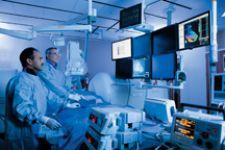
Dr. Eric Prystowsky, right, pictured with Dr. Benzy Padanilum, is among the country's EP specialists seeking new ways to treat AFib and other cardiac arrhythmias.
When it comes to treating patients suffering from heart failure, which is typically defined as a heart whose pumping power is weaker than normal, physicians are facing a paradox.
Although an increasing number of people are making healthier lifestyle choices like lowering their cholesterol levels and stopping smoking, there appears to be a higher incidence of heart failure among the general population, says David Burkhardt, M.D., associate program director for the Electrophysiology and Pacing Fellowship Program and a staff member of the Electrophysiology and Pacing Section in the Department of Cardiovascular Medicine at the Cleveland Clinic in Cleveland, OH.
"Overall, heart failure rates are increasing due to an aging population and longevity," he explained.
Dr. Burkhardt's observations are supported by the American Heart Association, which has reported that approximately two percent of the population has heart failure and that 75 to 80 percent of these patients are over 65 years of age. In addition, congestive heart failure (CHF) is responsible for over 260,000 deaths annually, while approximately 550,000 new cases are diagnosed each year.
Of course the ultimate cure for patients with end-stage heart failure is to receive a new heart. But that is seldom the case, says Margarita Camacho, M.D., surgical director of the Cardiac Transplant and Mechanical Assist Device Program at the Saint Barnabas Heart Center at Newark Beth Israel Medical Center in Newark, NJ.
"We can only do 2,100 transplants a year nationwide," she said. "However, the number of people who could benefit are between 75,000 and 100,000."
Compounding the problem is the fact that the cut-off age for most heart transplants is 65, Dr. Camacho notes.
As a viable alternative to transplants, a growing number of physicians are recommending the implantation of a mechanical pump, such as a ventricular assist device (VAD). Still mainly used as a "bridge-to-transplant" interim therapy, the newer VADs are much smaller and more efficient and are quickly becoming a preferred type of "destination therapy" for those with end-stage heart failure who are ineligible for a transplant, Dr. Camacho says.
But while VADs are gaining in popularity, drug therapy is still the first line of defense, says Dr. Burkhardt. Topping his list are beta-blockers, ACE (angiotensin converting enzyme) inhibitors and digoxin, as well as diuretics to reduce swelling and volume overload, he says.
As for the implanting of standard single chamber or dual chamber pacemakers, Dr. Burkhardt says this is reserved for those with reduced ejection fractions that have dropped to 30 percent or less.
Likewise, using the biventricular pacemaker, also known as cardiac resynchronization therapy (CRT), has been found to be successful in treating patients with desynchronous contractions of the left and right ventricles. These pacemakers have a response rate of 70 percent, he notes.
But advances in pacemaker technology are making them smaller and more efficient, Dr. Burkhardt says. Improved timing optimization may very well raise response rates to 90 percent, he says. And results also look promising among groups of patients whose pacemakers add an extra impulse immediately after the heart has contracted.
Another technological breakthrough is the use of invasive monitoring techniques. According to Dr. Burkhardt, a sensor that can be incorporated directly into the pacemaker can detect pressure variations in the left atrium which can signal a worsening heart function, resulting in an automatic activation of the pacemaker.
Treating arrhythmias
Without a doubt, the most common form of arrhythmia is atrial fibrillation (AFib), which is found in about 2.2 million Americans and about 4.5 million Europeans. Yet choosing the right therapy often depends on how life-threatening this condition is in a patient.
Eric Prystowsky, M.D., consulting professor of Medicine, Duke University Medical Center, Durham, NC, and director of the Clinical Electrophysiology Laboratory at St. Vincent Hospital in Indianapolis, IN, says that AFib is not life-threatening in itself, but its consequences, including stroke and congestive heart failure, can be fatal.
And there is a definite link between heart failure and arrhythmias, says Michael Orlov, M.D., director of Cardiac Arrhythmia Research at Caritas St. Elizabeth's Medical Center in Boston.
"Patients with heart failure usually have arrhythmias," he said, adding that in most cases the arrhythmias compound the severity of the heart failure.
To avoid sudden death or to treat patients who present with either ventricular tachycardia or ventricular fibrillation, an implanted cardiac defibrillator (ICD) is commonly used.
"Their use is showing more promise," said Dr. Orlov, who adds that they can even be implanted in high-risk patients in a "proactive, preventative approach."
Acknowledging that the industry has had some setbacks due to faulty circuitry and failing batteries in some models, Dr. Orlov does not see the use of ICDs diminishing. In fact, he says their use is on the rise.
Also on the rise is the debate, as to whether drug therapy is still as effective as newer, more invasive therapies.
In treating AFib patients, Dr. Prystowsky says he will first try to control the irregular heart beat with drugs. But in explaining the difference between controlling AFib and finding a potential cure, he readily admits that "drugs don't 'cure' anything."
Dr. Orlov agrees. "Medications are limited in what they can do," he stated.
Yet new drugs are being developed. Among the most promising is Tikosyn (Dofetilide), which is being used to convert atrial fibrillation to a normal sinus rhythm. Clinical trials showed Tikosyn to be effective in about 70 to 80 percent of cases with maintenance of sinus rhythm at one year ranging from 46 to 80 percent. However, the risk of creating even more arrhythmias if the drug's dosage is changed has limited its use to only a few major hospitals in the U.S.
