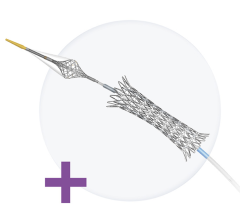
Cordis is developing the NEVO as its next generation drug-eluting stent. Nevo uses tiny reservoirs in the struts to hold a bioabsorbable drug polymer and to reduce both the amount of polymer and its contact with the vessel wall.
The polymer coating on drug-eluting stents (DES) used to carry the antiproliferative drugs cause an increased risk of stent thrombosis, months or even years after a stent is implanted. This has led stent manufacturers to look for or ways to eliminate the vessel irritating polymers for better biocompatibility usually associated with bare metal stents (BMS).
State manufacturers have developed both bioabsorbable polymers and totally-bioabsorbable stents. Boston Scientific, Cordis and Abbott all have stents in development with plans for introduction to market in the next five years. Medtronic is also developing a bioabsorbable polymer coating it has tested in animal studies. However, with the high cost of bringing a new DES to market, Medtronic wants to see how well its Endeavor and Resolute stents compare to any new competitors in long-term studies, because Medtronic says its stents already have a rate well below 1 percent for polymer-induced stent thrombosis.
NEVO Introduces Drug Reservoirs
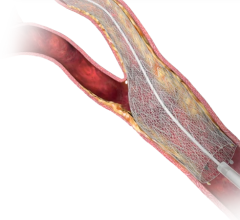
DES introduced in the U.S. since 2003 have consisted of a BMS with a polymer drug-eluting coating, but that formula is about to change with the Cordis NEVO stent now in trials. The stent uses a unique cobalt-chromium platform with tiny holes throughout the struts that act as drug micro-reservoirs for a sirolimus-containing bioabsorbable polymer. The reservoir technology was purchased from Conor Medsystems in 2007. This unique design allows drug delivery from a stent with a surface that is 75 percent bare metal upon insertion and becomes purely bare metal following drug delivery and polymer bioabsorption in three to four months.
“We feel NEVO really is a true second generation stent technology,” said Campbell Rogers, M.D., chief scientific officer and global head of research and development for Cordis.
He said Cordis is putting most of its stent resources into NEVO and hopes to file for CE mark by the end of 2009. Cordis plans to submit for FDA approval by the end of 2011.
Some results from the NEVO RES-ELUTION I (RES-1) study released during EuroPCR 2009 earlier this year showed significantly less in-stent late loss and no reports of stent thrombosis at six months when compared to the Taxus Liberte DES. Late lumen loss was reduced by 64 percent in the NEVO arm as compared to the Taxus Liberte. Angiographic results showed NEVO had a major reduction in restenosis compared to the Taxus Liberte (1.1 percent in the NEVO as compared to 8 percent). NEVO MACE (major adverse coronary events) were also significantly reduced compared to Taxus Liberte (4.1 percent vs. 7 percent). Cordis said data from the study will support its regulatory filing for a CE mark in Europe.
“We are really enthused by that data,” Dr. Rogers said. “It showed lower MACE, lower target legion revascularization, lower thrombus – lower everything – compared to TAXUS.”
He said the stent’s design means less polymer is in contact with the vessel wall, potentially reducing the risk of stent thrombosis. He said the company hopes this will translate into a much shorter period of antiplatelet therapy.
Dr. Rogers said Cordis is also developing ways to alternate the types of drugs loaded into each micro-reservoir. This would allow combinations like sirolimus and anti-thrombotics to be loaded into alternating reservoirs.
Results from the RES-1 trial compare much better than the previous CoStar stent Conor Medsystems offered, which used the same stent, but was loaded with paclitaxel. The COSTAR II trial compared CoStar to TAXUS, but data showed it was inferior to TAXUS and the stent was pulled off the market. Dr. Rogers said the stent’s performance was greatly improved with the use of sirolimus.
He said the company is also developing on a totally bioabsorbable stent, but it will not be targeted for the coronary arteries.
