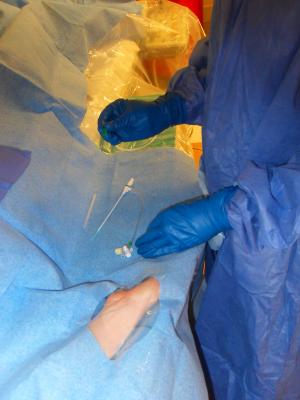
Millions of percutaneous coronary interventions (PCIs) are performed each year around the world to treat obstructive coronary artery disease. In order to access the arteries, interventional cardiologists traditionally use the femoral artery, which is still the most common access route for PCI in the United States. However, access via the radial artery is increasingly common. The transradial approach for PCI was developed 23 years ago and is used in more than 50 percent of procedures in most European countries. In fact, last year, the European Society of Cardiologists (ESC) bestowed its highest level of recommendation for the transradial approach over the transfemoral approach for PCI in patients with acute coronary syndrome.
In the United States, adoption of transradial access for PCI has been slower than in other parts of the world, but continues to grow. In 2013, the rate of PCIs performed transradially was estimated at 16 percent of all U.S. PCI procedures; more recently though, reports put estimates closer to 30 percent.
Multiple studies over the past 20 years have shown that transradial access for PCI may have a distinct advantage over the transfemoral approach in eliminating access site bleeding complications. It does, however, raise serious issues regarding operator exposure to ionizing radiation during transradial PCI and the significant health hazards associated with exposure.
As an interventional cardiologist in a busy urban tertiary care center – Detroit Medical Center (DMC) – I treat a very high number of patients each year and adopted the transradial approach years ago. While prioritizing care of my patients over my own well-being, I continue to have significant concerns about the health risks linked to chronic exposure to low-level ionizing radiation. Mounting evidence shows a link between fluoroscopy exposure among physicians and staff in the cath lab and serious health issues such as cancer, cataracts, and orthopedic injury from personal protective equipment (PPE).
Thankfully, DMC is proud to take radiation safety seriously and has made radiation exposure a key area of focus as a result of the high volume of procedures we perform. The hospital has dedicated significant time and resources to reducing radiation exposure to both its patients and its staff and has made several technology investments to achieve a safer cath lab environment.
Robotics to Help Lower Operator Dose
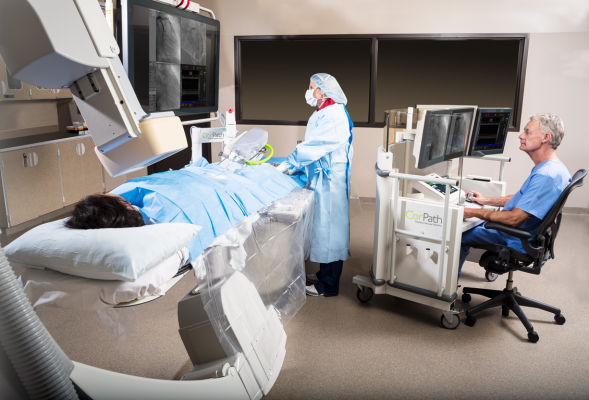
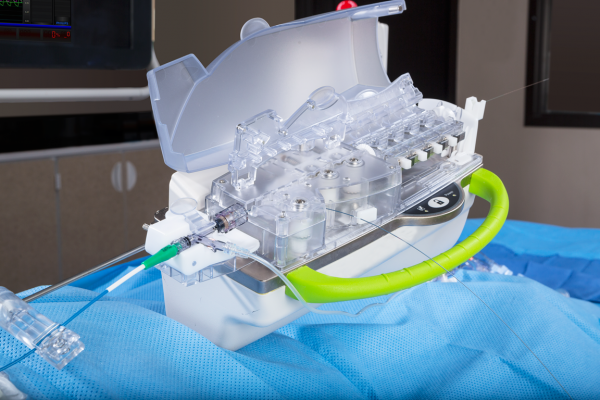
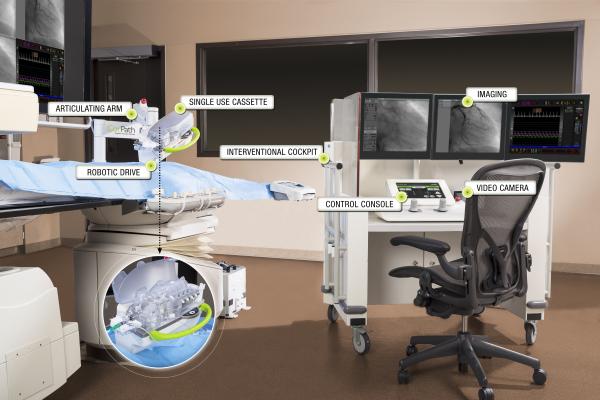
One investment at DMC was in the CorPath Vascular Robotic System from Corindus Vascular Robotics. I began performing robotic-assisted radial access PCIs with the CorPath System and have found that it is an ideal option for both patients and operators. While transradial access has been shown to have patient benefits, it increases radiation exposure to the operator. However, when transradial access PCI is performed with robotic assistance, we can dramatically reduce operator radiation exposure, utilizing the protection of a radiation-shielded interventional cockpit outside of the X-ray field. Precision and accuracy may also be improved with robotics, as robotic-assisted PCI allows for accurate measurement of relevant anatomy and enables balloon/stent positioning with movements as fine as 1 millimeter. Thus, robotic precision has the potential to benefit the patient.
