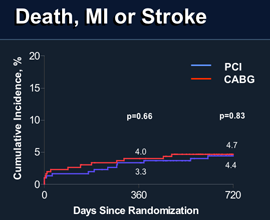
The rates of death, heart attack and stroke were equal for patients in the PRECOMBAT trial, regardless if they received a stent or CABG.
A study from a South Korean research team found that angioplasty with a sirolimus-eluting stent was non-inferior to coronary artery bypass surgery (CABG) in patients with unprotected left main coronary artery disease. Rates of death, heart attack, stroke and ischemia-driven target vessel revascularization (TVR) were all equal, according to research presented this week at the American College of Cardiology (ACC) Scientific Session in New Orleans.
“PCI [percutaneous coronary intervention] seems the same as CABG, however, the results were wide, so it is not a clinical mandate in the results,” said Seung-Jung Park, M.D., Ph.D., lead study author and professor of medicine at the University of Ulsan College of Medicine in Seoul, South Korea.
The trial follows decades of questioning among cardiovascular specialists about which procedure – CABG or angioplasty – yields better outcomes. While angioplasty is less invasive and requires a shorter recovery time, it is also associated with a greater need for repeat procedures and a reduced ability to fully revascularize patients with multivessel disease. Although numerous trials have been conducted comparing the two procedures, a lack of randomized clinical trials has left the question open to debate.
“In spite of higher revascularization after angioplasty, it can be a potential alternative if the two treatments have a similar risk of hard endpoints, such as death, heart attack or stroke,” Park said. “At the time this study was initiated, there was great enthusiasm about the outcomes of angioplasty, and as a result, off-label use rapidly spread without enough evidence. Therefore, initiation of a randomized study was urgent.”
Study Details
For the study, the researchers randomized 600 patients to receive either CABG (n = 300) or angioplasty with the sirolimus-eluting Cypher stent (manufactured by Cordis; n = 300). After the procedure, clinical followup was conducted at 30 days and six, nine and 12 months; angiographic followup was conducted from eight to 10 months for the angioplasty cohort.
The study’s primary outcome measure was a composite of major adverse cardiac or cerebrovascular events (MACCE) at 12 months that included: death from any cause, heart attack, stroke and ischemia-driven TVR.
The researchers found that angioplasty was not inferior to CABG for the primary outcome measure, with MACCE rates of 8.7 percent and 6.7 percent, respectively (p = 0.001; HR 1.29, 95 percent CI, 0.72 – 2.32). The rates of MACCE at 24 months were also comparable between the two groups, at 12.2 percent for angioplasty and 8.1 percent for CABG. A different composite of death, heart attack and stroke (which was used as a safety indicator) also showed similar outcomes at 24 months, at 4.4 percent for the angioplasty cohort and 4.7 percent in the CABG cohort (p = 0.83).
The research team did find a significant difference, however, in the rates of ischemia-driven TVR at 24 months. Specifically, 9 percent of patients in the angioplasty group experienced this individual outcome, compared with 4.2 percent in the CABG group (p = 0.022).
“Our study endpoints included safety and efficacy outcomes. The incidences of death, heart attack and stroke – which are indicators of safety and have a significant impact on mortality – were comparable,” Park said. “Although angioplasty did have a higher risk of TVR, this efficacy endpoint does not have a direct association with mortality and thus has a less significant implication than the safety outcomes. Therefore, we can conclude that angioplasty can be a feasible alternative to CABG surgery.”
In the angioplasty arm, intravascular ultrasound (IVUS) was used in 91 percent of patients to evaluate lesions and for vessel sizing. In patients with bifurcation lesions, a single-stent technique was employed in 87 percent of the cases.
In the surgical arm, left internal mammary arteries (LIMA) grafts were used in 233 of the 300 CABG patients.
Surgery May Still Be Best Option for Long-Term Outcomes
After the trial presentation, panelists compared this trial to the SYNTAX trial, which was a comparison of the Taxus stent vs. CABG. That trial slightly favored CABG. Three-year outcomes data from SYNTAX appear to show surgery has better durability without the need for repeat revascularization, which was required in a higher percentage of PCI patients, said panelist Bernard Gersh, MB, Ch.B. D.Phil., FRCP, FACC, Mayo Clinic College of Medicine, Division of Cardiovascular Diseases at Mayo Clinic.
"There does seem to be a divergence in MACCE rates as time goes on, especially in patients with two- and three-vessel disease,” said panelist Steven Bolling, M.D., a cardiac surgeon at the University of Michigan. He said data from the past three years seem to show CABG has better durability than PCI.
Panelist Gregg Stone, M.D., director of cardiovascular research and education, Cardiovascular Research Foundation, said PRECOMBAT had an improvement over SYNTAX in that IVUS was used in the majority of cases to help decide if stenting was necessary and for more accurate stent sizing to avoid malapposition. This may have led to better outcomes for PCI in this trial compared to SYNTAX.
The PRECOMBAT study was supported by funds from the Cardiovascular Research Foundation (Seoul), Cordis and the Health 21 Research and Development Project (Ministry of Health and Welfare, South Korea). Park had no disclosures.
This study was published this week in the New England Journal of Medicine (NEJM).


 May 05, 2026
May 05, 2026 









