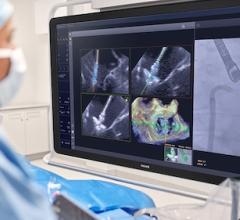
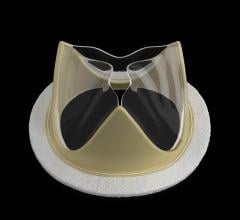
JenaValve Uses a self-expanding nitinol stent with a pericardium valve. The device can be repositioned.
Aortic stenosis (AS) is one of the most common valvular disorders in older adults, with a prevalence of approximately 8 percent at age 85 (1). Symptomatic patients managed medically have a poor prognosis (2), and the hope of durable benefit with balloon aortic valvuloplasty (BAV) has not been realized (3,4).The Society of Thoracic Surgeons (STS) database shows that the operative mortality for isolated aortic valve replacement (AVR) has continued to decline to approximately 2.5 percent in 2006, while the percentage of patients older than 75 years has increased to 37 percent (5).
However, many patients are denied AVR due to advanced age and multiple comorbidities. A prospective, multicenter European survey suggested that only 47 percent of patients with severe aortic stenosis underwent AVR (6). Likewise, approximately half of patients with severe aortic stenosis underwent AVR confirming similar findings in North America (7).
The development of catheter-based techniques may provide an alternative method for treating AS in patients with unacceptably high estimated surgical risk. Transcatheter aortic valve implantation (TAVI, also known as transcatheter aortic valve replacement, or TAVR) was first reported in animals by Anderson (8) and Pavnik in 1992 (9). Cribier performed the first TAVI in humans using an antegrade femoral venous procedure with transeptal access to the aortic valve (10-12).
The Development of Transcatheter Valves
As of this writing, there are at least six transcatheter valve devices in development (13). The Sapien valve (Edwards Lifesciences Inc.) and the CoreValve (Medtronic) have the most worldwide experience. Early trial experience with CoreValve included 646 patients and Sapien trials included 785 patients. Both valves have received a Conformité Européenne (CE) mark approval in Europe and are available for commercial use. The feasibility trial for the Sapien valve has been completed in the United States and the pivotal trial (PARTNER) is currently being conducted in multiple centers in the United States, Canada and Europe. The U.S. pivotal trial for the CoreValve was approved in October by the U.S. Food and Drug Administration (FDA).
Hybrid Operating Room and Imaging Systems Required for TAVR
Joint recommendations of the European Society of Cardiology and the European Society of Cardiac Surgery consider the hybrid operating room (OR) the optimal environment for these new procedures (14). A multidisciplinary team including surgeons, interventional cardiologists, anesthesiologists and echocardiographers must work in tandem for a successful TAVI program. The hybrid OR should combine the diagnostic capabilities of the cardiac catheterization laboratory with the surgical capabilities of a full operating room to allow for both catheter-based and open-surgical approaches.
Advanced angiography imaging systems enable the operator to accurately position and deploy the transcatheter valve. Locating the C-arm at exactly perpendicular to the plane of the aortic annulus is essential to reliable valve positioning. Two imaging systems may aid in the rapid positioning of the C-arm while minimizing contrast administration.
The first is the Syngo DynaCT (Siemens Healthcare). Advanced angiographic C-arms with 2-D and CT-like 3-D imaging can detect and mark relevant landmarks, including the coronary ostia and the “perpendicularity ring” of the aortic annulus. The image can be rotated to achieve an optimal perpendicular projection with the C-arm. Moreover, the acquired image can be overlaid onto live fluoroscopy for further device guidance.
The second system is the C-THV (Paieon). This software system uses two angiographic projections to generate a “perpendicularity graph” along which the C-arm can be positioned to achieve unlimited orthogonal angles to the plane of the annulus. This system also helps with navigation and real-time positioning by using two spot markers
on screen (15).
