The biggest issue in electrophysiology (EP) is the disparate nature of patient tests, reports, images and waveforms, and the need to aggregate all this data in one place to more efficiently care for patients with arrhythmias. This is especially true as the need to meet government-required meaningful use criteria for electronic medical records (EMRs) pushes forward and healthcare reform necessitates a deeper data integration.
There is a need in EP to make patient data more accessible in a single data management system, said Michael Mirro, M.D., FACC, cardiologist, electrophysiologist and medical director at Parkview Heart Institute, Fort Wayne, Ind. As an example of why data needs to be more accessible, he explains the complicated care of patients with atrial fibrillation. These patients typically undergo many tests for diagnosis and monitoring of the condition and are prescribed several drugs. They might also undergo more invasive treatments, such as ablations, where data is brought in from EP recording systems, hemodynamic systems and possibly imaging systems. If the information for the care of this patient is located in several separate systems or only in paper form, much time is wasted in accessing and re-entering it.
“Clinical workflow improvement is the end point of all of this,” Mirro said.
He said EP reporting systems need to integrate with stimulators, pacers, intracardiac echo (ICE), EP recording systems, ablation navigation systems, hemodynamic systems and the cardiovascular information system (CVIS). Report templates are also needed for tilt table exams, Holter monitoring, implantable devices and ablation procedures. Other integrations that are very helpful include scheduling, inventory management, billing and interfaces with picture archiving and communication systems (PACS) and electrocardiogram (ECG) management systems.
Systems should automate the transfer of information so data is only entered once into a computer system, Mirro said. This can save a large amount of staff time, especially if a system can auto-populate registry data forms, such as the NCDR ICD Registry.
“You see people doing this by hand, which is a little alarming because it is time-consuming and entering data multiple times can lead to errors,” Mirro explained.
Mirro’s hospital is using an Epic EMR system, which he said is great for primary care, but for specialties such as EP, the system lacks what is needed to properly document cases. For this reason, his EP department will soon be among the first to go live with McKesson’s recently released EP reporting system.
Watch the video “IT Considerations for Electrophysiology Reporting Systems.” To help hospitals upgrade their electrophysiology (EP) reporting systems and integrate EP into cardiovascular and hospital reporting systems, Michael Mirro, M.D., FACC, medical director, cardiology/electrophysiology, Parkview Physicians Group, Ft. Wayne, Ind., offers suggestions of what to look for.
EP Needs a Dedicated System
Mount Sinai Hospital’s Leona M. and Harry B. Helmsley Charitable Trust Center for Cardiac Electrophysiology previously used in-house built dedicated workstation software to create EP reports. The department also used separate billing, scheduling and inventory tracking systems. Each system required the same patient data to be entered repeatedly because these systems did not interface. The department wanted to integrate all of these functions into one system that was easier to use, said Nicholas Skipitaris, M.D., medical director of cardiac electrophysiology operations.
“The lesson we learned over the years [using a one-size-fits-all reporting system] is that the needs of individual departments will vary. There will always be a department that does not like the system, but it works great for all the other departments,” Skipitaris said. “My biggest complaint as an EP was that the group that developed our cardiovascular information system designed it for a cath lab that does 40,000 procedures a year. It was not centered on EP, so the reporting for our prospective was not what we needed.”
EP procedures also present challenges because of a wider variety of complications that can occur in complex ablation or device implant procedures. This variability usually requires a lot of freehand text fields. While structured reporting might be better suited for data mining, Skipitaris said unlike coronary cath lab procedures, there has not been the same level of standardization in how various EP labs around the country perform procedures and report information. For this reason, he said a fair amount of customization might be needed when implementing a new EP reporting system. Most EP reporting systems offer customization.
With EP volumes going up nationwide and the eventual requirements of Medicare to have standardized reporting, it is likely that vendors will be tasked with creating EP reporting system standards in the future.
“There is a lot more variation in EP procedures than in cath lab procedures, so it’s a lot harder to create a system that can be used in the EP environment,” Skipitaris said.
He said the department wanted a system that could allow entering data once, interoperable billing and inventory management, the ability to record metrics during procedures and medications for reports, allows for the importation and use of computed tomography (CT) and magnetic resonance imaging (MRI) 3-D reconstructions for procedural guidance and use for data mining analytics.
The hospital adopted Perminova’s EP reporting system in April 2012. The Web-based system is easy to install and upgrade and can be accessed through any browser, including when a physician is at home.
“We use the system not only as an EP reporting system, but also as a billing system,” Skipitaris said. “We also use the system as a database to track the number and type of procedures we perform. There is a significantly lower degree of data entry with the system.”
The software enables procedural scheduling and reports for cardioversions, device therapy, tilt table and ablation procedures. It also allows review of prior reports and lists reports the physician still needs to review and sign off on.
“They have done a remarkable job of delivering what we need,” Skipitaris said. “It’s the nerve center, computer-wise, for the department.”
A consideration for departments looking to purchase a new EP reporting system is its ability to interface with the hospital’s ECG management system. He said the Perminova system is not yet linked to Mount Sinai’s GE Muse system, but it would be helpful to see prior ECGs when reviewing patients with persistent issues.
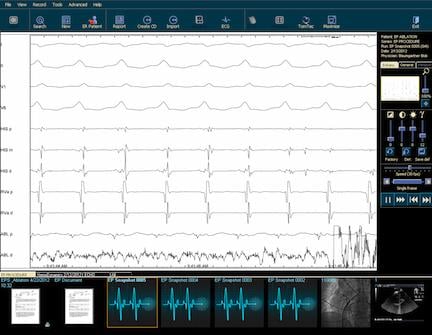
Another consideration for EP departments is having a system that allows integration of electrograms and their related measurements. Just as the bread and butter of cath lab reporting systems is the integration of angiographic image capture and cine loops, EPs need integration with patient electrograms.
Third-Party EP Integrations
There is a problem with expecting big vendors in the EP market, such as Bard, St. Jude and Biosense, to interface their technology with competitors’ systems, Skipitaris said. There is not much incentive for vendors to cooperate with their competitors, because they want customers to purchase their solutions, he noted.
“The beauty of adopting a third-party system is that they have skin in the game, so they have good reason to work with St. Jude, Bard and other vendors to make their systems work,” he explained.
Comparison Chart of EP Reporting Systems
This article served as an introduction to a comparison chart for Electrophysiology (EP) Reporting Systems. It access this chart, go to www.dicardiology.com/comparison-charts. Access requires a login, but it is free to register and only takes a moment. Participants in the chart include:
Flexible Informatics — www.encapturemd.com
GE Healthcare — www.gehealthcare.com
Lumedx — www.lumedx.com
McKesson — www.mckesson.com/cardiology
Medstreaming — www.medstreaming.com
Merge Healthcare — www.merge.com
Perminova — www.perminova.com
Philips Healthcare — www.healthcare.philips.com
Siemens Healthcare — www.usa.siemens.com/angiography
St. Jude Medical — www.sjmprofessional.com


 November 06, 2025
November 06, 2025