
In the past decade there has been a proliferation of clinical-grade wearable monitors and implantable devices such as pacemakers, ICDs, implantable cardiac monitors, and new pacemaker-like devices that can control hypertension. In the near future, these devices will be tied into a body-wide internet of things for specific patients that can transmit patient data to clinicians wirelessly to enable an integrated, more robust form of telecardiology and telemedicine.
Cardiovascular diseases are among the leading causes of death for people over 65 years old in North America and Europe. According to a report by the World Health Organization (WHO) on the top 10 causes of death in 2019, heart disease remained at the top of the list. The world’s aging population has resulted in an even greater surge in health problems. These increasing health problems cause many challenges, including a lack of timely treatment due to limited resources (hospital beds, monitoring devices, and healthcare personnel), as well as disposable funds to meet these healthcare expenses.
One of the primary cardiovascular diseases is cardiac arrhythmia caused by premature ventricular contractions (PVC) and premature atrial contractions (PAC). Another common heart anomaly is myocardial infarction, which results from the narrowing of the arteries that supply blood to the heart. Because of this, detecting the early signs of these cardiac anomalies is crucial for efficient treatment for cardiac complications. Ideally, the symptoms of the standard cardiac conditions are monitored using an electrocardiogram (ECG) to measure the contraction and relaxation patterns of the cardiac muscles that are made up of myocardial cells, which are electrically depolarized and re-polarized.
Patients that have survived heart attacks or have underlying cardiovascular problems require implanted devices. Millions of people a year receive implantable devices such as pacemakers, implantable cardioverter defibrillators (ICDs), and left ventricular assist devices (LVADs). In earlier times, patients would periodically have their data downloaded from these devices at healthcare centers to analyze further or maintain patient health records. Also, these implantable devices required testing for battery health status, impedance and sensing thresholds in periodic intervals throughout the year.
In recent years, there has been a surge in the number of devices used for heart failure and other cardiovascular treatment. With optimism about these devices from experts, several advancements in treating cardiovascular diseases with such devices has occurred over the years. For example, pacemakers, small implantable devices designed to be placed under the skin of the chest, have helped millions of people worldwide continue to live normally after developing heart arrhythmias, with electrical impulses in the pacemakers controlling the pace of the heartbeat.
New and innovative technologies have led to the development of intelligent sensors for pacemakers, that permit real-time monitoring of patients. Such devices enable re-synchronization upon the detection of cardiac anomalies. Moreover, using an app, these devices can transmit patient data to a physician in real-time. Recently, the FDA has approved highly advanced pacemakers such as cardiac re-synchronization therapy (CRT) pacemakers. Several features, such as smaller sizes, remote monitoring capabilities, faster responsive rates, and a notable improvement in battery longevity of modern implantable pacemakers have resulted in wide acceptance from industry experts and physicians. Wireless Body Area Networks (WBANs) have made real-time monitoring of patients possible, including monitoring potential faults in wireless communications and ensuring safety.
What is a WBAN and How is it Used in Cardiac Monitoring and Therapeutics?
A wireless body area network (WBAN) consists of wearable or implanted devices or sensors that are used for monitoring and logging vital parameters of patients. Rapid technological advancements in low power integrated circuits and high throughput wireless communication networks have made WBANs possible. Each device on the network is called a node, that can transmit real-time data of patients' measurable physiological functions to a healthcare centre. WBANs can operate autonomously to connect multiple medical sensors and devices connected to or implanted in a human body.
For cardiology, WBANs offer cost-effective solutions for real-time monitoring of temperature, blood pressure, heart rate, ECG, and respiration, which can provide further insight into a person’s health. The advantage of WBANs extends further as patients don't need to remain in the hospital for constant monitoring. Such benefits improve the patient’s quality of life while significantly reducing healthcare expenses. In addition, patient data collected from the device provides valuable insight on the prognosis of a patient's condition in a natural environment for a more extended period, which is essential for accurate and faster diagnosis. WBAN solutions are promising and are likely to revolutionize how health care services are utilized and delivered. Figure 1 provides an overview of the WBAN architecture.
