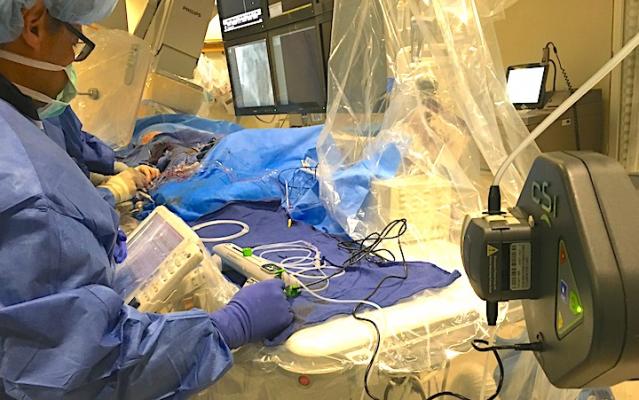
In the electrophysiology (EP) lab, hundreds of thousands of used devices are sent to reprocessors every year to get reprocessed. This practice benefits the EP lab by significantly reducing the cost of “single-use” devices, and as a result, EP procedures remain among the most profitable in the hospital.
In the cardiac cath lab, often located right across the hall, no devices are reprocessed. Yet, the potential is as great as the financial need: More focus on mapping and complex interventions with higher device costs are putting pressure on hospitals that see insufficient reimbursement for these procedures. Short term, reprocessing has the potential to reduce costs in these procedures significantly and help create a highly profitable service line.
Electrophysiology and Single-Use Device Reprocessing
Using reprocessed devices in the EP lab saves U.S. hospitals an estimated $140 million per year. This has grown since the 2000s to become a key cost savings strategy and helped hospitals make EP procedures a highly profitable service line. Some hospitals save more than $1 million per year and rely in their budgets on sustained cost savings from the practice of single-use device reprocessing.
Most EP devices are labeled “single-use.” Therefore, hospitals cannot reprocess EP devices through their central sterile department. However, registered third-party reprocessing companies can obtain FDA clearance through the 510(k) process to reprocess these devices and sell them back to EP labs at about half the price of a new device.
In the infancy of EP reprocessing, mostly low-complexity devices such as diagnostic catheters were reprocessed. However, as reprocessing companies have become more advanced and physicians more used to the devices, more complex devices have been added to the portfolio of reprocessing companies. These today include devices such as introducer sheaths, mapping catheters, diagnostic ultrasound catheters, and transseptal needles.
Reprocessing Technology and the Cath Lab
As noted, in recent years, reprocessing technology has revolutionized EP lab reprocessing, adding devices to the program that traditionally have been viewed as not reprocessable. This includes devices with a microlumen. Patented reprocessing technology today allows EP labs to utilize several reprocessed micro-lumened devices.
In the cath lab, almost all the devices used in interventions are micro-lumened. Thanks to technology advancements on the EP side, these devices could now feasibly be reprocessed without compromising patient safety or device functionality. Microcatheters, imaging catheters, thrombectomy devices, and atherectomy devices are all good candidates.
EP reprocessing has grown tremendously during the past years, with FDA clearances for very complex devices. As a result, EP labs can enjoy quite substantial savings, allowing them to:
• Reduce costs without impacting quality or physician choice
• Serve more (complex) patients
• Pay for new systems or compensate for the increasing cost of some devices
• Compensate for poor or inadequate reimbursement on some procedure types
Some of the same advantages can be realized by using reprocessing in the cath lab. However, the cath lab is very different from the EP lab in terms of procedures, devices, and costs, among other things.
Device Costs and Reimbursement in Interventional cardiology
In EP procedures, most devices cost hundreds of dollars. In the cath lab, many devices, especially those used for diagnostic procedures, are very low cost. This means that even though the total number of interventional cardiology procedures is much higher than the number of EP procedures, the cost of the average interventional cardiology procedure is much lower, and the total amount of money spent in U.S. healthcare on devices for interventional cardiology procedures is $6.9 billion versus almost $5 billion in EP.
This is because many devices are less costly, and because the most common interventional cardiology procedures – diagnostic procedures – use only the low-cost devices. A full two-thirds of interventional cardiology procedures are estimated to be diagnostic (only) procedures, with device costs between $500 and $600. Most cath labs will also conduct basic interventions with much higher costs of $3,700.
Complex interventions and procedures where chronic totally occluded vessels (CTOs) are addressed are much rarer and take place in only certain cath labs with highly skilled interventional cardiologists. However, these are also procedures with very high device costs of $9,000 to $14,000.
Therefore, the total device cost in interventional cardiology comes mainly from interventions (86 percent of the total costs). However, controlling the cost is important for both interventions and for diagnostic procedures:
Interventions: Interventional device costs are between 37 and 88 percent of CMS reimbursement. This means that it is extremely difficult for the cath lab to control the costs, especially for CTO procedures, but also for interventions in general. As more advanced (and expensive) mapping, atherectomy and thrombectomy devices are introduced, labs will come under increasing cost pressure.
