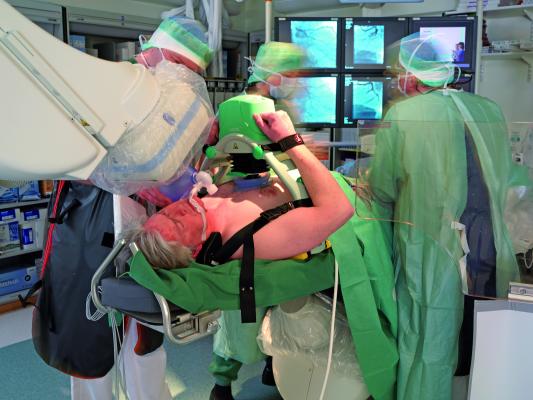
January 27, 2015 — ECRI Institute has released an updated comparison on cardiac resuscitators used during cardiopulmonary resuscitation (CPR).
Cardiac and cardiopulmonary resuscitators provide automated chest compressions and are used as a substitute for manual external cardiac compressions during CPR. They deliver a more consistent applied force and rate of compressions than manual CPR and are designed to relieve rescuers of the exhausting effort of sustained chest compressions and to free them to more effectively manage resuscitation activities.
The ECRI guidance briefly describes four units currently on the market: Michigan Instruments’ Life-Stat Model 1008 and Thumper Model 1007CC, Physio-Control’s Lucas 2 and Zoll’s AutoPulse. The report also addresses the pros and cons of manual versus automated cardiac compressions.
Types of Resuscitation Devices
There are two types of resuscitation devices: cardiac resuscitators, which provide chest compressions only; and cardiopulmonary resuscitators, which provide both chest compressions and respiratory support. Both types are designed to artificially produce blood flow in a patient during cardiac arrest. They are pneumatically or electrically driven and apply mechanical compressions cyclically to the sternum or to a wider section of the thorax, causing the heart to eject blood.
Cardiopulmonary resuscitators can also make the ratio of compression to ventilation more consistent; they use an integral pneumatic pulmonary resuscitator, typically applying time-cycled ventilation. For the purposes of this article, we refer to both types as cardiac resuscitators.
The latest American Heart Association (AHA) guidelines for CPR place greater emphasis on chest compressions and less emphasis on ventilatory support than in the past. They state that sternal compressions should be performed at a rate of at least 100 per minute, and that compression depth should be a minimum of 5 cm (2 in). Manual breaths can be used when feasible, but AHA generally recommends this only for trained rescuers. Additionally, interruptions to therapy (for example, when switching rescuers or when putting the resuscitator onto the patient) should not exceed 10 seconds. (This AHA table summarizes the key basic life-support components recommended for adults, children, and infants.)
Cardiac resuscitators are marketed to emergency medical services (EMS)/ambulance services, emergency departments (EDs), intensive care units (ICUs) and cardiac catheterization labs. They are promoted as offering the following benefits:
- Providing consistent rate and depth of chest compressions, especially compared to manual compressions delivered by fatigued clinicians or during transport. CPR may be performed for up to 30 minutes and sometimes longer; for example, one study concluded that while most survivors achieve return of spontaneous circulation early during resuscitation attempts, “some survivors were resuscitated for more than 30 min before spontaneous circulation returned” (Goldberger et al. 2012). This suggests that longer resuscitation efforts than are currently used in some situations may be appropriate, which may increase concerns about fatigue. As an indicator of how arduous manual compressions are, AHA recommends that rescuers rotate the task of compressions every two minutes.
- Allowing clinicians to perform other resuscitation activities.
- Increasing the safety of emergency medical technicians (EMTs) who can remain buckled in while attending a patient during transport.
- Allowing defibrillation to be performed without interrupting chest compressions.
- Allowing CPR to be performed in catheterization labs during imaging and stenting procedures.
Although compression devices were originally developed to help resuscitate patients during transport in ambulances, they are increasingly being used in hospitals, as evidenced by their presence in hospital-based studies. In addition, over the past five years, interest in these devices has increased by 500 percent (from 6 to 30 requests per year) from ECRI Institute’s SELECTplus member facilities.
Choosing a Unit: Focus on Ease of Use
Resuscitators should be simple to operate and require little training. When choosing a resuscitator for purchase, the first step is to request a list of several users from each manufacturer and contact them to learn their experience with ease of operation, training and maintenance.
Then, for each model you’re considering, the following points should be assessed when relevant to your needs:
- Time needed to transfer an adult patient from manual to mechanical CPR (Determine patient size limits in conjunction with this assessment)
- Ease of applying the unit on patients while the patient is on the ground and on a bed
- Ease of use on a stretcher in an ambulance
- Ease of use while loading into/out of an ambulance
- Ease of use while descending stairs
- Ease of use in the ED and in an intensive care environment
- Radiolucency of the product to gauge usability in the cardiac catheterization lab
- Ease of ventilating the patient during compressions (if resuscitator does/does not provide ventilation)
- Ease of continuing CPR while changing oxygen cylinder or rechargeable battery
For more information: www.ecri.org

 April 02, 2019
April 02, 2019 



