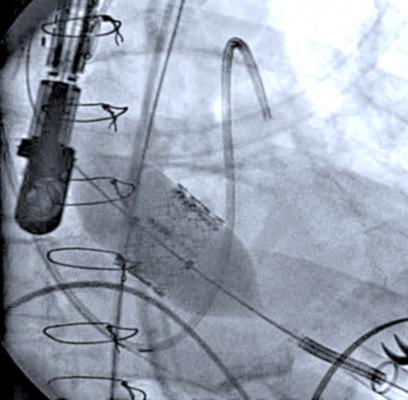
Implantation of an Edwards Lifesciences Sapien valve under angiography during the balloon inflation to expand the valve into the aortic annulus.
April 15, 2016 —The more frequently a hospital performs a transcatheter aortic valve replacement (TAVR) the better patients fare, on average, immediately after the procedure, researchers reported at the American College of Cardiology (ACC) 2016 meeting.
TAVR was first approved by the U.S. Food and Drug Administration (FDA) in 2011 to treat patients with severe aortic valve stenosis for whom standard surgical valve replacement is too risky. The valves are now being tested in trials in intermeiate- and low-risk patients.
“In a large data set of over 40,000 cases of TAVR performed in the first four years after the technology was approved by the FDA, we found that outcomes significantly improved first during the early learning phase. In addition, even after hospitals achieved a volume of 100 or so cases, there continued to be improvement in patient outcomes with higher procedure volume,” said John D. Carroll, M.D., professor of medicine and director of interventional cardiology at the University of Colorado Hospital, and lead author of the study.
Watch a video interview with Carroll on this study at ACC.16.
The findings are important because they shed light for the first time on a key factor involved in determining patient outcomes following treatment with this novel procedure, Carroll said. This will help inform decisions by health care professionals, patients and payers about how to ensure the best outcomes for patients treated with this new technology, he said.
“These results support the view that the healthcare system as a whole benefits when hospitals perform procedures in higher volumes, improving outcomes,” Carroll said.
When the FDA approved the first transcatheter aortic heart valve in November 2011, the national Transcatheter Valve Therapy (TVT) Registry was created to track patient outcomes from the use of the device. The registry, which is jointly maintained by the ACC and the Society of Thoracic Surgeons (STS), now contains data on more than 50,000 patients whose TAVR procedures were performed at nearly 400 hospitals in the United States. The database is designed to provide information that can help hospitals improve the quality of care for patients with severe aortic stenosis and help patients make informed decisions about this new form of heart valve replacement. Carroll serves on the Steering Committee of the TVT Registry.
Carroll and his colleagues analyzed data for 43,000 patients in the database whose procedures were performed between November 2011 and July 2015. Patients whose procedures were performed for different types of valves or as emergency procedures were excluded from the analysis. The researchers looked at how many procedures each hospital performed and how often four outcomes –– deaths, vascular complications, bleeding and stroke –– occurred in the hospital following a TAVR procedure.
The average death rate following the procedure, adjusted to take account of varying patient risk levels, was 4.03 percent, Carroll said. Cumulative procedure volume at U.S. centers was a median of 80 cases, ranging from a handful of cases at some hospitals to more than 600 at the highest-volume centers, he said. Most hospitals established TAVR programs in the last four years, but some were active longer due to their participation in the original clinical research trials.
“Both unadjusted and risk-adjusted mortality showed a highly statistically significant association between volume and mortality,” he said. In other words, generally speaking, performing a higher volume of TAVR procedures was associated with a lower death rate, he said. A similar association was seen for vascular and bleeding complications but not for stroke, which occurred at 2 percent.
The study has a number of limitations. First, the association of better outcomes with higher volume does not prove causality. The analysis attempted to control for other factors that could affect patient outcomes, such as differences in patient characteristics and the subsequent introduction of new valve technologies, but Carroll said these adjustments are not perfect. Second, the “early learning curve” could not be separated from the subsequent period that is commonly used to study the volume-outcome relationship. During the nearly four-year study period, the number of hospitals performing TAVR increased rapidly, and FDA-approved indications for the procedure expanded to include patients who could have surgery but were at high risk for serious complications or death from open-heart surgery, as well as those not eligible for conventional surgery. Furthermore, the technology itself was evolving, with several new models of the device coming onto the market while the study was underway.
“These findings are a first look at how procedure volume influences outcomes for a recently introduced technology,” Carroll said.
Although procedure volume is important, volume is not a direct measure of quality, he said.
“The bottom line is not volume but the actual outcomes achieved at a center,” Carroll said. “In general, outcomes at U.S. centers are excellent. Furthermore, there are some lower-volume centers that have excellent outcomes and some higher-volume centers that do not have the best outcomes.”
The TVT Registry provides quarterly reports to all participating hospitals, providing their results benchmarked against national averages. A major goal of the registry is to provide feedback to centers so they can continue to improve outcomes, Carroll said.
Currently, TAVR can be performed only at hospitals that meet qualifications laid out by the federal Centers for Medicare and Medicaid Services (CMS). A major question for CMS and professional societies, Carroll said, is whether to keep or revise these qualifications. The present study provides data and analysis that can help inform these decisions, he said. At the same time, rapid growth in the number of hospitals offering TAVR means that the vast majority of U.S. patients are reasonably close to more than one center that meets the CMS qualifications for providing TAVR, he explained.
Researchers said further studies are also planned that use other methods to analyze the relationship between volume and outcomes, follow patients after discharge from the hospital, and assess how patient outcomes are affected as hospitals gain more experience with TAVR and the technology is refined over time.
The study was supported by the American College of Cardiology and the Society of Thoracic Surgeons.


 April 02, 2026
April 02, 2026 









