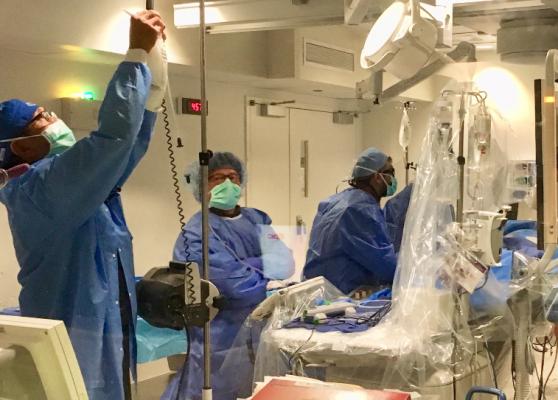
Avoiding high-risk PCI procedures does not improve hospital scores according to a study presented at SCAI 2021. CTO procedure at Henry Ford Hospital, Detroit. Photo by Dave Fornell.
May 5, 2021 — A late-breaking study presented at the Society for Cardiovascular Angiography and Interventions (SCAI) 2021 meeting looked at hospital-level percutaneous coronary intervention (PCI) performance with simulated risk avoidance strategies and found this might not improve performance.
"Any individual hospital seeking to improve their performance, there is no guarantee that practicing systematic risk-avoidance will improve the measured quality of a PCI program, and may in fact worsen it," explained Ashwin Nathan M.D., a cardiology fellow at the Hospital of the University of Pennsylvania, who presented the study.
He said the study data support offering PCI to appropriate candidates regardless of calculated pre-procedural risk.
The study was conducted because it is believed some PCI operators may avoid high-risk cases so they can to limit the effect of these cases on performance metrics. Nathan said the effect of such a strategy on individual hospital performance metrics is uncertain. This study simulated the effects of systematic risk avoidance on risk-adjusted post-PCI mortality.
He said hospitals, especially in states that require public reporting on outcomes, may shy away from high-risk patients or complex procedures in an effort to improve these publicly reported scores.
Researchers identified all adult patients who underwent PCI at a participating hospital in the National Cardiovascular Data Registry CathPCI registry between January 2017 and December 2017. Risk-adjusted mortality rates were calculated for each hospital. They then simulated a systematic risk-avoidance strategy of eliminating the highest predicted risk cases (top 10%) for each hospital, then recalculating risk-adjusted mortality rates.
The study included 1,565 hospitals in the analysis. Of these, 883 (56.4%) hospitals reduced their risk-adjusted mortality rate, but 610 (39%) hospitals increased their risk-adjusted mortality rate. Hospitals changed their risk-adjusted mortality rate by -0.14% on average with this strategy.
There were no significant differences in the patient or procedural characteristics among hospitals which improved compared with those that worsened.
The study authors included: Ashwin Nathan, M.D.; Sameed Khatana, M.D., MPH; Elias Dayoub, M.D., MPP; Lauren Eberly, M.D., MPH; Paul Fiorilli, M.D.; Alexander Fanaroff, M.D.; Peter Groeneveld, M.D., MS; and Jay S. Giri, M.D., FSCAI, all from the Hospital of the University of Pennsylvania. Stephen Waldo, M.D., University of Colorado Anschutz Medical Campus; Robert W. Yeh, M.D., FSCAI, Beth Israel Deaconess Medical Center; Sunil V. Rao, M.D., FSCAI, and Adam Nelson, MBBS, Duke University Hospital; and Pratik Manandhar, MS, Daniel Wojdyla, Ph.D., and Tracy Yu-Ping Wang, M.D., from the Duke Clinical Research Institute.
Watch the VIDEO: Avoiding Higher Risk Cath Lab Patients May Not Improve Outcomes Scores — Interview with Ashwin Nathan M.D.


 April 10, 2026
April 10, 2026 









