From left, Craig Schumacher, Jake and Yvette Honda-Schumacher. Image courtesy of Cedars-Sinai
December 16, 2022 — Yvette Honda-Schumacher was 20 weeks pregnant and had just had a routine anatomy ultrasound when she was surprised to hear that a cardiologist was asked to come into the exam room. Together with the maternal-fetal specialist overseeing the ultrasound, Myriam Almeida-Jones, MD, a fetal and pediatric cardiologist in the Smidt Heart Institute at Cedars-Sinai, explained the findings on the images.
“The cardiologist just gave me the worst possible news,” Honda-Schumacher said. Although she recalls Almeida-Jones spending time discussing every detail about the baby’s heart and the treatment he required, it was tough to process.
The first-time mom learned that her baby had four congenital heart defects collectively known as tetralogy of Fallot. One of the defects included a hole between the heart’s two pumping chambers. Her son would also be born with a narrowed pulmonary valve and narrowed arteries that would require surgical repair and the placement of stents, metal mesh tubes that keep arteries open and allow blood to circulate.
“I can remember that when I was listening to her, I wasn’t really listening to her. I was in shock,” Honda-Schumacher said. She returned to her shift as a physical therapist at Cedars-Sinai thinking about how her son would need multiple surgeries throughout childhood.
About 40,000 babies are born with a congenital heart defect every year in the United States, according to the U.S. Centers for Disease Control and Prevention. Many of these children have narrowing in one or several blood vessels that require stents. In adults, stent placement is typically permanent. Children, however, don’t have stents designed for them, so surgeons must retrofit adult stents to fit their tiny blood vessels. The stents need to be replaced as children outgrow them.
“At some point, because the stent has a fixed diameter, the child is going to need open-heart surgery to get that stent out,” said Evan Zahn, MD, director of the Guerin Family Congenital Heart Program and director of the Division of Pediatric Cardiology at the Smidt Heart Institute. “We've been waiting for a solution for decades.”
After Jake Schumacher was born in August 2018, his medical plan was put into place. Jake had frequent visits with Almeida-Jones to monitor his pulmonary stenosis and oxygen levels. He had open-heart surgery when he was 5 months old to have the hole closed in his heart and to open narrowing in his pulmonary valve and arteries. The pulmonary artery narrowing recurred, however, so when Jake turned 3, Zahn placed an adult stent into his main and left pulmonary arteries and balloon dilated his right pulmonary artery. Over time, Jake developed narrowing of his right pulmonary artery. This time, his doctors recommended a different approach.
Zahn and Almeida-Jones suggested the family wait for the launch of a clinical trial that would investigate the use of a new stent engineered to fit children.
A Grow-With-Me Stent
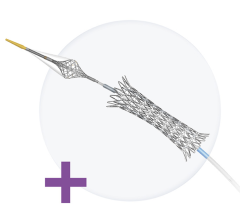
Cedars-Sinai is one of four hospitals that participated in the first clinical trial of the Minima Stent, a stent that’s being developed to grow with children. Ten children, including Jake, had these medical devices implanted as part of an early feasibility study, a type of research conducted before a larger study is planned. Investigators are continuing to study the safety of the device, as well its long-term effectiveness.
“What's beautiful about this is that it's using cutting-edge scientific discovery to address a real clinical need for our patients,” said Dor Markush, MD, assistant professor of Pediatrics and Cardiology at Cedars-Sinai and the principal investigator of the trial at Cedars-Sinai. “More studies and approval from the U.S. Food and Drug Administration are needed, however, before the device can become available for routine clinical use.”
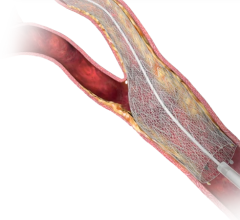
Zahn collaborated with engineers at Renata Medical to help invent the device and is now medical director of the company. The Minima Stent is made from the same metal used in adult stents, but its geometric design allows for it to expand, going from less than 2 millimeters in size to more than 18 mm. That expansion means the stent likely won’t ever need to be replaced.
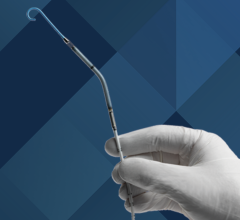
Placing the stent only takes a couple of hours through a minimally invasive procedure called cardiac catheterization, and children are expected to be able to go home the following day. Expanding it is done using the same procedure. In contrast, removing an adult stent from a child’s artery usually requires open-heart surgery, a hospital stay and several weeks of recovery.
An Active Future
Honda-Schumacher said she and her husband relied on information from Jake’s doctors and their instincts when deciding to try the experimental stents. They were attracted to an approach that would possibly mean fewer surgeries for Jake.
“It was definitely scary,” she said. “However, throughout the course of care with our doctors, we developed a lot of trust, and our doctors were always open and upfront and explained everything.”
Jake had two of the expanding stents placed in his right pulmonary artery in March 2022 when he was 3-and-a-half years old. The procedure was done on a Thursday and by Monday he was back at preschool.
Almeida-Jones, who is also associate professor of Cardiology and Pediatrics at Cedars-Sinai, predicts Jake will need to have his Minima stents expanded as he grows in approximately three to five years.
“My prognosis for Jake is that he'll live a normal life, play sports, whatever he's into,” Zahn said.
So far, Jake hasn’t wasted any time embracing what he loves: climbing, running, gymnastics, swimming and playing tennis with his mom.
“He is super energetic,” Honda-Schumacher said. “There is nothing he has been restricted from doing, which was our biggest fear, that he wouldn’t be a healthy, normal boy. I do hope other parents see this story and are hopeful.”
For more information: https://www.cedars-sinai.org/

 November 24, 2025
November 24, 2025