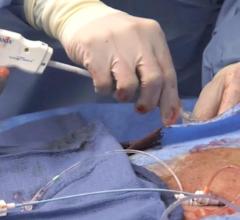
Following cath lab procedures, the final step is to attain hemostasis at the arteriotomy access site. Manual compression has been the gold standard for decades, but vascular closure devices (VCDs) can speed wound closure, and hemostatic pads can help decrease clotting times. VCDs and the new dressings also accelerate patient ambulation.
Manual compression advocates say it is less expensive than closure devices and does not leave behind foreign materials at the wound site. However, this method requires patients to sit on their backs in a hospital bed for hours, which requires additional nursing attention and may lead to additional patient discomfort.
Vascular Closure Devices
VCDs were developed in the 1990s to help control high rates of access site bleeding from compression alone. Despite improving patient outcomes, they have not been widely adopted, partly due to their higher cost as compared to compression. VCDs offer a means to improving patient comfort and decrease time to hemostasis. While vascular closure devices add costs to procedures, physicians who prefer them say the advantages include reduced nursing time and faster ambulation. Both of these factors also can help increase staff efficiency and patient throughput.
These devices offer various methods to seal the arteriotomy, including sutures, spring-clips and bioabsorbable plugs.
In 2001, about one-third of diagnostic and percutaneous coronary interventions (PCI) used a VCD. In 2006, more than 2 million VCDs were sold – about 1.6 million in the United States and 500,000 in Europe.(2)
Clinical Data Shows VCD Advantage
In 2007, a study of 12,937 patients showed fewer complications for those who received a VCD (2.4 percent) as opposed to compression alone (4.9 percent).(3)
A recent single center study of 428 patients, who received either an AngioSeal or Mynx VCD, showed similar complication rates as the 2007 study. The two devices also showed similarities in their complications, with a rate of 2.1 percent.(1) Hemostasis was achieved by the VCD followed by two to five minutes of manual pressure in all patients. Time to ambulation was two hours post-VCD placement, as compared to four hours with patients who had manual compression alone, researchers said.
Radial Compression Devices
Radial artery access through the wrist, as opposed to femoral access, is commonly used overseas. But in the United States, is usage is less than 10 percent. However, advocates of the wrist over the femoral artery are gaining numerous converts, because of the virtual elimination of bleeding complications and much faster patient ambulation. With an increasing number of radial access procedures being performed, several radial compression bracelet devices have entered the market.
Hemostatic Bandages
Several companies produce dressings that contain compounds that speed clotting and reduce the time to hemostasis. These products are generally used along with manual compression. These substances include marine organism-derived chitosan, calcium alginate from seaweed, mineral substances from clay and thrombin derived from animal sources.
The similarity of the chitosan compound used by two vendors led to a patent infringement case, which was resolved earlier this year. In April, a federal jury awarded Marine Polymer $29.4 million in its case against HemCon Medical Technologies. Both companies use a chitosan-based clotting compound in their wound dressings, but the sources of the material differ. Marine Polymer uses cultures of marine micro algae, while HemCon uses chitosan derived from shrimp shells.
Marine Polymer plans to seek accounting for HemCon’s sales in 2010 and seeks a permanent injunction to preclude further sales of HemCon’s products in the United States. HemCon has asked the U.S. Patent Office to re-examine, and possibly invalidate or limit, Marine Polymer’s patent in light of prior publications about chitosan before its patent was issued.
References:
1. Shah Azmoon, et al. “Vascular Complications after Percutaneous Coronary Intervention Following Hemostasis with the Mynx Vascular Closure Device Versus the AngioSeal Vascular Closure Device.” Journal of Invasive Cardiology, vol. 22, issue 4, April 12, 2010, pages 175-178.
2. Harold L. Dauerman, et al. “Vascular Closure Devices: The Second Decade.” Journal of the American College of Cardiology, 2007, vol. 50, pages 1617-1626
3. Nipun Arora, et al. “A Propensity Analysis of the Risk of Vascular Complications After Cardiac Catheterization Procedures With the Use of Vascular Closure Devices.” American Heart Journal. 2007, vol.153, pages: 606-611.


 October 27, 2021
October 27, 2021