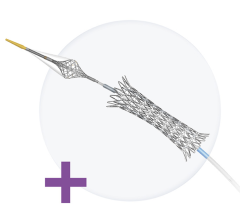
Capella Inc.'s Sideguard stent
iffering approaches for the treatment of coronary bifurcation and ostial lesions (CBOL) continue to feed the debate over which stent designs and stenting techniques are most effective.
While, for the most part, bifurcations and ostial lesions are still treated with conventional tubular DES, new innovative stents with built-in side structures are being developed to treat the side-branch ostium and prevent renarrowing.
Providing ostial support
As much as 30 percent of coronary artery disease occurs at a bifurcation, where one artery branches into two smaller arteries -- one being the continuation of the main branch and the other often referred to as the side branch. These lesions pose a serious challenge to interventional cardiology as bifurcations present a common location for the buildup of plaque and are particularly difficult to treat with currently available stents.
Over the years, cardiologists have tried to adapt tubular stent technologies to address CBOL to obtain better results, leading to the development of creative and innovative stenting techniques to work in unconventional ways.
A key factor to successfully treating bifurcations involves providing ostial support. Frequently, the bulk of the stenosis will be present in the main vessel with minimal or no disease in the side branch. However, when one stent is used it can cause a “snowplowing” effect. This approach provides inadequate protection to the ostium. Leaving the ostium exposed and unprotected can lead to increased risks of ostial spasm and side branch closure.
Specialty coronary main vessel coronary stents with side branch apertures have done little to improve ostium protection.
Advanced Stent Technologies (AST) Inc., which was acquired by Boston Scientific, was one of the first small companies to develop a “true” bifurcation stent. Developed based on its tubular stent cousin, the first AST bifurcation stent was unique in design because it featured a side-hole aperture with a slightly-flared proximal lip design that was supposed to provide support to the ostium.
Several other companies, including Abbott/Guidant, Invatec, Medinol and Mivasys, have followed suit, creating their own main vessel bifurcation stent and adopting similar stent designs. All these companies have incorporated some type of side branch aperture or ostium scaffolding feature into their stent’s design. Nevertheless, these bifurcation stents remain main vessel stents with dual-delivery systems, making the devices more challenging to place and deliver, while requiring the use of a second tubular stent in the side branch.
Stent the side branch first
After many years of practice and the creation of several pioneering bifurcation two-stenting techniques, restenosis and TLR rates, companies are now developing side-branch stents.
Recently, Boston Scientific successfully implanted its TAXUS Petal Bifurcation Paclitaxel-Eluting Stent System (TAXUS Petal Stent) in a patient in New Zealand, marking the beginning of the TAXUS PETAL I First Human Use (FHU) Trial.
The TAXUS Petal Stent consists of a traditional drug-eluting stent with an innovative side structure — the Petal Strut — in the middle of the stent that opens into the side branch. The TAXUS Petal is designed to provide access, coverage and support to the critical areas of the bifurcation and uses a proprietary platinum chromium alloy. According to Boston Scientific, it used platinum chromium to offer an improvement over stainless steel and cobalt chromium. It believes the platinum chromium enables even thinner struts, increased flexibility and improved radiopacity. The TAXUS Petal Stent is coated with a combination of the paclitaxel drug and translute polymer.
“A major strength of the TAXUS Petal Stent design is to provide consistent mechanical support and drug application not only to the main branch but also to the side-branch ostium, where renarrowing is common with other techniques used today,” said John Ormiston, M.D., at Auckland City Hospital, Auckland, New Zealand, who performed the first procedure using the TAXUS Petal Stent.
One of the pioneers in treating ostial and bifurcated lesions with side-branch stents is Cappella Inc. The company’s approach is to protect and deliver drugs to the ostium, while supporting the side-branch. To do this it developed the Ostium Protection Device (OPD), which has a trumpet-shape design and the side-branch stent is a self-expanding stent.
The procedure begins by first stenting the side-branch to ensure good stent-to-ostium and side-branch wall apposition by keeping the main-branch’s lumen free for the advancement of a second stent and kissing stent deployment, while eliminating stent deformation and minimizing trauma to the vessel wall.
