There are several hemostasis devices that can help cath labs improve efficiency by reducing nursing time in the recovery area, speeding the post-procedural time to patient ambulation and enabling same day percutaneous coronary interventions (PCI). There are three types of devices to aid hemostasis of arteriotomy access site punctures — vascular closure devices (VCD), compression devices and bandages coated with agents to speed the clotting cascade.
“There are devices that have an intravascular process that get trapped against the abluminal surface of the vessel and synch down like a sandwich, with a collagen plug that sits on the outside of the vessel,” said Doug Drachman, M.D., Mass General Hospital Institute of Heart, Vascular and Stroke Care. He gave presentations on how to avoid vascular access complications at the 2014 Transcatheter Cardiovascular Therapeutics (TCT) meeting. “There are others that are entirely extravascular, including ones that use a clip device, or others that insert a sort of wadded coagulant device inside the vascular arteriotomy. There are others that do not leave any prosthesis behind that just help the arteriotomy close quickly, or use a fenestrated approach, to get through the wall of the vessel and act as a trapdoor that seals when the device is removed. I think all of these devices offer opportunities for earlier ambulation time, but in meta-analysis of these devices there has not been a demonstration of lower complication rates using these devices.”
Drachman said there is still a fair amount of controversy about use of vascular closure devices, with some supporting the traditional use of manual compression only, and others advocating vascular closure devices to free up staff and speed ambulation. One of the biggest concerns regarding vascular closure devices is that some of these systems leave behind metal hardware.
“Sometimes leaving a prosthetic device behind can increase the chances of a wound infection at the access site, or in some cases, the need for vascular surgical corrective action,” Drachman said.
However, he said some patients benefit from use of vascular closure devices. “There are some patients where early ambulation is critical, as in patients with very bad lumbosacral disease who can not tolerate lying flat, or others where same day-discharge is key,” he explained.
He said closure devices cost more than manual compression, but that cost may be off-set by saving staff time or avoiding potential complications from manual compression, which may result in longer length of stay.
Rise in Radial Access
According to data from the National Cardiovascular Data Registry (NCDR), radial artery access use in the United States is now around 15 percent. One of the key reasons to use radial is to avoid access site bleeding complications.
“Transradial access really provides the opportunity, by virtue of the fact that it is a small and relatively superficial artery, to engage the vessel in a way that carries a much lower risk of bleeding or causing vascular trauma or other complications,” Drachman said.
“You have to select your patients carefully when you consider the approach, but transradial access is one method I tend to prefer and use in the majority of my patients.”
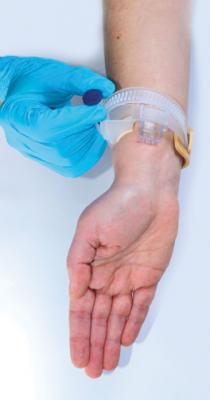
He said vascular closure devices are not suited for the radial artery, but inexpensive wristband type compression devices are commonly used to speed radial hemostasis. These are often enhanced with the use of a pad coated in hemostatic agents that promote clotting.
Advances in the Market
To expand its interventional cath lab offerings, in April Cardinal Health acquired AccessClosure Inc. for $320 million. AccessClosure’s annual sales are more than $80 million, driven by a direct sales force. The company’s Mynx family of patient-friendly vascular closure devices helps physicians seal the femoral artery using a unique, secure sealant, which dissolves within 30 days, leaving nothing behind but a healed artery. Mynx allows patients to safely ambulate more quickly, which in turn, means patients can return home sooner. In March, AccessClosure launched the Mynx Ace Vascular Closure Device, an upgraded version of the Mynx.
Biolife introduced the StatSeal Advanced Disc in August. It uses a formulation of potassium ferrate and hydrophilic polymer found in the company’s StatSeal Advanced Powder, but the disc creates an instant seal for faster hemostasis and shorter hold times following diagnostic and interventional procedures. The disc is easy to use for sheath and catheter removals and the vendor said it is more cost-effective than hemostasis pads or patches.
Cardiva Medical Inc. announced in August it closed $16.5 million in private equity financing and a $12.5 million senior secured facility with GE Capital. The company will use the proceeds to expand commercial efforts for its Vascade vascular closure system in the United States. Vascade was approved by the U.S. Food and Drug Administration (FDA) in 2013.
Last fall, Merit Medical Systems Inc. acquired Datascope Corp.’s Safeguard Pressure Assisted Device, which assists in obtaining and maintaining hemostasis after a femoral procedure and the Air-Band Radial Compression Device. The acquisition expanded Merit’s radial access and interventional portfolio.
New Trial Data
The results from the ISAR-CLOSURE trial were presented as a late breaker at the 2014 TCT meeting in September. It compared outcomes after arteriotomy closure with two different vascular closure devices to manual compression after diagnostic angiography. Data show closure devices are non-inferior to manual compression. Some meta-analyses have suggested an increased risk of vascular complications with VCD compared with manual compression, while other studies demonstrated a reduction in bleeding complications with VCD.
This trial showed after 30 days, the vascular closure device group reported access site complications in 6.9 percent of patients compared to 7.9 percent in the manual compression group. The most common complication in both groups was hematoma formation, followed by pseudoaneurysm formation. Time to hemostasis was shorter in the VCD group (median 1 minute [0.5-2] vs. 10 minutes [10-15], p<0.001), while the VCD group had a higher rate of repeat manual compressions (1.8 percent vs. 0.7 percent, p=0.003).
The multicenter, open-label clinical trial randomized 4,524 patients undergoing diagnostic coronary angiography via the common femoral artery to receive either manual compression (n=1,509) or one of two VCDs (Femoseal VCD n=1,509; Exoseal VCD n= 1,506).
The primary endpoint was vascular access site complications, including the composite of hematoma greater than or equal to
5 cm, arterio-venous fistula, pseudoaneurysm, access-site related bleeding, acute ipsilateral leg ischemia, the need for vascular surgical or interventional treatment, and local infection at 30 days after randomization. Secondary endpoints included time to hemostasis, repeat manual compression and device failure. A secondary comparison between the two VCDs was
also performed.
The secondary comparison found that the intravascular Femoseal VCD was associated with a tendency toward less vascular access-site complications as compared to the extravascular Exoseal VCD (6 percent versus 7.8 percent, p=0.043). (Due to multiple comparisons, a p-value of 0.025 was considered statistically significant.) In addition, time to hemostasis was shorter and device deployment failures were less frequent with the Femoseal VCD compared to the Exoseal VCD.
Comparison Chart
This article served as an introduction to the 2014 hemostasis management comparison charts. Listed below are the companies that participated in the chart. The chart can be accessed by clicking on the "comparison charts" tab at the top of the page.
Abbott Vascular
www.abbottvascular.com
Advanced Vascular Dynamics
www.compressar.com
Biolife
www.statseal.com
Cardinal Healthcare
www.accessclosure.com
HemCon
www.hemcon.com
St. Jude Medical
www.sjm.com
Vascular Solutions
www.vasc.com
Related Vascular Closure Content
Justifying the Use of Vascular Closure Devices
Vascular Closure Devices Show Safety Comparable to Manual Compression
Comparison Chart of Vascular Closure Devices