
(Editor’s note: This is the first part of a two-part series on the proposed Medicare five-year demonstration for mandatory bundled payment system. Part 1 outlines the baseline capability requirements. Part 2 presents a model methodology for developing a successful cardiac bundle the payment model as it applies to cardiac patients.)
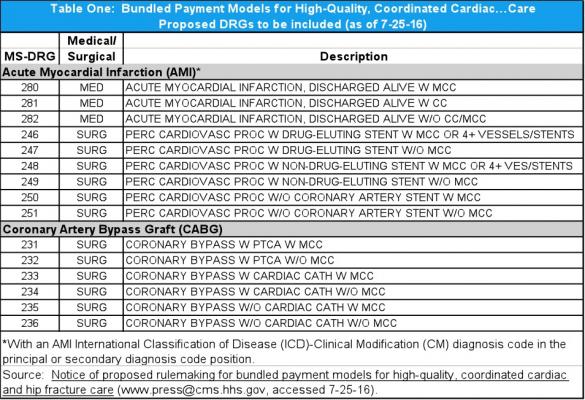
The movement away from traditional Medicare fee-for-service reimbursement and into bundled payment models by the Department of Health and Human Services (HHS) will include heart attack patients effective July 1, 2017 (see Table 1). This includes patients with myocardial infarction who undergo percutaneous coronary intervention (PCI) with or without stenting and coronary bypass graft surgery.
The Centers for Medicare and Medicaid Innovation (CMMI) is currently seeking comment on the five-year demonstration, which would include 98 (of 381) randomly selected metropolitan statistical areas (MSA). The July announcement is part of the HHS push to expand its existing bundled-payment projects in an effort to move the Centers for Medicare and Medicaid Services (CMS) from fee-for-service to alternative payment models. The goal is to pay for high-quality, coordinated care and achieve a 50 percent penetration rate with these new models by 2018. According to the CMMI notice, “These models would reward hospitals that work together with physicians and other providers to avoid complications, prevent hospital readmissions and speed recovery.”
This move may signal the beginning of the end of traditional CMS reimbursement for cardiac patients and the dawn of a new era of increased financial and organizational challenges for hospital cardiovascular programs.
Read the article “Societies Comment on New CMS Bundled Payments for Cardiology.”
How the Model is Intended to Function
Under the proposal, a hospital in which a patient is admitted for care for a heart attack or bypass graft surgery would be accountable for the cost and quality of the care provided to Medicare fee-for-service beneficiaries during their inpatient stay and 90 days post-discharge. Once the model is in full effect:
• Hospitals would be paid a fixed target price per episode, with hospitals that deliver higher-quality care receiving a higher target price.
• At the end of a model year, the actual spending for the episode of care (Medicare parts A and B only) would be compared to the targeted price that reflects the quality outcomes for the individual hospital.
• Hospitals and physicians that provided needed care for less than the quality-adjusted target price, while meeting or exceeding quality standards, would be paid the savings achieved; hospitals that did not meet these standards would be required to repay Medicare the difference.
Each year CMS will set the target prices for different episodes of care based on a blend of regional historical data and hospital-specific data on total costs for Medicare fee-for-service patients admitted for heart attack and bypass surgery – from hospitalization through 90-days post-discharge. Target prices will be “adjusted based on the complexity of treating a heart attack or providing bypass surgery.” The target prices will be blended from hospital specific data and regional historical data, starting with the first year (July 2017 to December 2018) at two-thirds participant-specific data and one-third regional data, to the last year of the demonstration (2020 to 2021) with only regional data.
Paying for High Quality Care
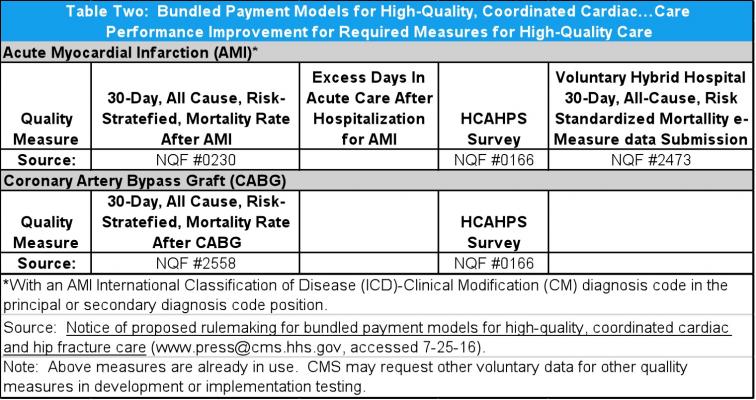
Under the proposal, hospitals that produce higher quality outcomes would be paid more than those that did not. For example, an individual hospital quality-adjusted target price would be based on a 1.5 to 3 percent discount rate relative to historical spending – with the lowest discount percentage going to those hospitals providing the highest-quality care. The quality metrics used would be measures already in use in other Medicare programs. For example, for bypass surgery, measures would include hospital 30-day, all cause, risk-stratified mortality rates as well as Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) survey results (see Table 2). The HCAHPS patient satisfaction survey is required by CMS for all hospitals in the United States.