The OPD reached a milestone in December of 2006 with the successful implantation of its Sideguard dedicated side-branch stents in two patients.
According to Eberhard Grube, M.D., chief of Cardiology and Angiology at the Heart Center Siegburg, Germany, the implantation of the stent in humans was a breakthrough in the treatment of ostial-bifurcated lesions.
“The Sideguard bifurcation stent system, which incorporates Cappella’s smart balloon-sheath SE delivery technology, allows for flawless advancement, positioning and delivery of the Sideguard stent to the side branch ostium,” said Dr. Grube. “This resulted in excellent angiographic results and very good wall apposition.”
Delivering the Sideguard over a separate wire to the side branch ostium first, and then delivering a Cypher stent in the main branch, according to Dr. Grube, simplified the bifurcation procedure.
“Today there is disagreement among clinicians when comparing
provisional stenting and the two-stent approach. We are overwhelmed by conflicting studies as to which strategy is better. The Sideguard seems to present the most logical compromise between the two approaches,” said Dr. Grube.
Advantages of the culotte technique
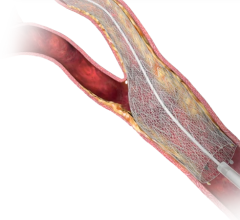
Another technique that is making inroads in coronary bifurcation treatment is the culotte bifurcation technique. While in some cases results of using the culotte bifurcation technique have not been as promising as bare metal stents, researchers have found some advantages of applying the culotte technique in combination with paclitaxel drug-eluting stents (DES) to stent provisionally, to use lower French sizes and to completely cover the coronary wall and the new carina with a single or double stent layer.
While the crush technique, which aims to reach complete coverage of the coronary wall to allow antiproliferative drugs to homogeneously distribute into the coronary walls, offers one method, a coronary bifurcation treated with the culotte technique and paclitaxel-eluting stent deployment has produced effective angiographic results.
Where a dedicated drug-eluting bifurcation stent is challenged by providing consistent mechanical support and drug application not only to the main branch but also to the side-branch ostium, where renarrowing is common, culotte stenting can provide full coverage.
According to a recently published study, “Culotte bifurcation stenting with paclitaxel drug-eluting stent,” by investigators Giuseppe Mezzapellea, Duccio Baldaria and Roberto Baglini, at the Department of Interventional Cardiology, University of Pittsburgh Medical, Centre European Medical Division and Istituto Mediterraneo per i Trapianti e Terapie ad Alta Specializzazione, they found that the “culotte treatment is able to completely cover the main and the side branch. The side branch ostium is generally covered by a single layer of stent struts, while the proximal portion of the main vessel is covered by a double layer of stent struts,” said Baglini.
When comparing the crush to the culotte technique, researchers found that the culotte technique acts more physiologically, allowing the creation of a new, homogeneously covered carina, without any crushed metal inside the coronary wall.
“The culotte technique is probably more physiological and does not allow the presence of layers of stent struts against a single coronary wall,” noted Baglini.
One of the principal concerns with drug-eluting stents is the development of late-stent thrombosis, and Baglini acknowledges that this is a safety concern with any technique using DES.
“The presence of a considerable amount of metal, especially into the proximal part of the main vessel, could be a risk factor for the development of subacute, late and very late stent thrombosis,” said Baglini.
Despite safety concerns, after 10 months of follow-up, the angiographic results in the study were positive. Although the researchers do underscore the need for more data to evaluate the potential utility of the culotte technique in treating bifurcation coronary lesions in the area of drug-eluting stents, the culotte technique offers another promising approach to completely treating the whole lesion.
Reference:
Culotte bifurcation stenting with paclitaxel drug-eluting stent. Giuseppe Mezzapellea, Duccio Baldaria and Roberto Baglini, Department of Interventional Cardiology, University of Pittsburgh, Medical Centre European Medical Division, Istituto Mediterraneo per i Trapianti e Terapie ad Alta Specializzazione, 90127 Palermo, Italy. Received 20 June 2006; accepted 6 July 2006. Available online 9 February 2007.

 November 24, 2025
November 24, 2025