Diagnostic procedures: Device costs in diagnostic procedures are fairly low, and reimbursement is ample enough to make these procedures profitable. Further, there is a downward pressure on these device prices (in contrast, the price of devices used in interventions are bound to increase). However, the sheer amount of diagnostic procedures means that overall service line revenue could be significantly impacted if device costs in diagnostic procedures were reduced.
The market for EP devices is dominated by two to three very large manufacturers. In fact, most labs are really only acquiring technology from one or two manufacturers. This gives the manufacturers enormous power in the EP lab to determine device choices, pricing, etc.
Most EP physicians are loyal to a specific brand, whether this is the brand they were trained on during their internship or because they rely on the manufacturer for knowledge and support.
In the cath lab, the situation is different. Here, there is a very large number of manufacturers, and brand loyalty and preference are much less pronounced. This means that buyers are a lot more price sensitive – and that physicians may be more willing to switch between brands based on costs.
Technology, Utilization and Cost Trends in Interventional Cardiology
The number of interventional cardiology procedures is expected to increase very minimally (1-2 percent) in the following years. However, several trends in interventional cardiology are poised to change how these procedures are done and what technologies dominate:
• Compared with EP, where technology innovation is very ambitious and new devices are introduced every 1-2 years, interventional cardiology technology has remained fairly stable for the past 15-20 years. This is certainly true for the catheters used in interventional cardiology procedures. The development of more advanced micro-catheters and interventional wires is an exception.
• There has been some pressure to ensure better accountability and effectiveness measurement for procedures in the cath lab. This has led to an increase in the use of fractional flow reserve (FFR) as well as imaging catheters. These will likely continue to be improved upon, with resulting upwards price pressure.
• Many cath labs do not conduct complex interventions, and some do not do interventions at all. This is at least partially due to the high cost of these procedures, which may not be profitable in hospitals with an unfavorable payer mix. This unfortunately means that access to life-saving interventions is not a given. This is not expected to change in the near future, due to the high costs of interventional procedure devices.
• We will likely see technology development in mapping devices as well as microcatheters. When there are price increases for advanced devices, procedure costs go up. In contrast, we are experiencing price erosion for diagnostic devices – and as a result, procedure costs go down or remain stable. This may unfortunately pressure smaller labs to stay away from complex cases.
Reprocessing Potential in Interventional Cardiology
Although there are significant differences between the economics, the technology, and the procedures of the cath lab and the EP lab, these trends suggest that reprocessing could be very valuable in the cath lab. Additionally, the development of new reprocessing technologies makes it technologically feasible to safely reprocess several devices in the cath lab for significant financial impact.
There are three reasons why single-use device reprocessing should be embraced by interventional cardiology and why it can be expected to deliver the same impact it has in EP:
1. The high volume of diagnostic procedures in the cath lab makes it critically important to control costs, even as these procedures are profitable.
2. Low reimbursement combined with increasing device costs in interventional procedures is threatening to make these procedures unattractive from a financial perspective.
3. High costs of interventional devices may prevent several labs from offering more complex procedures.
There are several possible ways of controlling device costs in the cath lab. However, single-use device reprocessing offers one with an important advantage: no need for the physician to change procedure approach or device brand.
The savings potential associated with reprocessing in the cath lab is substantial. An analysis conducted at an LA County hospital including just seven devices (a mix of high volume-low cost devices and low volume-high cost devices) showed potential savings of $87,000 per month. Savings will be different, of course, between diagnostic and interventional procedures: Cost savings in complex or CTO procedures would be $2,400, while savings in diagnostic (high volume) procedures would be less than $100.
On a national scale, it is realistic to predict that within a fairly short amount of time, single-use device reprocessing could reduce the cost of interventional cardiology procedures by hundreds of millions of dollars, with that savings translating to greater access to life-saving procedures across the board.
About the authors: Aaron DeTate is senior director of clinical integration at Innovative Health LLC. Prior to this role, he served as a clinical electrophysiology specialist and invasive cardiovascular technologist at Torrance Memorial Medical Center.
Lars Thording, Ph.D., serves as vice president of marketing and public affairs at Innovative Health LLC. He has a background in academia, consulting, and industry leadership. He has been responsible for the launch of numerous market-disrupting solutions across healthcare, insurance, and technology. Originally from Denmark, Thording has taught at universities in Denmark, Ireland, and the United States. He currently serves as the vice president of marketing and public affairs at Innovative Health, a medical device reprocessing company specializing in electrophysiology and cardiology technology. Lars currently serves on the board of the Association of Medical Device Reprocessors.
Related Catheter Reprocessing Content:
Integrating Cath and EP Lab Reprocessing With OM Technology Development
Innovative Health Receives FDA Clearance to Reprocess Pentaray Nav Eco High-density Mapping Catheter
Innovative Health Planning to Add Catheter Reprocessing for Emerging EP Technologies
Should Economic Criteria be Included in Medical Device Trials?
Use of Catheter Reprocessing to Reduce Cath and EP Lab Costs


 May 13, 2026
May 13, 2026 









