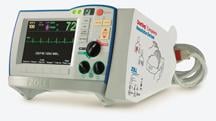
Philips HeartStart MRx enables paramedics to acquire and wirelessly transmit a suspected STEMI patients 12-lead ECG data to the emergency department.
Door-to-balloon time can be used as a quality measure for hospitals in their level of excellence in caring for patients with acute ST-elevation myocardial infarction (STEMI). It can also be used as a conceptual framework for thinking about quality improvement, differences between outcomes-focused and process-focused quality programs.
A classic conceptual model for thinking about quality is to think of quality as having three interrelated components: structure, process and outcome. The advantage of process-based quality programs, such as measuring door-to-balloon time, is that processes can be tightly linked to outcomes. The steps in the door-to-balloon process can be clearly described, easily measured and modified, allowing for continuous assessment and improvement.
The choice of quality (performance) measures is a complex process. A number of factors need to be considered, including the condition affected by the measure, the scientific acceptability of the measure as a determinant of clinical outcome, the usability of the measure and the feasibility for measuring the quality indicator and applying statistical analysis. By these criteria, door-to-balloon time is an excellent quality indicator. There is an enormous scientific rationale for expecting that shortening door-to-balloon times would result in improved outcomes.
Factors to Consider
The relationship between door-to-balloon-time and clinical outcome is probably complex. Less ischemic time, particularly if it is less than two hours, results in less time for cell death and thus, the potential for preserved left ventricular function. This is the “time is muscle” concept. Shorter door-to-balloon-times may be accomplished in hospitals with better processes other than excellent door-to-balloon time, and it may be these other processes that affect outcome. Shorter ischemic times may be associated with higher procedural success rates, so it is the successful procedure rather than time that is critical.
Shorter ischemic times may be associated with better reperfusion. No reflow, poor micro-vascular perfusion despite epicardial coronary patency is seen more often with late rather than early reperfusion. Door-to-balloon times may be longer in the elderly, women, patients with overt heart failure, patients with multivessel disease and patients with significant co-morbidities, all of which may adversely affect outcome. Although the association between door-to-balloon-time and outcome appears to be convincing, the mechanisms underlying this association may be complex.
A number of process factors are associated with superior door-to-balloon time. There needs to be an explicit goal of reducing times. It is mandatory for senior management and physicians to support the program. The process should be broken into manageable segments and there should be flexibility in developing solutions for each segment, reflecting the reality of the particular hospital. Successful programs need strong individual clinical leaders and collaborative interdisciplinary teams, including but not limited to emergency medical services (EMS), the emergency department (ED) and the cath lab. There should be data feedback so the teams can monitor progress to identify problems and successes. Finally, there needs to be an organizational culture of persistence and collaboration. Finger-pointing and assignment of blame for failure to achieve a good time is an easy and predictable response. However, the constructive response is to recognize quality is about process, not about individuals, and failures in quality are failures in process.
Strategies to Reduce Times
Specific hospital strategies have been identified as being important to improve door-to-balloon time. Of particular importance are early cath lab activation by the ED, effective use of pre-hospital ECGs and data feedback. Cath lab activation by the ED prior to the patient being assessed by a cardiologist has been a difficult step in many centers. Our experience at The Medical University of South Carolina (MUSC) in Charleston was that a number of cardiologists initially were uncomfortable allowing ED personnel, without cardiology consultation, to activate cath lab physicians and staff. However, once implemented, it was quickly found the ED can do an excellent job in correctly identifying appropriate patients for immediate catheterization. This single step saves enormous amounts of time.
In Charleston, most STEMI patients who call EMS have an ECG performed in the field, which is transmitted to the hospital. For patients transported by EMS, it is frequently possible to call a “STEMI ALERT,” our name for a single page that notifies all key personnel a STEMI patient has entered the system. The paging operator gives a single page, which activates the cath lab, interventional cardiologist and key personnel such as the CCU charge nurse and nursing supervisor prior to the patient’s arrival. Initiating the process while the patient is still in the field resulted in door-to-balloon-time of less than 30 minutes.
In 2005, median door-to-balloon time at MUSC was about 120 minutes with wide variability. We established goals of both decreasing median time to treatment and also eliminating variability. The times were carefully tracked, as was each step in the process. Key steps included door to ECG being performed, ECG to activation of the STEMI ALERT, time from alert to arrival in the cath lab and time from cath lab arrival to balloon inflation and successful reperfusion. By the first quarter of 2007, our median time was around 60 minutes, with nearly all patients having times of less than 90 minutes.
This model has been adopted by hospitals across the country with excellent performance. This dramatic improvement in STEMI care has been led by and documented by the Door-To-Balloon Alliance and the American College of Cardiology.
The next step for progress includes creating best processes for short door-to-balloon times and making them universal in all hospitals performing urgent STEMI PCI. In addition, we need to move the process one step back in time when the first medical provider (usually EMS) makes contact with the patient. The ultimate goal of shortest possible symptom-onset to balloon time will also require improved recognition and response by affected patients. Finally, state-wide STEMI networks for the delivery of care should be developed. South Carolina has embarked on such a program in association with the American Heart Association Mission: Lifeline program in partnership with the State Hospital Association, ACC, the South Carolina College of Emergency Physicians and the Department of Health and Environmental Control. The goal of this program is to assure every STEMI patient in South Carolina receives optimal, evidence-based care including as rapid as possible reperfusion. This program will depend on multiple key players including EMS providers and hospitals delivering PCI care.
Dr. Eric Powers is a professor of medicine and the medical director of the Heart and Vascular Center at MUSC. He is currently chairman of the Steering Committee for The South Carolina Mission: Lifeline Project developing a statewide STEMI program.



 January 15, 2026
January 15, 2026 









