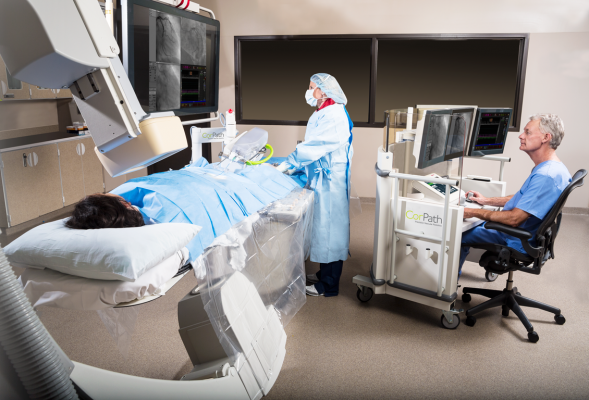
The University of Virginia Health System (UVA) installed a Corindus Corpath robotoic PCI system to help reduce the amount of radiation operators are exposed with table side during procedures.
Long-term exposure to ionizing radiation is a primary occupational concern for today's interventional cardiologists. To address these concerns, many interventional cardiologists are enlisting the support of their hospital administrators to create workplace environments that reduce exposure to ionizing radiation.
As the medical director for interventional cardiology at the University of Virginia Health System (UVA), I am proud to say that our organization is taking proactive steps to improve workplace safety for our team of interventional cardiologists and the staff working in our cardiac catheterization laboratories.
In 2014, UVA launched its "Be Safe" initiative, which is designed to make the health system the safest place in healthcare for patients and employees alike. The initiative focuses on training UVA team members to identify issues that improve safety, workflow and outcomes by increasing protection of operators in the cath lab, where risks from harmful radiation exposure and traditional protection methods continue to be a major concern.
To support the Be Safe initiative, UVA has invested in staff education and equipment purchases to create a culture that empowers all front-line staff to call out issues that affect safety, workflow and outcomes. These efforts help address many of the factors that contribute to health issues resulting from long-term exposure to ionizing radiation.
The Long-Term Impact of Radiation Exposure
In recent years, the interventional cardiology profession has paid much closer attention to the long-term health impact of exposure to ionizing radiation that is prevalent in cath labs. This focused attention is well founded, as the radiation exposure rates found in interventional cardiologists are two to 10 times higher than those experienced by other medical specialties, due to the physician's proximity to the radiation source in the cath lab.[1]
In addition, there is mounting evidence linking interventional cardiologists to a series of long-term health effects, including:
• Left-sided brain tumors [2]
• Skin cancer [3]
• Posterior subcapsular lens changes (a precursor to cataracts)[4]
• Thyroid disease [5]
• Neuro-degenerative disease [6]
Plus, more generalized adverse health effects, such as cardiovascular disease and diminishment of reproductive capacity, also may be linked to general chronic, low-dose radiation exposure.[7]
Equipment Investments
Part of our efforts to improve safety includes adding equipment to reduce radiation exposure. These include implementing imaging equipment that uses lower levels of radiation while in operation, and the addition of shields and drapes that reduce scatter radiation during procedures.
Additionally, UVA has installed CorPath robotic-assisted systems (Corindus Vascular Robotics) in two of its cath labs. The system has demonstrated a reduction in radiation exposure to the primary operator by more than 95 percent in clinical trials.[8] The CorPath system allows physicians to perform percutaneous coronary intervention (PCI) procedures from the comfort of a radiation-shielded cockpit that includes angiography and hemodynamics monitors. Physicians using the system are able to take measurements, with sub-millimeter accuracy, of relevant anatomy and well as advance or retract guide wires and/or balloon stent catheters with precise movements as small as a millimeter.
Our team of interventional cardiologists at UVA has used the robotic-assisted systems in more than 100 PCI procedures to-date, and is now exploring robotic PCI in an expanded set of highly complex cases to reduce operator radiation exposure.
Quantifying Reductions in Radiation Exposure
We are confident that our efforts at UVA are going in the right direction to improve workplace safety for our interventional cardiologists. To quantify the results of our efforts, I initiated a study in January 2015 that is evaluating the ionizing radiation exposure levels of interventional cardiologists using the CorPath system during various points of PCI procedures. Findings of the study will be published at a future date.
My hope is that the research can be used to help other interventional cardiologists — and the administrators at their organizations — have additional data to develop strategies that improve workplace safety.
Read the article, "5 Technologies to Reduce Cath Lab Radiation Exposure."
Editor’s note: Michael Ragosta, M.D., is the medical director for interventional cardiology at the University of Virginia Health System. He also is a professor of medicine/cardiology at the University of Virginia. Ragosta has been principal investigator or co-principal investigator on 10 clinical trials involving myocardial viability, coronary collateral circulation, coronary flow reserve, fractional flow reserve and myocardial contrast echocardiography. He has shared his research and experience through more than 40 invited lectures or visiting professorships and by authoring or co-authoring more than 120 peer-reviewed journal publications
References:


 May 13, 2026
May 13, 2026 