Boston Scientific is developing the JACTAX stent that uses a bioabsorbable polymer and seems likely to receive FDA clearance before NEVO. But Dr. Rogers claims NEVO will have some advantages over JACTAX in that paclitaxel is not as effective as sirolimus and the Labcoat polymer requires a longer dissolution time and cannot be loaded with as much drug as the NEVO polymer.
NEVO will be pitted again the XIENCE V everolimus-eluting coronary stent in the upcoming NEVO II trial. The study will enroll thousands of patients with coronary artery disease and will include expanded enrollment in multiple patient subgroups. The primary endpoint of the study is target lesion failure at 12-months.
Boston Seeks Clearance of Bioabsorbable Coating
In January 2009 Boston Scientific purchased Labcoat Ltd., a development-stage drug-eluting stent technology company in Galway, Ireland. The company developed a new technology for coating drug-eluting stents using droplets of a biodegradable polymer and drug formulation to create a thin coating (less than 1 micron as compared to 18 microns for TAXUS) confined to the outer surface of a coronary stent. The technology significantly reduces the amount of polymer and drug to which the vessel wall is exposed, while minimizing polymer and drug on the inner surface of the stent where endothelial cell growth is required for healing. The biodegradable coating dissolves, leaving behind a bare-metal stent. Boston Scientific said this approach is intended to provide the same degree of restenosis reduction as a conventional drug-eluting stent, but faster and more complete vessel healing after stent implantation.
The JACTAX stent consists of a Boston Scientific bare-metal Liberte stent coated on its outer surface with a Labcost biodegradable polymer containing paclitaxel.
Labcoat presented clinical trial data on the JACTAX at TCT 2008, which showed promising results for both restenosis and strut coverage nine months after implantation. The stent was also used in two other European trials.
Dennis Fiedler, a vice president in research and development at Boston Scientific, said data from these trials is being used to support the JACTAX CE mark submission made earlier this year. He said the U.S trials for FDA submission are hoped to begin in early 2010. Fiedler said Boston Scientific is “vigorously investing” in the bioabsorbable coating technology and plans to use it on the TAXUS Element platform with both paclitaxel and everolimus drug coatings.
Terumo and Biosensors
Biosensors received CE mark approval in January 2008 for its BioMatrix Drug-Eluting Coronary Stent System, The DES uses a polylactic acid bioabsorbable polymer and the company’s proprietary drug, Biolimus A9, which is an analogue of sirolimus. The polymer only coats the outer (abluminal) side of the stent and dissolves in six to nine months.
Terumo licensed Biosensors’ BioMatrix technology and also announced its CE mark approval for its NOBORI DES in January 2008. Biosensors and Terumo entered into a licensing agreement in 2003, allowing Terumo to sell the NOBORI exclusively in Japan and nonexclusively in countries outside Japan, excluding the United States. Terumo shares a portion of the revenues with Biosensors.
The NOBORI showed excellent efficacy and safety in several clinical trials. (1) In randomized studies versus TAXUS Express and TAXUS Liberte, the NOBORI stent proved its noninferiority and even superiority in efficacy endpoints such as late loss, with a very low frequency of adverse cardiac events and no stent thrombosis up to one year. In NOBORI CORE, a comparative study versus the CYPHER DES, NOBORI showed excellent performance with very low rate of adverse cardiac events. Terumo said the overall restenosis rate in all NOBORI trials was as low as 0.5, and no late stent thrombosis was recorded in any of the trials.
(1) “A Randomized Comparison of the NOBORI Biolimus A9-Eluting Coronary Stent with the Taxus Liberté Paclitaxel-Eluting Coronary Stent in Patients with Stenosis in Native Coronary Arteries: The NOBORI 1 Trial–Phase 2,” Bernard Chevalier et al. Circulation: Cardiovascular Interventions. 2009, issue 2, pages 188-195
For More Information:
www.abbott.com
www.bostonscientific.com,
www.cordis.com
www.medtronic.com
www.mivtherapeutics.com
www.xiencev.com


 November 24, 2025
November 24, 2025