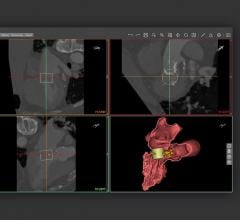
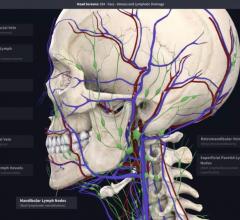
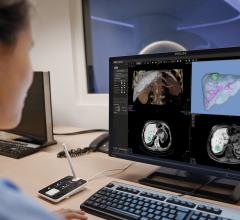
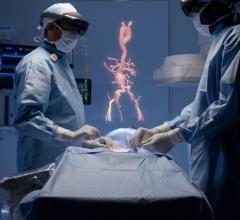
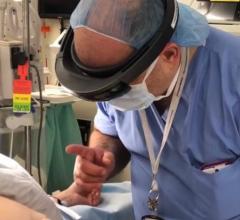
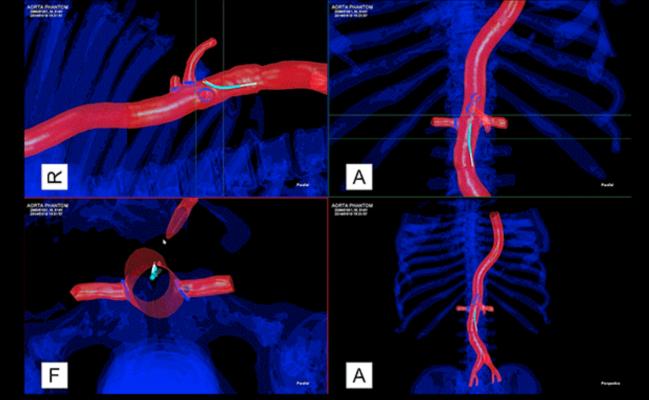
As interventional procedures become more complex, one of the biggest issues is the ability of operators to see the devices they are using in the soft tissue anatomy that is mostly invisible under 2-D fluoroscopy. Several companies have developed new navigation aids, including multimodality fusion imaging software from Philips, GE and Siemens. This image shows a new system being developed by Centerline Biomedical. There is a more detailed image below.
When Andreas Grüntzig, father of percutaneous transluminal coronary angioplasty, approached his cardiac surgeon colleague Åke Senning for support in applying newly-developed angioplastic techniques to the coronary arteries, Dr. Senning enthusiastically responded, “You will take away my patients, but get started!” Senning foresaw what Grüntzig was setting in motion — the development of the discipline of interventional cardiology, destined to become a field of practice positioned to bring lifesaving therapies to patients whose bodies struggle to recover from the traumatic insult of open surgery.
Indeed, today image-guided interventions have become the treatment of choice for a broad range of diagnoses, thanks to their minimally-invasive nature. But even with the success achieved with widespread dissemination of these technologies and techniques, there remains significant opportunity to improve technology and techniques, to access and treat more patients, and to do so more safely and with even greater clinical success.
Improving Soft Tissue Visualization
Today’s cath lab or hybrid suite faces some challenges that innovators are hard at work to address. The ability to visualize soft tissue and to appreciate complex three-dimensional structures with a fundamentally two-dimensional X-ray-based imaging modality still leaves something to be desired. The exposure to ionizing radiation is now known to represent an occupational hazard to interventionalists, carrying radiation-related risks including an elevated cancer rate. And there yet remain many types of surgical procedures that have no commonly available minimally-invasive counterpart, although conceptually an interventional approach is possible.
Nascent solutions have appeared, many reflecting trends in the latest in computational and electromechanical technology. And while these first-movers have made a significant impact, we have now advanced to an even more rapid pace of innovation, as access to engineering and design necessities has exploded. Building blocks are increasingly available to those with the concepts, understanding, and ability to execute.
