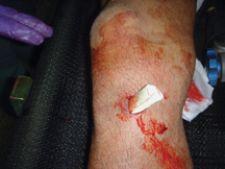
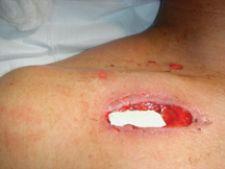
HemCon's ChitoFlex Dressings have been used by the military in Iraq and is now available for civilian use.
The battle for infection control is fought daily in wound management where the body's first line of defense against microbes has been breeched.
Sometimes something old is made new again with a twist of new technology, as is the case in new infection-fighting wound care products that use shrimp shells, honey and silver as their key ingredients.
The silver bullet
Silver-based bandages and device coatings offer a potential answer for fighting bacteria, viruses, algae and fungi. Silver’s antibacterial properties have been used for centuries and were used in drugs and antibacterial ointments prior to the introduction of antibiotics in World War II. Silver ions form strong molecular bonds with other substances used by bacteria in cellular respiration. Once the ion combines with these molecules they are rendered unusable by bacteria and it leads to death.
“The reason for using silver is because it is very effective in small amounts,” said Bruce Gibbins, Ph.D., chief technical officer, chairman of AcryMed.
After starting the AcryMed research and development company in 1993, he said it quickly concentrated on silver-based wound care and infection control technologies. The company focused on stabilizing silver’s properties to prevent it from staining skin and increase its effectiveness by controlling the release of ions. Gibbins said this led to the release of silver-based wound dressings in 2001. More recently, the company developed silver-ion nanotechnology that allows dip-coating of medical devices and will not easily wash off. AcryMed licenses its technology to numerous manufacturers, including Baxter, I-Flow, MedLine and Edwards Lifesciences.
AcryMed has developed several wound dressings that use microlattice technology with a stabilized, controlled-release silver-ion formula that works up to seven days without harming healthy tissue. The bandages also help regulate moisture at the wound.
Studies conducted on the company’s SilvaGard nanocoating have been shown it to help cut hospital-acquired infection rates in half, company officials say. The technology is incorporated into I-Flow's ON-Q PainBuster post-surgical pain relief pump and ON-Q SilverSoaker antimicrobial catheter. The results of a study on that device released last September showed a 55 percent reduction in surgical site infection rates and significantly shorter hospital stays in a 14-center infection surveillance study involving 289 colorectal surgery patients.
In November Baxter Healthcare Corp. received FDA clearance for its needleless V-Link Luer-activated device (LAD), an IV connector containing an AcryMed silver-based antimicrobial coating. Baxter says the device has been shown to kill 99.9 percent of specific common pathogens known to cause catheter-related bloodstream infections.
Silver nanocoatings are also being applied to nonmedical items, including bed mattresses and computer keyboards.
However, there is some apprehension among doctors that overuse of silver may also lead to silver-ion resistant strains of bacteria, but Gibbins says this is unlikely.
“The way silver kills and the way antibiotics kill is very different,” he said.
Silver ions attack several parts of an organism at once, which Gibbins says would be similar to a car losing its brakes, transmission, electrical and fuel system all at once. For that reason, he says it is unlikely germs will have time to develop multiple levels of resistance all at once. He also says antibiotic-resistant bacteria have developed only in the past 50 years, while silver has been used by humans for thousands of years and there are no known silver resistant bacterial strains.
Folk remedy for infection control
Honey is another product that has been round for thousands of years and used as a folk remedy and is now seeing renewed interest in honey-based wound dressings. Honey-based products have been available in Europe where they compete against silver-based dressings, but were only recently released in the U.S.
Natural honey has a tendency to liquefy with body heat, so the new honey-based bandages use modified honey with a viscosity-increasing agent. Different honeys have varying antibiotic properties, but researchers say the manuka Leptospermum honey is best.
A 2007 Irish study on the use of honey in the treatment of chronic wounds showed active manuka honey helped cleanse and heal wounds. It also provided antimicrobial activity. Overall, the study showed when compared to standard hydrogel, both under compression, over a 12-week period, the group treated with honey had a higher rate of debridement, faster healing rates and reduced infection. The honey also was effective in helping completely eliminate bacteria in seven out of the 10 wounds in the study that were infected with MRSA.
