angiogram. Initiated by Toshiba America Medical Systems, this is the first study of its kind to sample patient groups from several countries, reportedly offering the most statistical data available to date. The results of CorE 64, which should be available by the end of 2007, could serve to influence reimbursement and the use of CT as a diagnostic tool.
What 256 Slices Can Offer
The most significant advancement on the horizon is the 256-slice* CT by Toshiba, with a beta system that has been clinically tested at Johns Hopkins University School of Medicine’s Heart Institute. This game-changing technology is the world’s most advanced, offering four times the coverage of the 64-slice CT and the capability of imaging an entire organ in a single rotation.
The single-rotation imaging will significantly reduce patient radiation dosage. Imaging the heart in a single beat will produce images at the exact same moment in time, opening
the door to effectively diagnosing a new set of patients – those with abnormal heartbeats.
Perhaps one of the 256-slice CT’s greatest attributes is its ability to provide comprehensive, multi-function data to evaluate perfusion, anatomical and physiological insights, which are currently evaluated using tests from multiple modalities. Visualizing blood flow through the heart, brain and other whole organs will enable physicians to more accurately diagnose disease faster.
256-slice CT is a medical advancement that will allow clinicians to offer their patients more accurate results, less radiation exposure and an overall improvement in patient care. The ability to acquire more data will decrease testing time for patients by completing all necessary tests with one modality, in one location. It also will potentially benefit third-party payers by lowering costs and improving efficiency of diagnosis and treatment.
Today’s 64-slice CT and tomorrow’s 256-slice CT present dramatic advantages over previous imaging technologies for accurate diagnosis. As more physicians realize the benefits of diagnostic CT, and as the 256-slice CT changes the medical landscape, the hope is that third-party payers will offer support through adequate reimbursement, allowing medical professionals to deliver the best patient care available.
* Works-in-progress

 February 06, 2026
February 06, 2026