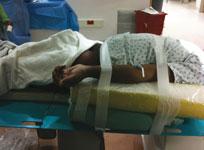
A patient is prepped for a radial access procedure using an arm board extension.
Radial access has been a standard for most patient cases for several years at both the University of Illinois at Chicago (UIC) Medical Center and the Jesse Brown VA Medical Center. The centers are located within two blocks of each other, and the two staffs work very closely. Part of their coordination has been developing training programs and best practices and protocols for radial artery access techniques.
“The whole selling point of radial access is to gain efficiency,” said Adhir Shroff, M.D., MPH, associate professor of medicine, section of cardiology, UIC. He added there is a learning curve for new operators unfamiliar with radial access techniques, but this curve can be flattened by working with and taking advice from those with experience.
The following tips are based on the experiences at UIC and Jesse Brown:
1. Conduct a Modified Allen’s Test
Both medical centers conduct an Allen’s test on all radial access patients as a “cover-your-butt” strategy to document whether there is circulation to the hand prior to the procedure, Shroff said. An Allen’s test is fast, inexpensive and easy to do and will show if the radial artery has a clear lumen and can be used for percutaneous access by measuring pulse and oximetry.
To perform the test, place a pulse oximeter probe on the first digit or thumb and record the reading. Then, occlude both the radial and ulnar arteries to notice absence of the wave form on plethysmography, then remove pressure from the ulnar artery while maintaining pressure on the radial. Observe if the wave form returns. If it does, then it is a “normal” test; if it does not, then it is an “abnormal” test.
If the color to the hand is delayed more than eight seconds or there are differences in the oximetric readings, the test is considered abnormal, said Bernadette Speiser, RN, MSN, CCRN, cardiology department manager at the cardiac catheterization lab at the Jesse Brown VA. She said about 5-10 percent of the population will have an abnormal Allen’s test.
While hand ischemia is very rare, conducting an Allen’s test may help to identify patients that may experience ischemia during a case. Close oximetry monitoring during the procedure will also help identify any perfusion issues.
At the end of the procedure, document the oximetry again.
2. Properly Prep the Patient
Make sure the IV is placed in the contralateral arm, so it is not in the way of the access arm, suggests Speiser. In addition, ensure any jewelry is removed from the wrist area and clip the wrist hair. Also, prep the femoral site as well just in case radial access cannot be made. This will save time during the procedure.
3. Use an Arm Board Table Extension
Use an arm board extension placed under the patient to allow additional room to prep and support the arm and gain radial access. UIC originally made its own boards by cutting down backboards with a saw, but professionally made boards are now available on the market.
4. Use a Dedicated Drape
Use of a specifically designed drape will make preparation easier. Also, Shroff suggests using a drape that has access points for both left and right radial access and femoral access. This allows for a rapid switch to another access site if needed.
5. Choose the Right Introducer
Introducers for radial access need to have extremely smooth transitions. Shroff said when he examines new introducers, one thing he does is close his eyes and runs the introducer through his fingers to feel for any abrupt transitions. If there are, he says he would not consider it for transradial use because if it does not comfortably fit in the artery, it may cause spasm.
Some operators say they need to make a nick to allow easy insertion of an introducer into the radial artery. However, Shroff said if you need to make a cut, it probably means the sheath being used is not good enough for radial access procedures.
Another sign the introducer may not be appropriate for radial access is if a stitch is needed to close the access site. Shroff said only a Tagaderm should be needed to close the entry site.
6. Avoid and Treat Vasospasm
The first attempt to gain radial access is usually the best attempt, as the vessel is prone to spasm, making access and the movement of wires and catheters in the vessel difficult. Shroff said spasm usually will subside in a few minutes, which can be aided with the use of additional sedation or sublingual nitroglycerin.
Talk to the patient. Shroff suggests discussing the technique with the patient, and explaining what you are doing and why. He explains this helps put the patient more at ease, which can help with issues such as vasospasm, which can be caused by a patient tensing up if they are not aware of what is going on.
Use sedation and vasodilators. If vasospasm is encountered, the first sign is usually the patient reporting pain in their arm and the catheter may feel as if it is stuck. Shroff suggests treating the spasm first with sedation and antispasmodic drugs.
Drugs to treat spasm include nitroglycerin, verapamil, diltiazem, adenosine, nipride and nitric oxide, Shroff said. One trick he uses to prevent spasm is to repeat the vasodilator cocktail with each exchange, although he admits that each operator can individualize the practice.
7. Navigate the Arm
The radial vessel can sometimes be very tortuous and even have loops (In about 10 percent or less of patients), which can make navigating the arm difficult. Shroff said he uses a 0.035-inch wire without fluoroscopy, which usually passes into the aorta easily 90 percent of the time.
If navigation is difficult, he suggests using a hydrophilic-coated wire, such as a Glidewire, for smooth, rapid movement through tortuous vessels. However, Shroff warns hydrophilic wires also have a tendency to more easily slip into side vessels and he strongly advocates use of fluoroscopy whenever using a hydrophilic-coated wire.
Also, radial artery anatomy is not symmetrical, so if an operator has difficulty gaining access or pushing the wire up the arm, Shroff suggests switching to the other arm.
8. Aortic Access
One issue commonly encountered is making the tight turn from the subclavian arteries into the aortic arch. Shroff suggests asking the patient to take a deep breath, which will elongate the aorta, making it easier to access.
Once in the ascending aorta, the catheter angle is much shallower than with femoral access, so a guide catheter needs to be braced against the wall of the aorta to help make the tight turn into the coronary arteries. Shroff said this is especially true when using right radial access, which is why left radial access is often preferred by operators first starting out. Due to the curvature of the aorta, left radial access feels more like femoral access once the operator is in the ascending aorta.
Vendors offer a selection of dedicated transradial access guiding catheters to help make coronary access easier.
Other Radial Access Information Sources on DAIC
Radial Access Adoption in the United States
VIDEO: Update on U.S. Transradial Access Adoption With Sunil Rao at TCT 2015
Radial Access May Offer Cost Savings
Patient Satisfaction and Complications of Transradial Catheterization
VIDEO: Radial Access Recovery Lounge Mimics Cafe Atmosphere
The Economic Benefits of Transradial Access
Tips When Prepping for Radial Procedures


 November 14, 2025
November 14, 2025 