Computational power and high volumes of data storage are widely available in cloud-based form at reasonable monthly rates. Google provides machine learning services online. Three-dimentional hubs allows anyone access to 3-D printing for quickly prototyping new inventions. And network infrastructure interconnectedness allows collaboration between innovators around the world.
As a result, we are at a tipping point after which we will see our cath labs and hybrid suites become more and more technologically sophisticated at an increasing rate. The independent components of predictive analytics, interventional robotics and advanced imaging will converge, and provide clinicians with immensely powerful tools.
Predictive Analytics
Predictive analytics allow the mining of vast amounts of data to extract information and patterns which can provide valuable guidance to clinicians. One reason that the highest-volume practitioners are also the highest-performing is that they are able to draw upon the greatest pools of experiential knowledge. Analytics will allow us to spread this wealth. The widespread use of electronic medical records (EMRs) has set the stage for this type of technology, the most significant remaining piece is to encode data regarding anatomy. The development of technologies capable of transforming imaging data into models suitable for computerized analysis will close this gap and allow computational systems to provide valuable clinical decision support. As an example, research directed by Partho Sengupta, M.D., has already shown improved workflow efficiency leveraging machine learning to assist in interpretation of echocardiograms.[1,2]
The about Sanguta’s presentation on this topic at the American College of cardiology 2019 meeting in the article “How Machine Learning Empowers Echo Users Today.“ Or, listen to a PODCAST with Sangupta “How Technology Is Changing Cardiology.”
Robots in the Cath Lab
Surgical and interventional robotic systems have already made a significant impact. Just as the Intuitive Surgical da Vinci system has facilitated minimally-invasive therapies which previously could only be done invasively, the Hansen Magellan and Corindus systems have demonstrated the capability to perform interventional procedures with vastly decreased operator radiation exposure. They are joined by startup companies like Restore Surgical who are developing more compact, cost-effective, and workflow-compatible robotic solutions.
We are now at the verge of expanding these technologies and truly realizing robot-assisted procedures, in which clinicians are given mechanical and navigational tools which allow certain actions or portions of the procedure to be performed autonomously, with a level of control only possible with robotics.
Reducing Use of X-ray Image Navigation
Advanced forms of imaging with reduced dependence on ionizing radiation are becoming increasingly available. Navigation technologies like the Abbott MediGuide and Johnson & Johnson Carto leverage electromagnetic tracking, allowing improved 3-D visualization while also reducing dependence on fluoroscopy. Philips Medical recently completed a clinical study evaluating their Fiber Optic RealShape technology used to navigate interventional instruments using fiber optics. Startup companies including Centerline Biomedical, of which I am CTO, are expanding the reach of electromagnetic tracking to a wider range of vascular interventions as well as bridging the gap to these other interventional innovations.
Each of these areas of technological innovation stands to benefit from the others. Advanced imaging combined with robotic control will provide increasingly precise image guidance as well as increasingly precise interventional control. Predictive analytics will allow machine learning algorithms to provide optimal robotic navigation, and to augment imaging with the most clinically relevant and useful additional information.
Tomorrow’s cath lab will see an integration of today’s most advanced technologies, and the result will be much more than the sum of its parts. This will facilitate continued growth of the capabilities and reach of catheter-based interventional therapies, allowing a greater patient population to be treated with greater success. It will empower clinicians to make the best possible decisions for patients and to protect themselves and their patients from undesired exposure to radiation in imaging. Especially as we see advances in interventional structural heart therapies, complex percutaneous coronary interventions, and endovascular aortic repair (EVAR), this synergy will create value for clinicians, patients, and the healthcare system alike.
Editor’s Note: Vikash Goel, MS, is chief technology officer of Centerline Biomedical Inc. The company is developing next-generation imaging and precise real-time 3-D navigation to empower physicians with solutions designed to improve outcomes, lower costs, simplify complex procedures, and reduce radiation exposure to patients, clinicians and caregivers in minimally invasive endovascular procedures. The company was founded in 2014 as a spinoff of Cleveland Clinic.

 May 12, 2020
May 12, 2020