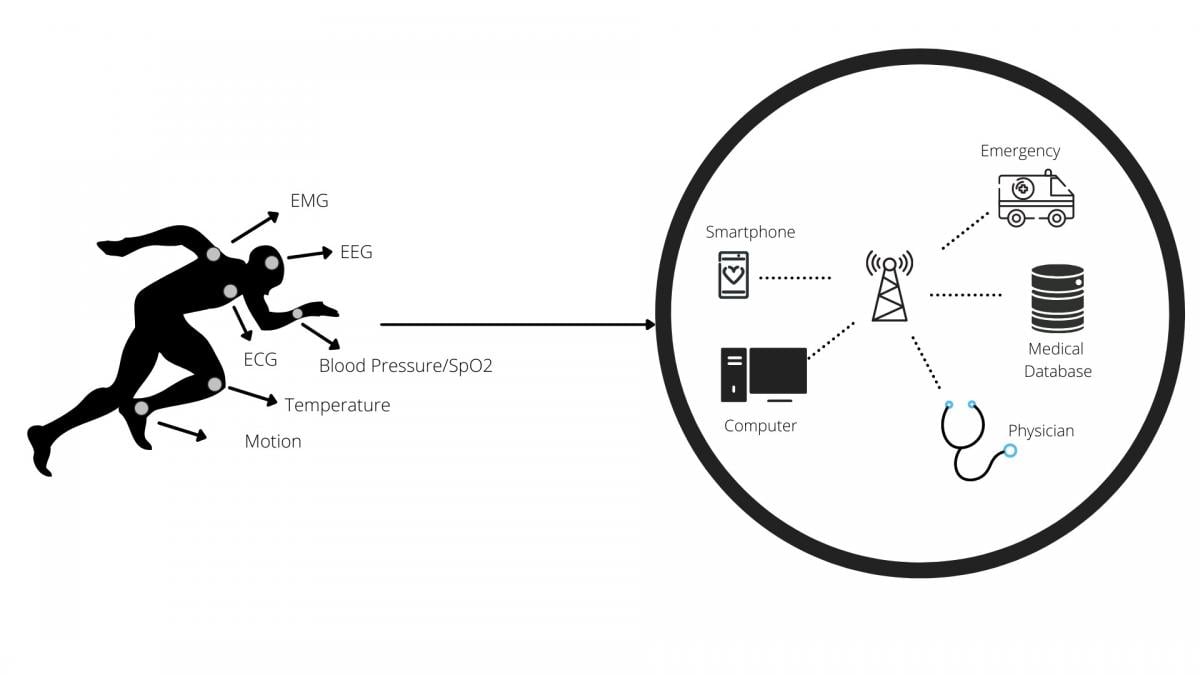
Figure 1. An overview illustration of Wireless Body Area Networks (WBAN) architecture where implantable and wearable medical devices can create their own internet of things (IoT) to wirelessly communicate date back to a central monitor or alert clinicians if there is a problem. This could represent a new approach to remote monitoring and telemedicine.
WBANs connect nodes such as sensors or actuators situated over the human body, including those under the skin, through a wireless communication channel. Generally, WBANs are known to be application-dependent, and classified into two different types: single event detection and periodic event detection. In the first type, nodes send data at the occurrence of an event (e.g., when a patient has a heart attack), while in the second type, the nodes send data at periodic intervals (e.g., sending blood pressure measures or heartbeat). Technical evolution has led to advances in high-throughput wireless data communications, thereby allowing for real-time streaming of WBAN device data. WBANs can monitor data using AI statistical classification techniques (e.g., real-time Bayesian networks and spport vector machines) to detect in patients cardiac anomalies such as PVC, PAC, and MI and to alert physicians before any critical scenario occurs.
WBANs are also helpful in monitoring the functionalities of implantable cardiac devices (e.g., implantable cardioverter defibrillators ICDs and pacemakers). Typically, WBAN is classified as per the operations - devices implanted inside the human body and wearable devices that work on the surface of the human body. Wearable devices monitor the activity changes in the surrounding environment with crucial feedback to maintain the optimum status. For example, ECG, EEG, and blood pressure monitoring to monitor patient's in a critical state.
Several modern ICDs, pacemakers, and LVADs have incorporated Bluetooth technologies to pair devices for communication with healthcare centers for assessing the sensors. Many leading technologies are focused on developing medical sensor systems with low power consumption and seamless data transmission. WBANs are vital for such tasks as it acts as the transceiver for transmitting the signals of an ICD and ensuring reliability during data transmission of essential health data of a patient such as pulse reports and relevant cardiac functionalities. Another significant advantage of WBANs is the compatibility with several wireless technologies for medical monitoring systems like WLAN, WiFi, GSM, 3G, 4G, WPAN, and WMTS.
Transferring highly sensitive medical data requires all forms of WBANs to maintain the privacy and authenticity of data, as well as being very robust. To build robust WBANs requires a failsafe system design, meaning the availability of backup node devices in case of failure of one device.