Last fall Derma Sciences Inc. received FDA clearance for its API-MED Active Manuka Honey Absorbent Dressing. While the FDA has not issued an antibacterial indication, research continues to show honey has some antimicrobial properties.
“Honey has an antimicrobial basis,” said Steven J. Kavros, DRM, Mayo Clinic, Rochester, MN. “It puts down a barrier that lets the wound fluid in and out and helps keep the bacterial load down.”
He says the Mayo Clinic uses a variety of bandages, including silver-based bandages that he says work very well. Dr. Kavros started using the Derma Sciences dressings about five months ago on lower extremity diabetic and pressure ulcers, and on venous, ischemic and neuropathic wounds. While he warns his study is on-going, he has seen less reoccurrence of infection than with standard dressings. He said it also seems to aid in the granulation of tissue and helps healing by keeping the wound moist. Sugar in the honey also changes the osmotic features of the wound, helping draw away “the slush,” which helps clean the wound, he says.
The honey dressing is very low maintenance, Dr. Kavros says. Drainage usually mandates how often you need to change a dressing, but in the case of the Derma Sciences bandage he says it can sometimes be kept in place two or three days.
“The nurses who take care of the patients have been very pleased, because it has helped reduce the time they spend changing bandages,” Dr. Kavros said.
Shrimp help save soldiers
Cardinal Health distributes the HemCon Bandage, which reportedly instantly stops bleeding in trauma patients using a shrimp shell-based dressing that gels on contact with blood.
“Hemorrhage is the leading cause of preventable death on the battlefield,” said Sudip Bose, M.D., FACEP, FAAEM, attending emergency physician, Advocate Christ Medical Center, Oak Lawn, IL, assistant clinical professor, and a former major and sole physician with the an infantry battalion of the U.S. Army’s 1st Cavalry Division in Iraq. “If you look at it statistically, as an amputee in the Korean War your survival rate was low. However, now soldiers have a higher survival rate, and much of this can be attributed to better hemorrhage control on the battlefield.”
Dr. Bose said HemCon Bandages are credited with saving more than 100 lives on the battlefields of Iraq since being introduced by the U.S. military in 2003. However, he believes this number is much higher. The U.S. Army Surgeon General's office says the HemCon Bandage has a 97 percent effective rate in controlling bleeding on the battlefield and it is especially effective with amputations and penetrating wounds.
“In my personal experience, HemCon has saved countless lives,” Dr. Bose said. “There was one situation when we were providing medical care while under attack during an ambush. A blast left several soldiers injured. As I was tending to other soldiers, one soldier was exsanguinating from an amputated leg and tourniquets were not controlling the bleeding. My medic quickly placed a HemCon Bandage he was carrying on the extremity injury. During the chaotic moments under attack, the HemCon Bandage eased much of our stress. This soldier would certainly have bled to death if it were not for the bandage.”
He says it is more effective than the usual compression bandage because it uses an adhesion technology to stop bleeding and seal the wound within two to five minutes. This adhesion technology stems from the manufacturing process in conjunction with the bandage's use of chitosan, the compound derived from shrimp shells.
The bandage’s chitosan properties also provide an antibacterial barrier to help prevent infection, Dr. Bose said. HemCon’s temporary surgical dressing ChitoFlex - Surgical, carries an antibacterial claim against a number of bacteria including MRSA, and uses the same technology platform as the HemCon Bandage. ChitoFlex is FDA cleared and will be launched in September for multiple trauma and damage control in surgery.
“I practice in one of the nation’s busiest trauma centers, and I've seen severe bleeding cases resulting from trauma, such as motor vehicle accidents, knife injuries, gunshot wounds and lacerations, where it was critical that we control the bleeding in order to save the patient's life,” Dr. Bose said. “By controlling blood loss, the HemCon Bandage also helps reduce the need for costly infusions. Most importantly, the bandage affords us critical time in the ER to administer care. In many cases, if we weren't able to use the HemCon Bandage, our patient’s would not have had a positive outcome.”