In finding a safe and effective therapy, Dr. Prystowsky said, "Catheter ablation is the treatment of choice because it cures you for life."
Whether or not catheter ablation qualifies as a true cure, Dr. Prystowsky insists that his success rate is over 95 percent.
By using a catheter to deliver energy to the area of the heart muscle where the abnormal heart rhythm originates, the electrical pathway is, in essence, disconnected. The therapy has proven successful in treating AV Nodal Reentrant Tachycardia (AVNRT); atrial fibrillation and atrial flutter; and ventricular tachycardia.
Dr. Prystowsky is certainly not alone in heralding the successes of catheter ablation.
Jeremy Ruskin, M.D., director of Cardiac Arrhythmia Service at Massachusetts General Hospital in Boston, said, "We do an average of three a day. Catheter ablation has become the most common treatment outside of drugs."
Because AFib is generally considered an age-related arrhythmia often seen in hypertensive patients, Dr. Ruskin says most of the patients he treats are over 60 years of age. So while medications will keep the irregular heartbeats under control, a catheter ablation is a good option for older individuals because it is a minimally invasive procedure, he says.
Expanded options
When treating AFib surgically, the list of accepted procedures is growing.
One method now gaining more support among surgeons is pulmonary vein antrum isolation (PVAI), also called pulmonary vein ablation.
By inserting a soft-wire catheter into the blood vessels of the atrium, energy can be delivered to the area of the atria that connects to the pulmonary vein (ostia). The ablation produces a circular scar that blocks any impulses from firing within the pulmonary vein. This procedure also has been performed in other parts of the heart such as the superior vena cava.
Pulmonary vein isolation has shown a success rate of 80 to 85 percent with the first ablation, and up to 95 percent in patients who have had an additional ablation.
Another procedure that shows promise is a modified Cox-Maze procedure that focuses on isolating the pulmonary veins and portions of only the left atrium.
The standard Cox-Maze procedure involves making incisions in both the right and left atria in order to interrupt the pathway of abnormal impulses, while directing normal sinus impulses to the atrioventricular (AV) node. The success rate of this procedure has been about 95 percent.
While the success of any ablation depends on the use of energy to disrupt the abnormal electrical impulses of the heart muscle, expanding the range of energy sources that can be used is giving surgeons even more options.
Among those that Dr. Ruskin sees as promising are:
- Radiofrequency ablation, which uses radiofrequency energy to heat the tissue and produce lesions on the heart. This procedure has shown to have a success rate of 80 percent.
- Cryothermy, also called cryoablation, uses extremely cold temperatures transferred through a probe called a cryoprobe that creates lesions. This procedure also has an 80 percent success rate.
- Microwave radiation, which uses a special catheter to direct microwave radiation to areas of the heart, thus producing the desired lesions. Studies have shown that this form of ablation creates more precise lesions with less charring of the surrounding area. The success rate of this procedure also has been about 80 percent.
New stroke protection
A major problem for most AFib patients is the possibility that they may suffer a stroke caused by blood clots forming in the left atrial appendage, says Dr. Ruskin. But a new implantable device may not only keep clots from entering the bloodstream, but may also "provide a replacement for Coumadin in patients who have bleeding disorders," Dr. Ruskin stated.
For close to six months, Dr. Ruskin and his staff at Massachusetts General have been involved in one of a number of clinical trials to test the efficacy of the Watchman device. More than 40 hospitals in the U.S. are involved in these clinical trials.
Developed by Plymouth, MN-based Atritech Inc., the Watchman is an "umbrella-shaped device that, when it expands, allows the left atrial appendage to clot off," Dr. Ruskin explained.
Permanently implanted behind or right at the opening of the left atrial appendage, the Watchman is placed in the heart by using a catheter inserted through a vein in the patient's upper leg.
The implantation of the device has been easy and encouraging," Dr. Ruskin noted.
While surgical procedures that use a catheter have a proven track record, finding an exact spot in the heart can be a challenge, says Dr. Orlov.
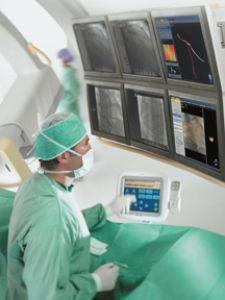
To help clinicians better treat arrhythmias surgically, Philips Medical Systems announced in February the commercial release of Philips EP Navigator, an imaging tool that combines pre-interventional 3-D CT images with live X-ray fluoroscopy in a single image.
Caritas St. Elizabeth's Medical Center has been a beta test site for EP Navigator since the fall of 2006 and Dr. Orlov was the first clinical user of the product.
"We've probably operated on 10 patients using this system," he said. "It's definitely helped mentally, but to determine its long-term efficacy we will need more patients."
Dr. Orlov explains that two separate images are commonly used when doing an ablation procedure: A three-dimensional CT scan taken prior to surgery forms the baseline image, while fluoroscopy during surgery provides the live, real-time image. But this image is essentially a "two-dimensional shadow," he says. By overlaying the remote CT scan onto the fluoroscopic picture, the entire image comes alive — making it easier to visualize catheter position and to maintain good contact between the ablation catheter and the left atrial wall.


 January 28, 2026
January 28, 2026