Interoperability is necessary for wireless medical sensors and devices, as it can provide greater accessibility for a WBAN through various radio protocols For example, if patients are mobile, a WBAN device could use GSM or Wi-Fi as a network gateway to transmit data to the healthcare centre.
A common concern observed with wireless networks is the dependence on hardware, thereby limiting reprogramming possibilities. Different devices require different radio transmission protocol stacks (i.e., sensor layer, communication layer, application layer, data layer, and user layer). Software-Defined Radio (SDR) solves many problems related to the hardware and offers several more benefits. SDRs are flexible, reprogrammable with various protocol stacks. They simplify merging with other software to provide features like interference detection, efficiency in frequency distribution, test repeater operations, and measurement of a parameter such as identifying spectrum intruders and noise characterization. SDRs can help in several stages, from prototyping to deploying WBAN devices, and allow for testing new protocols, filters, AI algorithms, and error correction using an FPGA. SDRs also provide real-time monitoring and storage solutions for a vast network of nodes (sensors/devices) on WBAN due to high data throughput.
SDR technology has gained a strong foothold with several utilizations in radio environments, and is witnessing widespread use of the technology for building innovations suitable for healthcare domains. With current trends, it is highly likely for a high performance SDR to be central to a WBAN and provide more accessibility for healthcare providers to track and monitor patients using WBAN sensor nodes. SDRs have become more reliable and can meet the most demanding requirements, with high performance, instantaneous bandwidth, custom channels, data backhaul, and an FPGA SoC. Importantly, SDRs have interference detection capabilities, and can be programmed on the FPGA to recognize if a device on WBAN is not transmitting or functioning correctly. Figure 2 depicts a high-performance SDR capable of real-time monitoring and storing data of several devices simultaneously.

Figure 2 depicts a high-performance software-defined radio (SDR) capable of real-time monitoring and storing data of several devices simultaneously. This type of device can enable Wireless Body Area Networks (WBAN) with an array of implantable and/or wearable medical devices on a patient.
Benefits and Drawbacks of WBANs
Benefits of WBANs to the patient:
• Patients can be monitored remotely while away from a hospital.
• Data acquired over an extended period is from a patient's natural environment, which provides more significant insight into epidemiological studies, prognosis, and maintaining accurate health data records of patients.
• WBANs are cost-effective solutions that reduce the financial burden on patients while improving the safety and quality of care.
Benefits of WBANs for Healthcare Providers
• Healthcare providers can offer affordable healthcare solutions with reduced costs for in-patient care.
• The cardiac data can be collected and can be used to train AI algorithms for detecting heart arrhythmia.
• Fewer frequent visits to doctors to download data on the device or check the devices' functionality.
• A reduced burden on healthcare providers, as data collection, monitoring, and storing data is automated.
Drawbacks of WBANs to Patients
• As with most advanced technologies, security and data confidentiality remain a challenge. The possibility of jeopardized network security and illicit accessing of sensitive health records of patients is a key issues to address.
• The transmission from devices via GSM/cellular services to the healthcare center may not work correctly if there is weak connectivity or no service in the patient's area.
Drawbacks of WBANs to Healthcare Centers/ Providers:
• The clinics associated with remote monitoring of patients will require a substantial amount of initial investment for setting up the infrastructure such as servers, transceivers, and storage solutions.
• The devices/sensors must have powerful communication abilities despite hardware constraints such as unreliable network links, limited energy reserves, and interference. These limitations may provoke incorrect transmission of data.
• The requirements for a large number of sensor nodes must coexist within the limited space in the hospital.
Emergence of SDRs Enhances the Capabilities of WBANs With Increased Accessibility for Monitoring Services
WBAN is an emerging technology capable of transforming how healthcare services are offered. The emergence of SDRs enhances the capabilities of WBANs with increased accessibility for healthcare monitoring services. As these technologies in communications are integrated into conventional medical systems, it gradually boosts patient health status analysis and monitoring efficiency. WBANs and SDRs require reliable and high-performance industry solutions for these technologies. Given the potential, it is evident that they are becoming the key contributors towards a technology that is reshaping affordable and mobile healthcare services.
About the author: Victor Wollesen is the CEO of Per Vices, a RF and digital systems innovator supplying multiple industries with wireless communication solutions. The vendor develops and deploys high performance software defined radio platforms with the highest bandwidth and customer focused designs, to support a wide variety of applications within defense, civil, aerospace, medical, telecommunications, low latency networks, global positioning (gnss/gps), radar, spectrum monitoring, and broadcasting and wireless management industries. For more information: www.pervices.com


 March 04, 2026
March 04, 2026 









