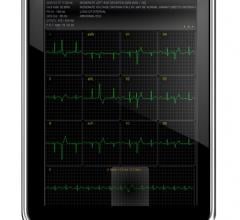
The latest Horizon Cardiology version 12.1 from McKesson integrates barcode inventory management. Supplies used in the cath lab are scanned during the procedure and immediately recorded for inventory and billing purposes.
In today’s market, many vendors have very good cardiovascular picture archiving and communications systems (PACS). One needs to only hit the exhibit floor for a short time at the Radiological Society of North America (RSNA) or the American College of Cardiology (ACC) before it becomes apparent that there is a myriad of systems available right now that are excellent and fairly user friendly. They are capable of storing and retrieving high-quality images in just seconds.
So how does one choose if all of the PACS give crisp clean images that are easily retrievable? Start by asking yourself the following questions: Can the PACS system readily tie into your centralized patient information system? How easy is this connectivity? Can information flow forward and backwards? In other words, at the completion of a study, can all of the information be readily “dumped” into your central patient server? When initializing a study can information be downloaded from your central patient server to the PACS to avoid duplication (such as patient demographics)? These issues are of paramount importance when choosing a CV PACS.
A PACS should allow you to see your images with excellent clarity, allow you to manipulate the image and do quantitative analyses without having to read a 400-page user manual. You may also want to be able to pull up old studies at a moment’s notice with no lag time, and add the ability to store and retrieve and manipulate digital subtraction images for your peripheral vascular studies in an ideal system, However, there are deeper issues to consider, such as connectivity, the ability to mine data and using technology to increase efficiency.
PACS Need to be Interoperable
While many major vendors have image storage and retrieval systems, they have a very closed architecture that makes it difficult, if not impossible, to “talk” to other information units in a hospital. This lack of interoperability may include systems in the cardiac catheterization lab itself. This offers a financial advantage for a given vendor, as it forces hospitals to purchase all of its individual components to insure the best connectivity.
However, it is unusual for a given vendor to have the “best” of everything. Clinicians prefer different vendor systems because the image quality of one cath lab is preferred over another. Some hemodynamic monitoring systems are also more intuitive for technologists and nurses to run. It is important to have a PACS that integrates with the clinicians’ preferred devices.
Auto Report-Generation Saves Time
It is also important the system has automated report-generation. In the current era, there is little reason to not be able to complete a study and have the report 80-90 percent completed and waiting. A physician should only need to spend an extra three to five minutes to finalize things. Dictation is so 1960’s. The ability for information to automatically transfer from the image acquisition system and the hemodynamic monitor to the PACS system is crucial. This also allows for automatic population of a nearly completed report. Remember saving time is a critically important feature to the interventional cardiologist.
The flow of data is not simply one-way into the PACS, there needs to be two-way communication. Data acquired in the cath lab must be sent to a central hospital information system, and IT communication is key for any system under consideration. This transfer of information might come in several forms, such as a finalized cath report.
Data-Mining Is Needed
The ability to easily program the PACS to pluck out data elements of interest that are subsequently collected and sent it to another repository is also quite helpful. It might be useful to know how many cases were successful vs. those that were unsuccessful; how many drug-eluting eluting stents were placed vs. bare-metal stents; or how many complications occurred and what was the precise nature of said complications. This information is requested on a regular basis by national data registries and quality assurance organizations. Furthermore, third-party payers are now demanding to know this information regularly. Reimbursement (both physician and hospital) is often tied to providing this information in a timely fashion. A hospital may have two, three, four or more full-time employees laboriously combing through charts to get this information. Alternatively, pre-specifying what data elements are sent automatically to a report from a PACS is worth its weight in gold.
At the conclusion of any given case, an optimal PACS has the ability to provide the operator with a report that is 90 percent complete and provide the operator with images that are easy to review and can be ultimately kept in storage. The system should also provide data elements that go to a central repository for later distribution to a quality assurance committee, national data bank registry, or any third-party payer as deemed appropriate by the hospital.
Open-Architecture
Obviously, inherent in this discussion is my belief that any PACS worth investigating is one that offers an open architecture. In other words it must be vendor-neutral. It must be able to easily communicate with whatever systems are either present in the cath lab, or are to be brought into the cath lab at a later date. It must be able to communicate with the overall hospital information system as well. This allows you to have a system as described above. The technology is moving and evolving in a fast and furious manner. My advice is to do your homework on any system and do not to rush into purchasing a system. This will pay off in the end.
Editor’s Note: Dr. Breall serves on the Editorial Advisory Board of Diagnostic and Invasive Cardiology. He is a professor of clinical medicine, director of the cardiac catheterization laboratories and head of interventional cardiology for Indiana University, Krannert Institute of Cardiology. He is also medical director of the cardiac catheterization laboratories for Clarian Health Partners in Indianapolis. He recently researched and purchased a cardio PACS for one of his facilities.

 March 06, 2024
March 06, 2024