Implantation Approach for TAVI Valves
Although the first case of TAVI in humans was described using the antegrade transseptal approach (10), the procedural complexity and associated risks (such as the development of acute mitral regurgitation) have limited adoption of this technique (11,16). Hanzel and colleagues described the first human case using the retrograde transfemoral arterial approach after a failed transseptal approach (17). Currently, the two most common approaches for TAVI are the retrograde transfemoral arterial approach and the antegrade transapical approach via the left ventricular apex. Other approaches include the retrograde transaxillary arterial (18) and retrograde transaortic approaches.
Other Indications for TAVI, Including Valve-in-Valve
Preliminary reports demonstrated feasibility of transcatheter placement of a prosthetic valve within a degenerated bioprosthetic valve (valve-in-valve) (19). The CoreValve was used to treat a stenotic 21 mm aortic bioprosthesis with initial success. Another report shows the feasibility of using the Sapien valve for CoreValve failure (20). Other attractive applications of this device include primary aortic regurgitation and failed xenograft or homograft roots, although no reports have been published
to date.
Access Closure Devices in TAVR Procedures
True percutaneous access for TAVI already exists for the transfemoral approach based on technology previously used with aortic endografting. These devices have the potential of reducing time to hemostasis, facilitating early patient mobilization and reducing hospital length of stay (21). Several studies have reported the off-label application of a preclose technique to achieve hemostasis following percutaneous procedures using sheaths up to 24 French (22, 23). Femoral access closure using two Perclose Proglide devices (Abbott Vascular) in TAVI has been described by Sharp et al (24). Alternatively, the Prostar XL device (Abbott Vascular) is FDA-approved for arteriotomy closure up to 10 French sheath size, but can also be used in an off-label fashion for large-bore access.
Results of TAVI Procedures in Trials Has Been Positive
Procedural outcomes of the Sapien valve and CoreValve from several multicenter trials and post-market registries are shown in Table 1. Initial results from the U.S. PARTNER pivotal trial using the Sapien valve were recently reported at Transcatheter Cardiovascular Therapeutics (TCT) 2010 in September for the inoperable cohort of patients (25). The trial is the only randomized clinical study to date and enrolled patients in 21 centers. Cohort B included 358 patients who were not considered to be suitable candidates for AVR and were randomized to TAVI or medical therapy (including balloon aortic valvuloplasty).
At one year, mortality in the TAVI group was significantly lower than the medical group (30.7 percent versus 50.7 percent, CI 0.40-0.74; P<0.001). The composite endpoint of death from any cause, repeat hospitalization or cardiac symptoms were better in the TAVI group, despite the higher incidence of major strokes and major vascular events.
Conclusion that TAVI Has a Promising Future
Transcatheter aortic valve implantation is a promising procedure for the treatment of high-risk AS patients. Although still an investigational procedure in the United States, technological improvements and procedural expertise will widen the spectrum of suitable patients and allow for a prudent testing of these technologies in a broader group of individuals. The long-term efficacy and cost-effectiveness of TAVI compared to conventional AVR remains to be determined. The device improvement in terms of lower-profile delivery systems, valve retrievability and increased durability will enhance the safety of this procedure and may extend indications to the lower
risk populations.
References
1. Ambler G, et al. “Generic, simple risk stratification model for heart valve surgery.” Circulation, 2005.
2. JM B, et al. “Isolated aortic valve replacements over 10 years in North America: changing risk, valve type and outcome in the society of thoracic surgeons database.” Presented at the 2008 Western Thoracic Surgical Association Annual Meeting.