Implementation of the Model
The program will be phased in according to a proposed schedule. Possible repayment to Medicare (the downside risk) would include no repayment the first year, capped at 5 percent the second year, capped at 10 percent the third year, and ultimately capped at 20 percent the fourth and fifth year. Possible payment from CMS to hospitals (the upside reward) would include possible payment capped at 5 percent for the first two years, 10 percent the third year, and capped at 20 percent the fourth and fifth years. The program is intended to start July 1, 2017 and run through 2021. There is no application process. Hospital payments under the model would be reconciled on a periodic, scheduled basis. Rural hospitals are exempt.
Once the program is complete in 2021, HHS will evaluate the results and make recommendations for continuance, modifications and/or expansion. The results of previous bundled payment experiments have shown strong potential to improve patient care while reducing costs; therefore, there is no reason to believe that Medicare bundled payments will not be expanded in the future or that private payers will not increasingly adopt this new model.
Of note is the fact that Medicare has also proposed a new incentive program aimed at acknowledging the importance of cardiac rehabilitation to overall patient recovery.
Implications for Hospitals
The implications of mandatory bundling are significant for most cardiac programs, particularly cardiac surgical programs. In preparation, every cardiac hospital should perform two basic calculations and analyze the results:
1. Compare its historical spending to its regional MSA average spending for targeted Medicare severity-diagnosis related group (MS-DRG). Assuming all other factors are equal, if spending exceeds the regional average, there is a potential for penalties. If spending is below the regional average, there is a potential for additional reimbursement.
2. Compare the existing quality metrics appropriate to each episode of care using performance and improvement on required National Quality Forum measures that are already in use with national benchmarks. Individual hospital performance could translate into a 1.5 to 3 percent discount rate relative to historical spending.
An analysis of the answers to the above questions, even on a preliminary basis, will allow the hospital to assess its historical position and hopefully, create an incentive to systematically prepare for new financial models including upcoming bundles.
Bundled Pricing Baseline Capabilities
Designing and implementing bundled pricing is not easy, but it will be increasingly necessary as Medicare and (ultimately) private payers move away from fee-for-service reimbursement and the payer marketplace continues to evolve. It is tempting to see bundling as focusing largely on pricing. However, there is much more involved that if not done properly can have significant financial and operational consequences beyond simply offering a competitive price. Assuming that there will continue to be an active market for cardiac bundles, hospital and health system preparations need to focus on the following 10 broad baseline issues and required capabilities:
1. Administrative Support — Bundles cannot be designed or implemented without a commitment to the concept, the required process and the need to plan – and potentially augment – existing resources to support the effort. This commitment may require new organizational structures, reporting relationships, care and business philosophies, and specialized manpower, as well as technology and infrastructure (including electronic medical records, specialized clinical databases or registries, and the optimization of cardiovascular information systems).
2. Physician Support is Critical — Standardization and care coordination processes are driven by physician and other practitioner leadership, planning and active participation. Physicians must provide necessary clinical leadership and actively support efforts to re-engineer care, streamline processes, boost quality outcomes and manage performance metrics, all under an appropriate hospital/physician alignment model that properly incentivizes participants. Note that the proposed CMS bundles do not directly include physician compensation, making it easier to develop a bundled price without negotiating for the inclusion of physician compensation. But, it potentially makes things more problematic, as physicians have less incentive to lower hospital costs through modification of their own clinical practices if their reimbursement is excluded from the bundle.
3. Information Drives the Process — Identifying patients, defining costs, setting prices, monitoring quality, identifying risks and complications, and managing these elements over time will make or break any bundle. These critical components will require timely and comprehensive information. Sophisticated hospital costing systems still lag behind other industries. Hospitals will need to address Medicare’s targeted MS-DRGs or analyze other patient MS-DRGs for specific bundling potential, allowing for clinical and cost variances. They also need to match potential bundles with outcomes and understand the circumstances that lead to variability in cost, length of stay, resource consumption, discharge to a post-acute care provider (PAC) and other factors to control the means of production. Clinically sophisticated risk stratification models will need to be applied and ongoing care carefully monitored to prevent complications, readmissions, etc.
