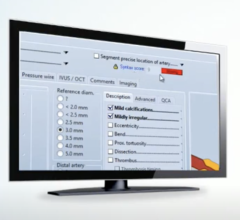
The subspecialty of electrophysiology (EP) requires patient data from a variety of sources to properly diagnose, treat and monitor patients with cardiac arrhythmias. Data sources needed for this care include procedure reports, Holter monitoring, ECGs, remote device monitoring data, office visit device interrogations, electromapping data, hemodynamics, tilt table exams and even INR blood testing results. Historically, this data has been stored in various silos of disparate IT systems within a hospital. However, several EP-specific reporting systems are now available to make all this information available in one location to speed workflow. Most are in the form of EP modules that bolt on to the larger cardiovascular information systems (CVIS) available on the market.
Due to EP’s small size and lower patient volume compared to other areas of cardiology, specialized EP reporting systems have been a more recent innovation by CVIS vendors as they attempt to include reporting for the entire department.
Having all the required EP data in one consolidated IT system avoids redundancy, saves time gathering information from separate data sources that are sometimes located in different departments, eliminates multiple logins, allows easier integration to billing, helps integrate the data with the patient's electronic medical record (EMR), allows an automated way to get reports to referring physicians, improves turn-around-times, and helps with integration to the NCDR ICD and other registries.
As with all health IT, EP reporting systems also will need to undergo major revisions in the next couple years because of new Stage 3 Meaningful Use requirements and new requirements by the Centers for Medicare and Medicaid Services (CMS) for future reimbursements.
Watch the video “IT Considerations for Electrophysiology Reporting Systems.” To help hospitals upgrade their electrophysiology (EP) reporting systems and integrate EP into cardiovascular and hospital reporting systems, Michael Mirro, M.D., FACC, medical director, cardiology/electrophysiology, Parkview Physicians Group, Ft. Wayne, Ind., offers suggestions of what to look for.
Read the article “What to Look for in Electrophysiology (EP) Reporting Systems.”
Challenges for EP IT
“The key things for EP physicians will be to know what they need to do to get reimbursement,” said Paul Varosy, M.D., associate professor, medicine-cardiology, University of Colorado, and director of cardiac electrophysiology, VA Eastern Colorado Health Care System. “Also, what do I need to do to meet new quality measures, such as required reporting to the ICD registry and other metrics.”
He explained the biggest challenge is the rapidly changing healthcare landscape due to healthcare reforms driven by the Affordable Care Act (ACA), HITECH Act and others that rely on health IT as a primary driver for change. Varosy explained these changes will ultimately culminate in a change from the current fee-for-service model to a fee-for-value model, which will all be driven by health IT systems data.
“You will need to show you meet clinical based medicine, and many in EP do not realize what is coming,” Varosy said. Unlike the mainstream subspecialty of cardiology, EP physicians are only a small fraction of cardiologists and usually operate separate from the rest of the cardiology department and they have not been as vocal or active in helping develop EP-specific IT systems.
“We need to engage with and work with our organizations like the Heart Rhythm Society (HRS) and the American College of Cardiology (ACC) and others so we are prepared for these changes,” he said. “We need to articulate what our specific needs are for these systems.”
He said some of the EP IT systems out there may have some shortcomings and not meet all of the needs of every EP department. For this reason, it is important to be involved and offer ideas to fix issues. A vendor should also be willing to help program their software to meet your needs.
The Need for Structured Reporting, Analytics and Improved Workflow
Varosy splits his time between the VA in Denver and the University of Colorado Medical Center in neighboring Aurora, so he works within two different EP reporting systems. Both systems have completely different user experiences.
The University of Colorado uses an older CVIS that pre-dates the current Web-based, modular systems now on the market. They use separate EP reporting software that sits on top of the CVIS. The hospital interfaces data from these sources and others into its Epic EMR system. During typical EP procedures, Varosy explained that patient data needs to be gathered from their GE CardioLab recording system, the hemodynamic system, EP mapping system, angiographic imaging system and echocardiography system. The workflow includes multiple logins and data from some of these systems do not interoperate, requiring data to be manually entered. EP also uses structured reporting templates, so dictation is not an option.
“It is cumbersome and painful to do,” Varosy said. “It is slow and laborious to enter the information into the system. It would be easier to dictate all this information, but we need the structured reporting, so it is a necessary evil.”
He said the structured reports help the hospital and cardiology department data mine information like procedural statistics and to monitor clinical quality control. It also is needed for mandated reporting, such as the ICD or Watchman registries.