3. Iung B, et al. “A prospective survey of patients with valvular heart disease in Europe: The Euro Heart Survey on Valvular Heart Disease.” European Heart Journal
4. Bach DS, et al. “Unoperated patients with severe aortic stenosis.” Jounal of the American College of Cardiology
5. ACC/AHA guidelines for the management of patients with valvular heart disease. A report of the ACC/AHA. Journal of the ACC
6. Feldman T. “Core curriculum for interventional cardiology: percutaneous valvuloplasty.” Catheter Cardiovascular Interventions
7. Lieberman EB, et al. “Balloon aortic valvuloplasty in adults: failure of procedure to improve long-term survival.” Journal of the American College of Cardiology
8. Andersen HR, et al. “Transluminal implantation of artificial heart valves. Description of a new expandable aortic valve and initial results with implantation by catheter technique in closed chest pigs.” European Heart Journal
9. Pavcnik D, et al. “Development and initial experimental evaluation of a prosthetic aortic valve for transcatheter placement. Work in progress.” Radiology
10. Cribier A, Eltchaninoff H, Bash A, et al. “Percutaneous transcatheter implantation of an aortic valve prosthesis for calcific aortic stenosis: first human case description.” Circulation
11. Cribier A, et al. “Treatment of calcific aortic stenosis with the percutaneous heart valve: mid-term follow-up from the initial feasibility studies: the French experience.” J Am Coll Cardiol
12. Cribier A, et al. “Early experience with percutaneous transcatheter implantation of heart valve prosthesis for the treatment of end-stage inoperable patients with calcific aortic stenosis.” J Am Coll Cardiol
13. Coeytaux RR, et al. “Percutaneous heart valve replacement for aortic stenosis: state of the evidence.” Ann Intern Med
14. Vahanian A, et al. “Transcatheter valve implantation for patients with aortic stenosis: a position statement from the European Association of Cardio-Thoracic Surgery (EACTS) and the European Society of Cardiology (ESC), in collaboration with the European Association of Percutaneous Cardiovascular Interventions (EAPCI).” EuroIntervention
15. Sharp AS, et al. “First trans-axillary implantation of Edwards Sapien valve to treat an incompetent aortic bioprosthesis.” Catheter Cardiovasc Interv
16. Zajarias A, et al. “Outcomes and safety of percutaneous aortic valve replacement.” J Am Coll Cardiol
17. Hanzel GS, et al. “Retrograde percutaneous aortic valve implantation for critical aortic stenosis.” Catheter Cardiovasc Interv
18. Giannini C, et al. “Dysfunction of a 21-mm aortic bioprosthesis treated with percutaneous implantation of a CoreValve prosthesis.” J Cardiovasc Med
19. Taramasso M, et al. “First-in-man case report of the use of an Edwards-Sapien valve to treat a regurgitant CoreValve aortic valve prosthesis.” Catheter Cardiovasc Interv
20. Martin JL, et al. A randomized trial comparing compression, Perclose Proglide and Angio-Seal VIP for arterial closure following percutaneous coronary intervention: the CAP trial. Catheter Cardiovasc Interv
21. Dosluoglu HH, et al. “Total percutaneous endovascular repair of abdominal aortic aneurysms using Perclose ProGlide closure devices.” J Endovasc Ther
22. Lee WA, et al. “Midterm outcomes of femoral arteries after percutaneous endovascular aortic repair using the preclose technique”. J Vasc Surg.
23. Sharp AS, et al. “A new technique for vascular access management in transcatheter aortic valve implantation.” Catheter Cardiovasc Interv
24. Webb JG, et al. “Percutaneous transarterial aortic valve replacement in selected high-risk patients with aortic stenosis.” Circulation
25. Thomas M, et al. “Thirty-day results of the Sapien aortic Bioprosthesis European Outcome (SOURCE) Registry: A European registry of transcatheter aortic valve implantation using the Edwards Sapien valve.” Circulation
26. Leon MB, et al. “Transcatheter Aortic-Valve Implantation for Aortic Stenosis in Patients Who Cannot Undergo Surgery.” N Engl J Med
27. Piazza N, et al. “Procedural and 30-day outcomes following transcatheter aortic valve implantation using the third generation (18 Fr) CoreValve revalving system: results from the multicentre, expanded evaluation registry 1-year following CE mark approval.” EuroIntervention


 April 24, 2026
April 24, 2026