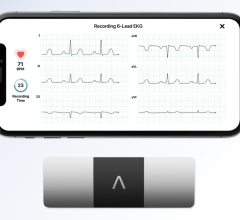
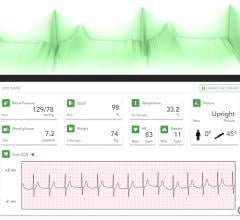
Data from thousands of patients monitored by Boston Scientifics LATITUDE Patient Management system is being compiled for further study in Bostons ALTITUDE initiative.
With the healthcare industry striving for greater efficiency at virtually every level, it shouldn’t be a surprise that hospitals and clinics are increasingly turning to manage patients with implantable cardiac devices remotely, including implantable cardioverter-defibrillators (ICDs), cardiac resynchronization therapy-defibrillators (CRT-Ds) and pacemakers. Remote monitoring for patients with these devices has ramped up over the past few years, according to clinicians, with big advances in sophistication.
As a sign of recent validation of remote monitoring, the Centers for Medicare and Medicaid (CMS) implemented changed in reimbursement for remote monitoring in January 2009, including using new codes that supplement those for remote monitoring of pacemakers and ICDs, adding reimbursement codes for remote monitoring of insertable loop recorders (ILRs) and ICMs and have adjusted billing guidelines for all cardiac devices to be on par with reimbursement for an in-office visit.
Efficiency — the name of the game
Patient monitoring is designed to reduce in-office follow up visits or even telephone checkups with patients in some cases.
One remote monitoring system is Medtronic’s CareLink Network, an Internet-based system designed to help manage the monitoring of implantable device therapy, such as pacemakers, ICDs, CRT-Ds and implantable cardiac monitors. The CareLink is made so patients can send data from their CareLink Monitor from a small piece of equipment in the patient’s home that is plugged into a standard phone jack. For most of Medtronic’s line of CRT-Ds and ICDs, the Carelink Network features Conexus Wireless Telemetry with SmartRadio, which allows for remote and automatic transmission of device data to physicians at preset dates and time, or if the system detects a notable change in the patient’s condition, according to Medtronic.
“The information we’ve been able to get now is the full interrogation of how the leads are working, the electrical parameters, etc.” said George Crossley, M.D. clinical cardiac electrophysiologist, president of Mid-State Cardiology, a unit of St. Thomas Heart in Nashville, TN. “The devices also store a lot of historical information about how much atrial fibrillation they’ve had, how much heart failure they’ve had. For the last few years, we’ve been able to get that on an irregular basis where we’ve given the patient a date to transmit their data manually. It’s much more efficient for the doctor and patient.”
Dr. Crossley notes that the new Conexus Wireless Telemetry system is useful in detecting episodes like atrial fibrillation within a day or two, which helps clinicians better manage the disease.
According to studies gathered in 2004 by Human Factors International on behalf of Medtronic, the CareLink Network was found to increase efficiency in remote follow-ups for ICD and CRT-Ds versus in-office visits. The study measured follow-up times at clinics that had a large number of both Medtronic CareLink Network patients and in-office device patients. According to the studies, CareLink remote follow-ups took 7.8 minutes versus 22.2 minutes for in-office visits, an efficiency increase of 65 percent. In breaking down the numbers, CareLink remote follow-ups increase efficiency for patients without episodes by 77 percent, while increasing efficiency by 44 percent for patients with episodes.
Another area of efficiency is when a patient has an episode and gets a shock. In the past, that patient would have had go to their local ER, get admitted and wait to see their electrical heart rhythm specialist, said Dr. Crossley. With CareLink, a patient can just send a transmission of their data after receiving a shock so the clinician can evaluate.
“We talk to the patient over the telephone after seeing the data,” Dr. Crossley said. “If the patient is feeling well, the defibrillator worked and they’re back at normal rhythm, they stay home. They spend $80 on the whole episode rather than a few thousand on a trip to the hospital.”
Another patient monitoring system is Boston Scientific’s LATITUDE Patient Management system, designed to offer remote monitoring for patients with ICDs and CRT-Ds. LATITUDE monitors the patient’s ICD or CRT-D by gathering information through the use of the LATITUDE Communicator, a small piece of equipment that sits in the patient’s home and connects to a standard phone jack. The LATITUDE Communicator is made to check device battery status, lead status and device settings, as well as notify the doctor if certain conditions are detected. The wireless LATITUDE Communicator uses Active Monitoring to automatically collect data from the implanted device, at a schedule determined by the implanting doctor. The “wanded” Communicator features a wand that patients use to check the device when promoted by the system. Patients are alerted by a flashing light on the Communicator to use the wand to check their device. (The type of LATITUDE Communicator used depends of the type of implanted device, said the company.)
