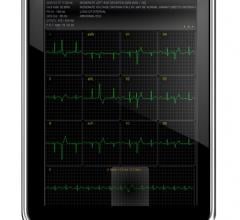
Dr. Lou Samuels used Abiomed's AB5000 BIVAD to help 77-year-old Rosemary Donaghue recover her own heart - she had developed shock in the OR and failed to come off a heart-lung machine. The device was successfully explanted after 10 days, Dr. Samuels said.
Dead is dead — everyone knows it, especially physicians. And what’s dead can’t be recovered; or can it?
Startling developments in heart research, combined with a growing body of evidence that demonstrates heart recovery potential through mechanical left ventricular devices, are creating a change in the way doctors understand and treat stunned, damaged and even “dead” heart muscle.
They’re also shifting some of their long-held beliefs about the primary objectives for acute and chronic heart failure patients, realizing that recovering the patient’s own heart is more and more viable as an end goal — rather than approaching mechanical assist devices solely as bridge to transplant or permanent destination therapies, though these indications are certainly still appropriate for many patients.
Resting and recovering a heart that has been ravaged by an acute M.I. or myocarditis, a cardiac virus, is seen today as an achievable objective for a great many more patients than even 10 years ago through the use of both short- and longer-term ventricular assist devices (VADs). And saving patients who have gone into cardiogenic shock (CS) — the shutdown of brain and organ function due to insufficient perfusion — is also more attainable with the advent of minimally invasive VADs that cardiologists can reach for at the front door of ensuing trouble, right in the cath lab, without waiting for the OR team to assemble for surgical intervention.
But how do physicians determine which hearts — and damaged heart muscle — are recoverable? To their surprise, heart specialists are witnessing total heart recoveries even where myocardium appeared to be dead. Rejuvenation is possible not only in stunned myocardium, doctors say, but cell regeneration may even occur in tissue that has initially been assessed as completely necrotic.
“Ten years ago I would have told you that dead muscle is dead muscle and forget about it,” said Lou Samuels, M.D., professor of Cardiothoracic Surgery and director of the Heart Transplant program at Lankenau Hospital, Philadelphia. “Now I will tell you I don’t know. One of my former colleagues coined a term, ‘Zombie Myocytes’ — in other words they look dead in the beginning, and then a week later it sort of doesn’t look as dead, and then another week or two later it looks alive.”
Dr. Samuels says that European physicians are discovering that some myocytes have a degree of apoptosis — cellular death — that was previously believed to be irreversible.
“Well, it is not,” asserted Dr. Samuels. “There is some degree of reversibility that we have yet to understand, but by virtue of resting and recovering and repairing these hearts, some of these so-called dead-looking myocytes come back to life.”
Make it Take a Break
Resting and unloading the heart suddenly takes on new meaning if even seemingly dead myocardium can be brought back — not in a day or two, but over the course of at least 30 days or perhaps three to nine months or more. But it won’t take a voluntary holiday — a damaged heart “that has taken a beating from the M.I. cannot rest; it must keep working,” says Michael Garippa, president of CardiacAssist. “And it will do irreparable damage to itself,” he said. Ultimately, cardiogenic shock — which is the leading cause of death at hospitals, according to Garippa — is imminent when the heart no longer pumps sufficient flow to the body,
Allowing the heart to take a break from its work can be accomplished through either (1.) a percutaneously inserted short-term VAD, such as FDA-cleared TandemHeart by CardiacAssist or Abiomed’s investigational devices, Impella 2.5 or 5.0 (2.) a paracorporeal VAD, such as Abiomed's AB5000 or the Thoratec VAD or (3.) a surgically implanted VAD, such as Thoratec’s I-VAD, HeartMate XVE or the still-in-trials HeartMate II. (This is by no means a comprehensive list.)
Imaging with sophisticated technologies, such as PET/CT, that weren’t available a decade ago, doctors can visualize myocardium that isn’t moving and discern that cells are actively metabolizing, according to Leslie Miller, M.D. — he is chief of Cardiology and director of Heart Failure and Transplant at Georgetown University and Washington Hospital. MRI and echo are also useful to physicians in their analysis of the heart’s true condition.
“[Through] CT and PET imaging I think we are going to be able to get a better sense of whether muscles are irreversibly lost and dead and those that might have some potential for recovery,” said Dr. Miller.
And if swallowing the dead-come-back-to-life idea is too big a pill just yet, another view on recovering the heart that’s been partially destroyed still applauds the benefits of re-establishing perfusion and resting the heart.
“Dead heart muscle that is totally necrotic does not regenerate,” said David Holmes, M.D., professor of Medicine and consultant in cardiovascular diseases at Mayo Clinic. “What can happen is, we can restore blood flow to the regions of myocardium around that area of necrotic tissue and hopefully then improve the function.”
Dr. Holmes does concur with Dr. Samuels and Dr. Miller that looks can be deceiving, and you can’t always judge a heart by its dead-looking cells.
