April 8, 2011 – A Canadian research team found that the radial artery outperformed the saphenous vein as the best conduit for coronary artery bypass graft (CABG) surgery. The radial artery also led to reduced rates of functional or complete graft occlusion, according to research presented this week at the American College of Cardiology’s 60th Annual Scientific Session.
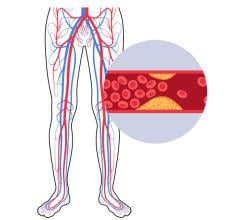
The study was conducted at 13 centers across Canada and enrolled 561 patients who underwent CABG surgery for three-vessel disease. Each patient received both a radial artery (the major artery in the thumb side of the arm) graft and a saphenous vein (the main leg vein) graft at two different diseased vessel sites. The primary endpoint of functional graft occlusion was determined through invasive angiography at least five years after surgery. The secondary endpoint was complete graft occlusion determined through invasive angiography or computed tomography angiography.
The research team conducted late angiography on 440 patients alive at one year and on 269 patients at a mean of 7.6 (+1.5) years post-procedure. In the latter follow up, the researchers found that significantly fewer radial arteries became partially occluded than saphenous vein grafts, at 12.0 percent and 18.8 percent, respectively (p = 0.05, odds ratio [OR] 0.64, 95 percent confidence interval [CI] 0.41 – 0.98). Significantly fewer radial arteries also became completely occluded, at 8.9 percent, than saphenous veins, at 17.8 percent (p = 0.004, OR 0.50, 95 percent CI 0.32– 0.80).
In the researchers’ previously published one-year results, complete graft occlusion was significantly reduced in the radial artery compared to the saphenous vein, while partial graft occlusion was similar between the two conduits.
“Our study shows that the radial artery does seem to offer an improvement in graft patency compared to vein grafts,” said Stephen Fremes, M.D., MSc, lead study author and head of the division of cardiac and vascular surgery, Schulich Heart Centre, at Sunnybrook Health Sciences Centre in Toronto.
Cardiac specialists have long debated which conduit provides better long-term graft outcomes. Many believe that the radial artery is superior to the saphenous vein because arterial grafts develop fewer diseases and better withstand aortic pressure. However, most of the studies proving this have been done using the left internal thoracic artery, not the radial artery.
“The left internal thoracic artery was shown in the 1980s to be superior to a vein graft, and as a result, there was a wave of enthusiasm to use this artery – as well as other arteries – for either more complete arterial revascularization or total arterial revascularization,” Fremes said. “The radial artery possesses some advantages relative to the internal thoracic artery; it has thicker walls, which makes suturing easier, and a greater length that can reach all targets on the heart.”
In addition to finding lower rates of occlusion in the radial artery grafts, the research team also found that radial artery grafts worked better when grafted to more thoroughly diseased vessels. Specifically, the researchers separated the target vessels into three groups: those with 70-89 percent narrowing, 90-99 percent narrowing, and 100 percent narrowing. They found a much lower failure rate (approximately 50 percent) for radial artery grafts that were grafted to vessels with 90 percent narrowing or more.
“The implications from our one-year study were confirmed in the five-year results – radial artery bypass grafts should be used preferentially for the most severely narrowed coronary arteries,” Fremes said.
Fremes noted that because each study patient received both graft types, the researchers were unable to associate clinical outcomes with a specific grafting strategy. He added that late findings from an Australian study and a study conducted by the Veterans Affairs Cooperative Studies program will provide both angiographic and clinical outcomes.
The study was funded by the Canadian Institutes of Health Research. Fremes had no financial disclosures related to the study.
For more information: www.cardiosource.org


 February 06, 2026
February 06, 2026