March 22, 2012 – Addressing concerns over radiation from cardiac imaging and procedures, the American College of Cardiology Foundation (ACCF), Duke University Clinical Research Institute (DCRI) and American Heart Association (AHA) released recommendations to enhance radiation safety.
Diagnostic imaging tests and procedures that use radiation play an important role in the effective treatment of heart disease. While there is no evidence that exposure to low levels of radiation in the course of treatment causes harm, concerns about patient safety remain.
“The use of radiation is essential to high-quality cardiovascular care,” said Pamela S. Douglas, M.D., professor of medicine at Duke University Medical School and chair of the writing committee. “Without it, we wouldn’t be able to do all the things we can now do to diagnose and treat patients, so we need to minimize patient exposure while preserving our ability to take care of this very common disease.”
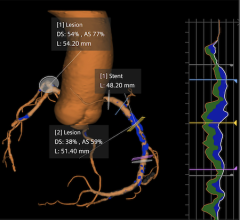
Radiation exposure for medical purposes has increased about six-fold over the past 25 years, with radiation from cardiovascular imaging and interventions accounting for about 17 percent of the total. Imaging tests with radiation allow healthcare professionals to see detailed pictures of the heart to identify problems. This technology is also commonly used when patients have chest pains and in treating arrhythmias (an irregular heartbeat), and can provide real-time guidance to cardiologists during angioplasty (when implanting stents to open blocked or narrowed coronary arteries), among other applications.
The new report – a culmination of the first multidisciplinary think tank on the topic – provides a roadmap to improve radiation safety, reduce patient dose, and obtain quality images for diagnosis and treatment based on available appropriate use criteria and best practices. A broad array of stakeholders were represented including medical physicists, experts in cardiovascular imaging, safety specialists, government agencies, patients, and industry representatives who are responsible for making better equipment.
“This effort represents a major step forward to better define the issues and needs around patient radiation safety in cardiovascular imaging, and to develop an action plan to guide future efforts,” said Douglas.
Ionizing radiation has been in use for medical purposes since 1895 and recent technological advances have increased its use in cardiology. Still, Douglas says there are gaps in many physicians’ understanding of how radiation is actually measured and what is known and unknown about the potential harm it might cause patients down the line. As such, experts say it is critical to better understand how radiation is being used and to allay concerns about exposure. A key challenge discussed by the group is that the absorbed dose – which is less than that delivered by the machine – varies tremendously from person to person, by the organ or tissue scanned, the machine design and a host of other factors.
“We need to better understand the difference between the radiation delivered (exposure) and the dose received, and try to reduce the variability across patients and across laboratories,” Douglas said. “The reality is that radiation exposure is a fact of life. We are exposed to background radiation from natural sources each and every day, and there is no evidence at this time that the low level of radiation used in most health care encounters causes any problems.”
However, she says the think tank has called for long-term tracking of those individuals most at risk, as well as the implementation of quality improvement initiatives designed to help laboratories track and improve their radiation safety.
Among the recommendations set forth include the need for:
• Collaboration across a large number of diverse stakeholders
• Education of healthcare providers ordering and providing medical tests and procedures using radiation, including creating a culture of safety to ensure clinicians are aware of strategies that can minimize radiation exposure
• Clarification of the relationship between low-dose radiation exposure associated with cardiovascular imaging and therapeutic procedures and potential health problems or malignancies down the line
• Careful patient selection and avoidance of inappropriate testing and procedures by using ACC’s appropriate use criteria and balancing the benefits of cardiovascular testing and procedures against minimizing dose, including adherence to the long-standing principle of ALARA—as low as reasonably allowed.
In addition to ACCF, DCRI and AHA, other participating societies included the American College of Radiology, American Society of Nuclear Cardiology, Heart Rhythm Society, Society for Cardiovascular Angiography and Interventions, Society of Cardiovascular Computed Tomography, and Society of Nuclear Medicine.
The full report, “Developing an Action Plan for Patient Radiation Safety in Adult Cardiovascular Medicine,” will be published in the May 15, 2012, issue of the Journal of the American College of Cardiology and an upcoming issue of Circulation: Journal of the American Heart Association. It will also be accessible at www.cardiosource.org.

 February 02, 2026
February 02, 2026