4. Standardization — The creation of best practice protocols, clinical pathways and guidelines of treatment are important underpinnings to bundles, as they define the standard of practice, coordinate clinical input and serve as the basis for cost analyses and ultimately pricing decisions. Driving out “unnecessary” variation leads to predictability, enhances quality, and solidifies physician and other practitioner commitment to the process required to produce a predictable “product.” Note that this clinical standardization will have to go beyond the hospital stay and cover 90-days post-discharge. This means that hospitals will have to work closely with PAC providers (particularly home health and skilled nursing), incorporating their own protocols and guidelines into the overall plan of care.
5. Care Coordination — With clinical, outcome, financial and other performance standards in place, care coordination across the continuum (potentially involving multiple facilities and organizations not owned by the hospital) will be paramount. Many hospitals are now selecting home care and PAC providers they can work with and incentivize as part of a network to support bundling. Coordination could include patient education, scheduling, transition planning and other activities to ensure smooth and faultless transitions. Care coordination must be incorporated into standardization activities that produce clinical protocols and guidelines and account for the risk-stratification of each patient under care.
6. Supply or Value-Chain Management — Beyond high-quality and coordinated care, competing on price and other appropriate clinical metrics will force hospitals to reconsider their supply (or “value-chain”) processes to continually tailor supply chain, procurement, physician-preference items, and vendor and product selection, as well as refining value analysis processes to increase the cost-quality-value philosophy.
7. Re-Engineered Business Systems — An often neglected capability involves the business systems necessary to produce and process appropriate billings for payers who bundle. Medicare billing under the proposed bundle is straight forward: one bills as usual and reimbursement is recalculated automatically on a scheduled basis. However, as bundling expands, billing for a bundle is not like generating a bill in the past — it requires carefully re-engineering the process to reflect patient identification, guaranteed prices per admit, subcontracts to other providers, included physician compensation, etc. Careful planning and resource allocation is required to keep the revenue stream both current and accurate.
8. Bundles vs. Episodes of Care — An episode of care and its matching billing historically stopped at the time of hospital discharge. Now it may involve multiple organizations (think home care and skilled nursing at the least) that will need to be coordinated, contracted and managed into an overall care process. Relationships will need to be set in place and properly managed to optimize care coordination and patient transition.
9. Constant Clinical Innovation — Bundles are not static, nor is the ongoing feedback on performance against internal or external benchmarks and metrics. Processes need to be in place to constantly monitor all of the care processes and performance indicators and innovation applied when necessary to make periodic adjustments. Systems and personnel must be in place to both monitor and innovate when required.
10. Marketing and Sales — While some market opportunities will come to the hospital, it is incumbent upon them to continually monitor the payer marketplace and develop bundles that are appropriate and will be well received by payers. Direct hospital-to-business bundle offerings are becoming more common. Based upon an ongoing positive relationship between hospital, payer and/or business marketing efforts need to be continual and founded upon principles of the exchange relationship, where each side must be seen to benefit from the other.
Some hospitals have significant current capability, but others are just getting started. It is important to consider the basic prerequisites for creating and managing bundles of all types before competitive and/or time pressures grow too great to ignore, or negative financial consequences commence. Creating an ill-conceived bundle can result in both poor outcomes and financial loss. There is considerable preparation to be done and little time to waste.
The preparation for bundling (be it Medicare-related or private payer) presents an opportunity for all hospitals to gain critical experience with cost management, care coordination, post-acute care provider network development, increased physician involvement and clinical standardization. These are all vital disciplines in the continuing effort to create value in healthcare and position the hospital’s cardiac program for future success.
Editor’s note: John W. Meyer, MPH, FACHE, is a senior manager with the business consulting firm Charles Franc & Associates Inc. The company works exclusively in cardiovascular services with clients including hospitals and health systems, clinics, physician practices and healthcare-related firms. For additional information, including blogs specific to bundled pricing and Medicare’s new cardiac bundle, go to www.charlesfrancassociates.com.
Reference:
1. “Notice of proposed rulemaking for bundled payment models for high-quality, coordinated cardiac and hip fracture care.” U.S. Department of Health and Human Services, 2016-07-25, ([email protected]).


 April 10, 2026
April 10, 2026 









