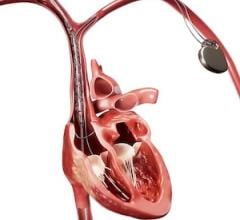
GE's ViosWorks combines 3-D cardiac anatomy, function and flow in a single, free-breathing, approximately 8 minute scan.
For decades now, magnetic resonance imaging (MRI) has been noted for its excellent soft tissue imaging capability with zero radiation dose. It has been called the imaging modality of the future over and over, but due to its complexity, long exam times and high cost, its growth has been severely limited. This especially has been the case for cardiac MRI, which only accounts for about 1 percent of all MRI exams in the United States. However, new technologies introduced at the 2015 Radiological Society of North America (RSNA) meeting in December may encourage future expansion.
Cardiac patients with chronic conditions such as congenital heart disease often require many imaging exams over their lifetime. These are generally performed using computed tomography (CT). However, CT exposes patients to ionizing radiation, and CT does not have the same contrast and ability to delineate soft tissues as MRI. Traditionally, getting a complete 3-D MRI scan of the heart would require a specialized technologist to do multiple 2-D acquisitions across several patient breath-holds, and this could make the exam take an hour or more.
Simplification and Reducing Time for Scans
GE Healthcare introduced a new MRI technology at RSNA 2015 to greatly simplify cardiac MR exams in hopes of wider adoption in the future. Developed for its new Signa MRI scanners, the new Viosworks cardiac MRI software helps automate the image sequences to perform a full 3-D chest volume scan that includes the full motion of the myocardium during the cardiac cycle, blood flow, time and fully automated quantification to create what GE calls a 7-D cardiac MRI exam. Viosworks also speeds the imaging time from about 70 minutes down to about 8-10 minutes using a single, free breathing exam at high isotropic resolution.
“We believe Viosworks can break this barrier and bring cardiovascular applications into the mainstream clinical routine,” said Ioannis Panagiotelis, chief marketing officer, MR, for GE Healthcare.
Gathering a full volume dataset of a chest in motion creates a large amount of data that would normally clog the average picture archiving and communication system (PACS) and post-processing 3-D image workstation. Viosworks 7-D MRI includes seven dimensions of information (three in space, one in time and three in velocity direction). An average cardiac MRI exam today is about 200 MB, while a Viosworks exam is an enormous 20 GB of data. A supercomputer would be required to store that much data, according to Panagiotelis, but thanks to Arterys, all of the Viosworks data is processed and stored in a HIPAA-compliant cloud in real time for increased capacity. This also provides access to the images from anywhere, including on smartphones and tablets.
GE launched a new cloud computing service in late 2015 to help process this large amount of data quickly with remote super-computing power. The use of the cloud also provides access to the images from anywhere, including on smartphones and tablets.
Simplifying MRI-Conditional Implant Scans
Advancements in medical implant technologies have greatly increased the number of patients with these devices in recent years, which complicated MRI scanning of these patients. MR-conditional implants include knee and hip replacements, spine implants, pacemakers and implantable cardioverter defibrillators (ICDs). According to Philips, data from the Millennium Research Group indicates that 12.5 million people in the United States had implants in 2015, and that number is expected to grow 71 percent by 2020, reaching to 21.6 million people.
“Today in radiology departments it’s actually very difficult to scan these patients,” said Martijn Hartjes, head of MR strategy for Philips. “You have to adapt a lot of parameters and in some cases these patients actually get turned away from an MR exam.” More and more of these devices are becoming MR-conditional, which permits MRI scanning within certain parameters.
These implants require adjustments in the scanner setup in order to create optimal images in the presence of these metal implants and to ensure patient safety. However, these adjustments can be time consuming. For example, it is difficult for clinicians to understand and scan within the safety limits defined by each implant manufacturer. These limits are not always clear or easy to implement on the MR scanner, causing patients with MR-conditional implants to often be denied MRI exams.
At RSNA 2015, Philips unveiled the first MRI automated user interface technology designed to greatly simplify exams with patients that have MR-conditional medical implants. The new ScanWise Implant software offers a guided user interface and automatic scan parameter selection designed to support “first-time-right” imaging. The software guides operators to meet the specific criteria for each implant. Hartjes said ScanWise was U.S. Food and Drug Administration (FDA) 510(k) pending as of RSNA 2015.