“What I like about LATITUDE is that you get data and you get reliable data,” said John Boehmer, M.D., professor of medicine and surgery, The Penn Sate College of Medicine. “[Sometimes patients] either didn’t weight themselves or didn’t bring in the weights. You’re really not sure how often they are weighting themselves. The unique aspect of remote monitoring is that you have validated, time-stamped weights that are automatically uploaded, and you have access to them.”
The efficiency gains are obvious, according to Dr. Boehmer. He said that scheduling telephone follow-ups with patients can be effective, except that there is only about “a 75 percent hit rate” on actually reaching the patient as the scheduled time. With remote monitoring, it is easier to obtain the basic information from the patient.
“We have a disease management coordinator who is able to oversee the data coming in and she’s grateful for [remote monitoring] because she now uses a different protocol for patients who have automated follow up,” Dr. Boehmer said. “She doesn’t call them as routinely.
“My estimate, and what others have said anecdotally, is that [the system] roughly cuts your work load in half or doubles your capacity, which ever way you want to look at it,” he said. “Generally, the disease management coordinator can handle 100 patients. That’s the benchmark I’ve picked up from a number of places. That’s not based on a lot of hard data, so there is more work to be done to see if those quantifications are accurate. But, anecdotally it seems to be case in our program.”
Detecting conditions
While efficiency may be the primary benefit to patient monitoring systems, clinicians are also quick to point out the clinical benefits. One example of a clinical benefit, supplied by Boston Scientific in a case study, illustrates how quickly a condition may be detected and, ultimately, treated. A Kansas patient (50-year-old male) with a Guidant CONTAK RENEWAL 3 RT CRT-D and a history of AF was enrolled in the LATITUDE Patient Monitoring and Active Monitoring system. Within several days after an AF episode, the patient would typically notice symptoms of clinical decompensation. The LATITUDE Active Monitoring program was programmed to alert David Mongolis, M.D., FACC, medical director, arrhythmia services, Via Christi Regional Medical Center in Wichita, KS, if the patient experienced an atrial tachycardia response episode, or a mode switch, for more than 24 hours. Dr. Mongolis was alerted via fax from LATITUDE that the patient had an episode of silent AF. The patient was called to the physician’s office, where a cardioversion procedure was performed to restore the heart to a normal sinus.
According to the case study, Dr. Mongolis said, “By the ability to quickly recognize his episode of atrial fibrillation, we were able to see the patient in the office, cardovert his artrial fibrillation through a commanded shock and the patient did not need to be hospitalized. With this patient, LATIDUE Active Monitoring gave me an early opportunity to identify an event previously associated with decompensation and intervene before the patient became symptomatic.”
The future of remote monitoring
Looking to the future, clinicians seem to be excited about potential new features and data accumulated, which will help better manage patients.
“What we see in the future is getting better sensors for heart failure,” said Dr. Boehmer. “What that sensor is going be is up for some debate, but the one that seems to have the most traction right now would be intracardiac or pulmonary artery pressures of some sort, such as left atrial pressure, right ventricular pressure, pulmonary artery pressure; one of those that gives a reflection of congestion.”
Dr. Crossley hopes to see the FDA approve the Medtronic OptiVol Alert, which is designed to notify clinicians if patients are experiencing congestive heart failure. The alert measures the amount of fluid in a patient’s chest cavity and alerts clinicians if the fluid gets to a certain level. The system is approval in Europe and is currently undergoing clinical trials in the U.S., said Dr. Crossley.
In May 2008, Boston Scientific announced its new clinical science initiative, ALTITUDE, which was created to analyze data from the LATITUDE system to seek answers to common questions related to ICDs and CRT-Ds. According to the company, the ALTITUDE initiative will be managed in collaboration with a physician panel who will assist in identifying clinical issues for further examination.
“We have an opportunity to do investigations on tens of thousands of patients over a long period of time, looking at interactions between heart failure and rhythm and things like autonomic function, heart rate variability and risk of ventricular arrhythmias,” Dr. Boehmer said. “Although we might lack in the level of detail that you’d get in a clinical trial, some of it can be overcome by the sheer numbers. When you have data on tens of thousands of patients, you can get a lot of detail. This is a de-identified database where we can learn a lot.”



 September 16, 2025
September 16, 2025