For facilities looking for a new EP reporting system, he said structured reporting is a must, along with easy access to all the data you need to diagnose the patient and to complete procedural reports. Integration and free flow of data, especially to help auto-complete reports, are some of the points he would look for in a new system to improve workflow.
“You need to facilitate the efficient entry of all this data,” he stressed, adding that CMS reimbursements will require new data to be submitted with claims. “There is a lot that can be leveraged with technology to meet the needs of the future.”
The VA has built its own homegrown CVIS called the Clinical Assessment Reporting and Tracking (CART) system. They are still developing the EP portion of this, but the cath lab reporting has been in place for several years. Varosy said the system is a night and day difference from the other system he uses, and it significantly helps speed workflow. s a manager, he explained the analytics data CART offers is a major help measuring quality in his department. The CART system is used across the VA, so he has access to data for about 75,000 patients and about 130,000 procedures they undergo annually. The system can compare trends and measures across the country for things such as complication rates, procedural type and volumes. Varosy said this is important when you want to compare your own facility’s performance.
“We are in a very exciting moment for healthcare, but there is a mountain of work ahead of us to meet the requirements for a value-based reimbursement system in healthcare,” He said.
Lessons on Integration
Spectrum Health in Grand Rapids, Mich., needed an add-on EP reporting system, but found full integration across the health system, or even the cardiology department, was difficult to achieve.
Spectrum looked at several EP reporting systems before deciding on the Lumedx EP reporting module. It was primarily needed for documenting ablation procedures.
“We liked its ability to customize it and make it fit our facility’s needs,” said Steven Locke, MSA, information services manager, Spectrum Health. “Usually it only takes two minutes to finalize reports, due to the automated data capture of the system during the procedure.”
While the system fulfills the EP lab needs, the software has the ability for greater integration, but issues were encountered. Locke said it does not integrate with the cath lab hemodynamic system or the Provation cath reporting software. He said techs still need to manually enter any needed data into the EP system. Complicating IT matters is the fact that the vascular surgeons who also use the cath labs have their own separate reporting software. The cardiology department’s ECG management system does not interface with the EP system either, but Locke said since the software is used primarily for ablation procedures and not diagnostics, the lack of an interface has not been a big problem.
He said Spectrum Health purchased a capture module to help gather information for ICD registry submissions. However, the software is not always used and not all ICD cases are submitted. Locke said this is due to how Spectrum submits data for all registries the system participates in via a separate quality improvement department that uses its own software and the cardiology module did not meet that department’s workflow.
Spectrum also purchased a software module to capture and record implantable device interrogations and remote home device monitoring data. However, Locke said this has been held up because of integration issues due to programming issues from a primary device vendor not interfacing properly.
Spectrum currently has an older Cerner EMR, which does not fully integrate with current IT systems in all departments. It is slated for replacement by Epic in the next year, which will likely bring new integration issues with any legacy IT systems, Locke said.
Epic is one of the largest EMR vendors and is seeing rapid growth as an enterprise-wide EMR to combine patient data from all hospital departments. However, bigger is not always better, Locke said. One issue that may arise is that decisions on enterprise-wide system are increasing being made by the hospital administration, and clinicians often feel these larger systems cannot be everything to everyone, so some departments get watered down EMR versions of specialty department IT modules.
The take away message Locke has from his experience is that all stakeholders need to be at the table when new software and workflows are being considered.
“You need to have the right people who are going to manage the system and work with it every day,” Locke said. This includes not only IT, but also all of the end-users and other stakeholders who may need access to the data.
“You need to work with both the IT folks and the clinical folks, it can’t just be IT driven, or else the clinicians will require work-arounds for things that don’t fit their workflow,” he explained. “Integration with the EMR is also key."
Any software that is adopted needs to have deep clinical content, or else it will not meet the needs of the users. It also needs to integrate with legacy or other IT systems used by the department to enable a smooth workflow without the need to manually re-enter data.
“A system also needs to be able to evolve with your service line,” Locke said. When new device technologies, procedures or changes in the standard of care are adopted, the system needs to be able to adapt to these changes.
Comparison Chart of EP Reporting Systems
This article served as an introduction to a comparison chart for Electrophysiology (EP) Reporting Systems. It access this chart, go to www.dicardiology.com/comparison-charts. Access requires a login, but it is free to register and only takes a moment.
Link to GE Healthcare's Interactive, Digital Guide for Centricity Cardio Enterprise


 November 06, 2025
November 06, 2025