March 17, 2010 – Body size, gender and the complexity of heart disease significantly influence how much cumulative radiation skin dose patients receive during percutaneous coronary intervention (PCI) therapy, according to a new Mayo Clinic study. The study was undertaken as a quality control initiative to reduce the potential radiation risks of cancer to patients and PCI operators.
Presented at the annual meeting of the American College of Cardiology this week, the review of 14 months worth of radiation data from 1,827 adult patients is an important early step in understanding ways to improve PCI safety and quality while optimizing therapeutic benefits. The Mayo Clinic study identified 20 clinical traits and circumstances that help predict whether a patient likely received higher or lower doses of radiation.
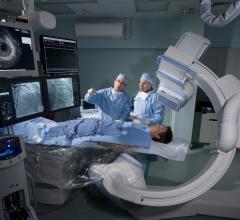
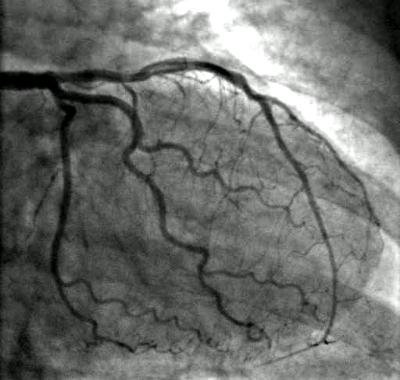
PCI owes its precision, safety and effectiveness to X-ray fluoroscopy imaging. The amount of radiation dose used during procedures is generally much greater than that used for a typical X-ray image, such as a chest X-ray. But because a chest X-ray is usually a screening test and a PCI is a lifesaving procedure, from the clinical perspective, the risk of not performing the PCI is much greater than the predicted radiation risk associated with the procedure.
Mayo study results show:
• Indicators of higher radiation dose included male gender higher body mass index (BMI); more complex disease, such as multiple diseased vessels or complex anatomy and lesions in the vessels; and previous history of coronary artery bypass graft (CABG) surgery.
• The median patient BMI was 29.7, with most patients having a BMI between 21 and 44.6. A BMI less than 30 can fall into normal (20–24.9) or overweight (25–29.9) categories.
• The median cumulative skin radiation dose was 1.5 Gray (Gy), a unit of absorbed radiation, with a range 0.34 Gy to 4.5 Gy. In general, the cancer risk for a typical PCI is likely about 0.05 percent, whereas the “natural cancer rate” from daily exposure to background radiation is about 35 percent, the Mayo team noted.
Implications for Cure
“Radiation risk is a recognized hazard of our specialty that has not been systematically or aggressively addressed,” explains Chet Rihal, M.D., lead cardiovascular physician on the study. “But our commitment to patient safety and quality at Mayo Clinic, and to protecting operators who perform the therapy, makes this a priority issue for us. The next step for us is to follow-up from this initial identification of the problem and lead efforts to formulate specific practice changes clinicians can use to improve safety while maintaining quality.”
Data also showed radiation doses comparable patients received differed depending on which of the 13 physicians treated them. Dr. Rihal says investigating possible causes of this finding is among the goals of the next phase of study.
Context of the Study
Nationwide, concern is growing across medical fields about reducing risks of radiation from all sources, such as X-rays and computed tomography (CT) scans. Recently the FDA has been addressing accidental cases of overexposure to radiation in certain specialties. The Mayo Clinic study cases differ from the FDA efforts. Mayo’s cases do not involve accidents or overexposure, but commonly accepted clinical best practices. “This work is a natural expression of Mayo’s historic commitment to improving patient safety, care and quality of treatment,” Dr. Rihal said. “We aren’t correcting errors, just improving the way things are done for all concerned.”
The Mayo study is the largest to identify clinical conditions that correlate with radiation dose level, and is therefore is an important first step leading to protocols to reduce radiation levels. “There is no standard model of the clinical determinants of radiation skin dose in PCI, so by using clinical data from a large sample of Mayo Clinic adult patients and commonly accepted statistical methods, we identified correlations between clinical variables and radiation dose that we hope will be useful in improving care,” said Kenneth Fetterly, Ph.D., another of the Mayo study authors.
Collaboration and Support
In addition to Dr. Rihal and Fetterly, other Mayo Clinic physicians and scientists who worked on the study were Ryan Lennon, Malcom Bell, M.D. and David Holmes Jr., M.D. Their work was supported by the Mayo Foundation for Medical Education and Research.
For more information: www.mayo.edu, www.mayoclinic.com

 October 24, 2025
October 24, 2025