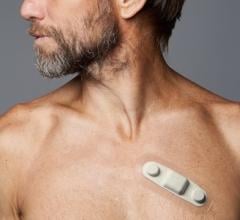
Several wearable, less-obtrusive ECG monitors have been cleared by the FDA for longer wear. This example is Cardiac Insight’s Cardea SOLO device.
When the patients of Michael Boler, M.D. need cardiac monitoring, the Holter monitor is no longer his first choice. “The newer ECG devices we have now are so much less cumbersome. It’s like wearing a Band-Aid versus carrying a bulky device,” said the Greenwood, Mississippi internist. “My patients prefer the more comfortable, wire-free form factor, and the quality is as good as, or better, than the Holter,” continued Boler. “Plus, my patient compliance has increased. With the Holter, the leads sometimes come off. The patient may think the device isn’t working, so they take it off and we have to restart the process.”
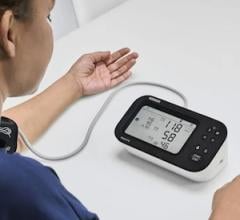
Holter ECG technology was created in the 1940s, with the ambulatory version introduced in the mid-1950s. While it gives accurate data, the device is worn around a patient’s chest or waist, with multiple electrodes adhered to the chest. The patient can’t shower or get wet while wearing it. In 2009, the first ECG patch monitor was cleared by the U.S. Food and Drug Administration (FDA). Since then, a number of less-obtrusive ECG monitors for longer wear have been approved, including Cardiac Insight’s Cardea SOLO, ScottCare novi+ Patch Holter, Biotricity Bioflux, Medicalgorithmics PocketECG, and the iRhythm Zio patch.
Extended ECG monitoring duration is an important reason why physicians are transitioning to newer ECG wearables and compact body-worn devices. Longer device wear time allows more time to capture cardiac arrhythmia events that may not present during a one- or two-day test period. Today’s ECG wearables can be worn for 7 to 14 days – and some for up to 30 days. Many studies suggest, however, that the peak diagnostic yield for arrhythmia detection occurs by about 8 days of device wear time. Wearing an ECG recording device for at least a week can significantly improve diagnostic yield compared to the traditional Holter, which is typically worn for 24 to 48 hours.
When measuring palpitations, one study documented that 24-hour Holter monitoring resulted in a diagnostic yield of 15% to 39%. In a study where patients wore both a Holter ECG for 24 hours, and a 14-day patch, the Holter recorded 61 arrhythmia events and the patch recorded 96 events. In that study, 90% of physicians felt they had a definitive diagnosis from the patch monitor, compared to 64% who felt the same way after Holter monitor usage. Also, 81% of patients preferred the patch over the Holter.
Tools in a the Cardiac Monitoring Tool Box
Cardiologist Mohammed Abuzahra, M.D., chief, division head of cardiology, Lifebridge Health, Baltimore, Md., thinks about heart monitoring devices as different tools in a tool box, and prescribes them according to patient need. “I prescribe a lot of single-channel, wearable ECG patches,” said Abuzahra. “However, if a patient has frequent PVCs (premature ventricular contractions) on an ECG, and I’m trying to quantify the number of PVCs, a multi-channel Holter test is the right way to go,” he said. Abuzahra continued that Holter ECG data can be more accurate in analyzing complex ventricular ectopy, since Holter-type devices offer a choice of three, five or seven leads, enabling multiple simultaneous views of cardiac electrical activity. With multiple leads for patients to wear, and more data to analyze, selection of the appropriate ECG monitoring device is paramount.
“Some ECG wearables use more than a single lead, but they are larger, bulkier, may have external lead wires and require more adhesive than single lead devices such as our lightweight Cardea SOLO ECG Sensor,” said Robert Odell, president and chief operating officer of Cardiac Insight. “Single channel ECG wearables are good at detecting the most commonly-occurring arrhythmias such as atrial fibrillation (AFib), among others, making them an efficient, cost-effective and patient-friendly choice for most conditions that physicians want to diagnose.”
Usage and physician acceptance of the patches is increasing, Abuzahra said. “Patients like them. Doctors like them. They’re simple to use,” he said. “With no wires, the devices are comfortable for patients and produce quality diagnostic yields. They’re especially good for patients needing a longer-term monitor, like those who might have symptoms once or twice per week. With seven days’ worth of ECG recording, that will catch it,” he said.
Like most ECG wearables, the ECG Sensor used by Abuzahra records continuously throughout the wear period, capturing every heartbeat and any abnormal activity. If the patient feels symptoms, they notate the event by pushing a button on the Sensor. After patient wear-time concludes, the great majority of wearable ECG devices require that they be returned by mail or connected to a remote, third-party ECG service center for review and processing, which can take days, or even up to a few weeks for return of results. Innovating on the status quo, Abuzahra’s practice processes its own wearable ECG device data completely onsite. The Cardiac Insight Cardea SOLO ECG System uploads and automatically analyzes Sensor data on the practice’s own Windows-based PCs, producing a draft report onsite that is ready for physician review in minutes.
With ECG wearables growing in popularity, physicians now have more choices of ambulatory ECG monitoring solutions for their office-based patients. Assuming appropriate medical indications (subject to the patient’s individual insurance plan and coverage), insurer reimbursement of prescription-based ECG wearables is widely available and should not be a barrier to adoption.
Related Wearable ECG Monitoring Content:
How Advances in Wearable Cardiac Monitors Improve the Patient and Clinician Experience
Cardea Solo Wearable ECG Collects High-altitude Cardiac Data on Denali Expedition
Cardiac Insight Partners With VivoSense for Cardiovascular Research
Wearable Cardiac Monitors Are Effective for Tracking Atrial Fibrillation Following Ablation
As Interpretation Criteria Evolve, False Positive Athlete ECG Screening Rates Can Decrease


 April 14, 2026
April 14, 2026