The findings of a recent major study led by cardiovascular imaging specialists at Allegheny General Hospital (AGH) suggest MRI is a safe and effective diagnostic procedure for patients with implantable cardiac devices. The research, believed to be the first focused solely on the value of MRI in this patient population, was presented at the annual Society of Cardiovascular MRI (SCMR) Scientific Sessions meeting in January.
“Having already established the safety of MRI for patients with these devices when performed at cardiac MRI centers with advanced capabilities, it was important to determine if significant life-saving or life-changing diagnoses could also be made based on the results of the MRI,” said Robert Biederman, M.D., medical director of the Cardiovascular MRI Center at AGH’s Cardiovascular Institute and one of the lead researchers on the study. “This ongoing study has shown that using MRI on patients with implanted pacemakers and defibrillators has added substantial clinical value to patient diagnosis and subsequent patient management, justifying the risk of the procedure. Now that we have been able to minimize the risks of MRI to patients with these implanted devices, it was crucial to prove the value of using what has really become the imaging tool of choice for countless clinical diagnoses.”
Over the last several years, AGH specialists evaluated 157 patients. That included 114 neurology/neurosurgery cases, 36 cardiovascular cases and seven musculoskeletal cases. For 88 percent of the neurology/neurosurgery cases, the MRI scan added value to the final diagnoses — with 18 percent of those cases seeing a change to the original diagnoses thanks to the use of MRI. And 92 percent of the cardiac cases saw a benefit from the use of MRI, while 100 percent of the musculoskeletal cases realized a benefit from using MRI. Additionally, Biederman reported, there were no adverse clinical events associated with it for any of the patients studied.
Under Biederman’s direction, patients with implanted cardiac devices who are referred for MRI at the hospital undergo an extensive evaluation of their cardiovascular health and level of device dependence. Once a patient is cleared to undergo MRI, Biederman and his team perform a baseline device interrogation and then convert the pacemaker and/or defibrillator to a safer mode of operation for the length of the test. If patients are determined to be non-pacemaker-dependent under baseline conditions, the device may be turned off completely while the imaging takes place, further reducing but not eliminating risk. Additionally, manipulations of the MRI environment to minimize likelihood of heating, induction of radiofrequency energy and triggering of certain potentially lethal rhythms are performed. During the procedure, a patient’s heart rhythm is monitored in real time in the MRI suite, and the entire process is closely supervised by Biederman, cardiovascular physicist Moneal Shah, M.D., and the Cardiovascular MRI Center’s team of nurses and technologists. Once the MRI is completed, the implanted device is reprogrammed to its original settings.
Image Enhancement
Rather than focusing on particular applications, some RSNA vendors chose to focus on overall image enhancement for their MRI systems. Philips, in collaboration with Dixon Technologies, debuted the mDixon scan sequence at RSNA 2015, which helps simplify and accelerate complicated scans.
“mDixon addresses one of the key challenges in MR imaging, which is fat saturation,” Hartjes said. “You want to see certain anatomies, and that’s why you want to get rid of the fat.”
Hartjes said this is typically done with sequences like SPIR (spectral pre-saturation with inversion recovery) and STIR (short-TI inversion recovery), “but what you sometimes see is that fat sat fails,” meaning the fat is not completely suppressed from the image. These types of scans can also take longer, Hartjes said. mDixon resolves both of these issues, offering complete fat suppression while actually reducing the scan time from four minutes to three minutes.
Hitachi introduced more than 40 different new MR image enhancement benefits with the release of the Evolution 5 software platform at RSNA. In cardiac MRI, it adds retrospective gating, which records more data throughout the cardiac cycle. It also adds myocardial tagging, which distinguishes myocardium displacement versus deformation. A new image-processing algorithm reduces noise while enhancing edge sharpness, and several new optimized sequences are included.
To improve magnetic resonance angiography (MRA), the Evolution 5 added selective saturation, which lets users focus on hemodynamics and isolate blood flow. Hitachi has expanded its RADAR suite for motion compensation into RADAR TOF (time-of-flight), which it calls an industry-first motion compensation MRA, and RADAR GE (gradient echo) with T2* contrast for bleeds. The software also adds arterial spin labeling (ASL) perfusion to quantify tissue blood flow. ASL is a non-invasive technique that labels the protons in the arterial blood by radiofrequency pulses, without the exogenous injection of contrast media.
Watch a video report on MRI advances from RSNA 2015.



 May 12, 2026
May 12, 2026