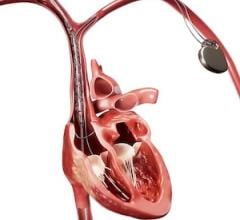
Other Nuclear Imaging Radiation Considerations:
The consensus document also lists the following safety considerations for the nuclear imaging staff:
• The photons emitted from the subject from radiopharmaceuticals are generally of higher energy than the X-rays emitted from fluoroscopy or computed tomography (CT). High-energy CT uses an energy of 140 keV. In comparison, the vast majority of Tc-99m gamma rays have an energy of around 140 keV. The photons emitted in PET from positron annihilation have an energy of 511 keV. Photons in this energy range readily penetrate the 0.5-mm lead equivalent of conventional diagnostic X-ray protective materials. Therefore, personal shielding devices, such as lead aprons or leaded glasses, are less effective and consequently are rarely used. Instead, nuclear cardiology personnel rely on the principles of time and distance. Because the total photon flux from nuclear studies is far lower than from x-ray tubes, limiting the duration spent near a radioactive subject is generally sufficient limitation of exposure. Therefore, personnel should limit the duration they spend in close proximity to either the dose syringe or the injected subject as much as reasonably possible.
• The X-ray tubes used in CT and fluoroscopy can be turned off so they do not generate X-rays, but radiopharmaceuticals are a continuous source of X-ray activity. The radioactivity also can be excreted via body fluids or spread during administration. Patient blood and excreted body fluids are radioactive and are a potential source of radiation exposure to personnel, particularly if an accident or an error causes a healthcare worker to become contaminated. Careful and routine monitoring for contamination is required. If contamination occurs, a medical physicist often needs to be involved to estimate the dose received by the worker. The reason for involving a medical physicist in cases of contamination is that monitoring devices (body dosimeters or ring badges) assume a relatively uniform dose to the person that can be accurately represented by the dose to the small dosimeter. However, a spill of radiopharmaceutical on a technologist’s shoe could result in a meaningful dose to the foot, but barely register on a dosimeter worn on a coat lapel.


 May 12, 2026
May 12, 2026