At DMC, robotic-assisted radial PCI also is used in our fellowship program. In fact, I am proud to have led the development of the first formal structure for a robotic fellowship program at DMC. Thanks to the opportunity to perform a high volume of cases, and access to advanced treatment techniques and advanced technologies, the interventional cardiology fellowship program at DMC continues to attract talented and dedicated physicians. Key highlights of the DMC fellows program include:
• A high volume of PCI cases and exposure to multiple modalities to treat a wide range of clinical scenarios, offering exposure to and experience with a multitude and variety of diseases, as well as many complex and high-risk PCIs; and
• DMC trains more female fellows than any other program in the country. In a field that is approximately 95 percent male, females are severely under-represented. However, two DMC physicians are hoping to change these statistics — Cindy Grines, M.D., and Theodore Schreiber, M.D. Aside from being a well-published and highly-respected interventionalist, Grines is an advocate for women in the field. Schreiber, nationally recognized for performing high-risk PCIs, is also committed to bringing more women into interventional cardiology.
As the DMC fellowship program evolves, we expect to see an increase in the number of operators using the CorPath System to perform radial-access PCI.
As part of the process for implementing a robotic-assisted PCI program in DMC’s cath lab, Corindus, developer of the CorPath System used in DMC’s cath lab, conducted a focused training session with DMC fellows and staff. Training was centered on increasing efficiency with the robot to decrease procedure times. Both operators and staff working with the CorPath System were trained. For the fellows, the team from Corindus spent time with each fellow outside the lab to help them develop the necessary proficiency. Subsequently, this has become the model for fellows training programs at other sites as well. Working with fellows outside the pressures of an ongoing procedure can lend additional focus on the skills required for successful robotic cases.
In addition to fellow and staff training, DMC conducts training for physicians from outside the facility to advance their skills and demonstrate novel technology. Observing a robotic-assisted PCI is always a highlight of these visits. These visits allow the team at DMC to show other physicians how we integrate a variety of technologies and techniques into our treatment plan, which, as an academic center, is very important to our overall mission.
The Fututure of Robotics in the Cath Lab
As I look ahead to the continued evolution of PCI, the natural question is “What is the future of that cath lab?” I see the opportunity for dramatic changes over the course of my career. I see the potential for robotics to expand and enable virtual assistance and remote operation in a PCI setting, where a physician who is located in an urban environment can perform cases in a rural area, remotely, akin to tele-intervention.
The benefits of robotic-assisted radial PCIs represent a meaningful advance for both operator and patient safety, and I will continue to work towards highlighting and demonstrating the benefits of this approach to increase its adoption in the United States.


 July 31, 2024
July 31, 2024