“In some patients it looks dead, and it doesn’t move very much because [cells] haven’t had any blood flow,” said Dr. Holmes. “Trying to decide if something is not recoverable or is recoverable — damaged versus ischemic necrosis — is a field that is in evolution. With MRI [for example], we can look at very discreet areas of necrotic tissue and decide whether it’s dead or whether it is alive.”
The one potential drawback associated with resting the heart completely, according to Dr. Miller, is that remaining inactive too long may result in some deterioration.
“If you look at someone who has had their leg rested in a long cast and then you take the cast off four to six weeks later, you can see a marked atrophy of the leg muscles,” said Dr. Miller. “So totally resting the heart may lead to atrophy that is disadvantageous.”
Do or Die
Nevertheless, use of VADs is undeniably essential for saving lives, and the devices are becoming ever-better and ever-smaller. Experts agree that patients who receive any type of VAD would most certainly be dead without it, and companies producing the devices are dedicated to not just improving their products but to improving the rates of survival among the many and varied types of patients who suffer from diverse manifestations of heart disease.
The pursuit of recovering the patient’s own heart, and in essence handing their lives back to them, is on the front burner for both practitioners and industry — it’s even a passion for some, including Dr. Samuels, who is looking for the “silver bullet” to find technology solutions to treat end-stage heart failure, both acute and chronic. The passion is professional and personal, he says, because he watched his father die from heart failure at a time when “there wasn’t a whole lot they could do for him.”
Heart recovery should be an active pursuit as well, he and others believe. Strategies that comprise a VAD along with medical therapies and, in the future, stem cell and hormone treatments, enable physicians to take the upper hand from disease rather than having to always passively react or helplessly wait.
“If you combine [use of a VAD] with other medical therapies such as stem cells, that combination in the future will achieve a lot more recovery of the natural heart than just the device alone,” said David Farrar, vice president, Scientific Affairs at Thoratec.
What is key in the present, however, is early intervention with the VAD — sooner rather than later, Dr. Samuels and others say, is the pre-emptive approach to stabilize patients and keep them either from slipping into cardiogenic shock or rescuing them out of it before irreversible brain and organ damage occurs. This protocol, if you will, could even offset the disparity between VAD-related expenses and actual CMS reimbursement, although that arena is improving, sources say.
The point is this, says Dr. Samuels: rapidly restoring circulation, adverse outcomes such as kidney failure (and the need for dialysis), liver failure, pulmonary congestion (and the need for ventilation) — all of which translate into elongated hospital stays and outrageous costs — can be averted.
Breaking from Tradition
The standard protocol for treating cardiogenic shock (CS), followed by many cardiologists at many U.S. institutions, is to initiate a series of drugs — inotropes and vasodilators. If this path is unsuccessful, they place an intra-aortic balloon pump (IABP). IABPs, which are relatively inexpensive and plentifully stocked at most hospitals, are used to establish a degree of circulation in order to stabilize the failing patient. The terrible irony, however, is that mortality outlook for CS patients on inotropes and IABPs is pretty poor. While the intent is to provide blood flow, it can be a treatment path that is also a double-edged sword.
“The inotropes cause the [heart] muscle to trigger, so they do get some pumping function out of the left ventricle,” said Mike Minogue, CEO of Abiomed. “However, remember, this muscle is being deprived of oxygen as it is stunned — and now you are making that area work harder, which is detrimental to recovery. If they don’t administer the inotropes, then they are not going to get enough pumping blood, which means organs are going to fail. And if two organs fail, mortality rate is 80 percent. But a patient that gets three inotropes also has a mortality rate of 80 percent.”
Starting an IABP in tandem with one inotrope, according to Minogue, is beneficial to a percentage of patients — but they will still be left with a small infarct in the muscle, he says. If true heart rest and recovery hasn’t been addressed, the patient may become more stable but has lost a percentage of muscle in the left ventricle, which decreases ejection fraction.
By adding minimally invasive percutaneously inserted VADs to their cath lab toolbox — such as TandemHeart and Impella 2.5 following its FDA clearance — physicians can quickly restore sizeable blood flow and rapidly prevent organ shutdown, right in the cath lab.
Halting the deadly course of cardiogenic shock through early intervention can provide the patient stability that doctors need in order to step back, take a deep breath, gather all the facts — medical and physiological comorbidities as well as the mental and sociological factors — and then make an educated decision about the next treatment step.
“Some hearts will recover, but it’s a spectrum,” said Farrar. “That’s why heart disease is such a big epidemic — it’s not just one disease and you don’t need just one therapy. It’s a full range of different pathologies and a whole range of events. What physicians like to have is a large armament of different devices to treat that spectrum.
“Short-term devices — the one-day or one-week devices,” Farrar continued, ”play a very valuable role in this bridge-to-decision process.”






 March 06, 2024
March 06, 2024